Real-Time VR Enhances View and Treatment Options in IR
|
By MedImaging International staff writers Posted on 05 Apr 2019 |
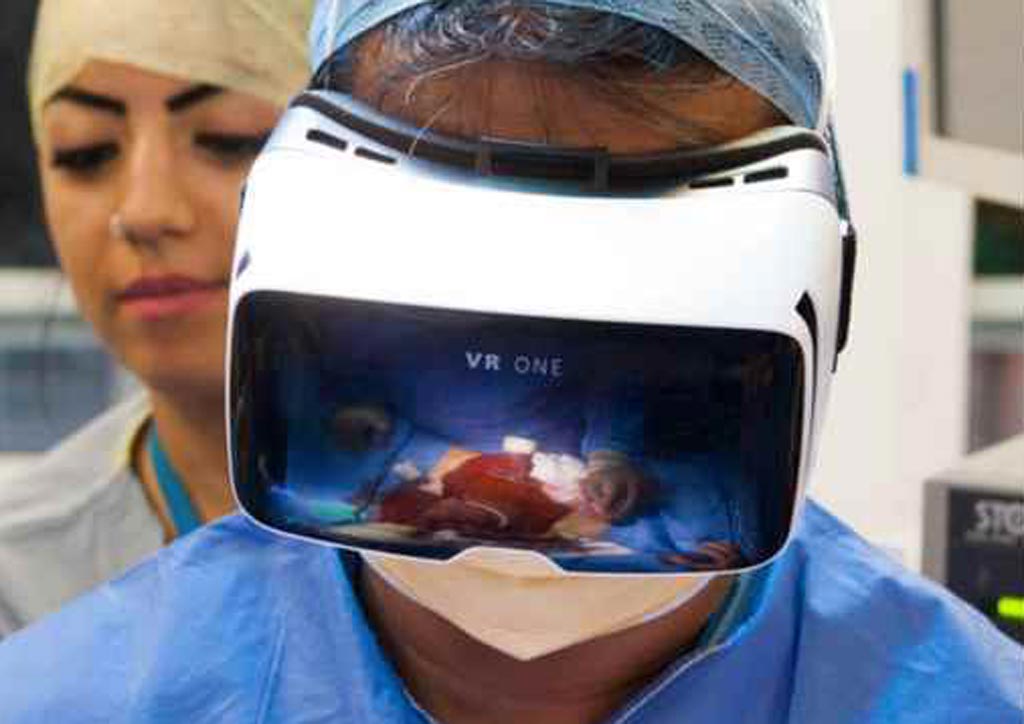
Image: New research suggests virtual reality options could enable interventional radiologists to improve treatments using RT 3D images from inside a patient’s blood vessels (Photo courtesy of Techmaish).
New research presented at the Society of Interventional Radiology’s 2019 Annual Scientific Meeting shows that immersive virtual reality (VR) could enable interventional radiologists to improve treatments using real-time 3D images from inside a patient’s blood vessels. The interactive technology could provide faster, more efficient treatment, with less radiation exposure and greater precision, ease and confidence.
The researchers conducted a study to demonstrate the feasibility of using a catheter with electromagnetic sensors projected onto a VR headset to see and steer the catheter through the anatomy to certain blood vessels. Using a CT angiography scan, they created a 3D printed model and a holographic image of blood vessels in a patient’s abdomen and pelvis. A team of radiologists guided hi-tech catheters through the 3D printed model while the tracking system showed the image from the catheter through the VR headset. They compared the time taken to steer the catheter from the entry point of the femoral artery to three different targeted vessels versus the time the process took using conventional fluoroscopic guidance, as well as the time taken in similar real-life clinical angiographic procedures.
In 18 simulated procedures, the researchers found the mean time to reach the three targeted vessels using VR was much lower than in fluoroscopy, the standard practice that uses an x-ray image. In the first vessel, VR took 17.6 seconds versus 70.3 seconds using the standard practice on the model and 171.2 seconds in the real-life procedure. With the improved efficiency, the researchers believe that VR technology will create safer treatments by reducing the amount of radiation exposure to both patient and physician, as well as increase access to IR treatments. The researchers also surveyed the practitioners who had tried the technology who reported that VR improved the ease, precision and efficiency of the treatment. Additionally, the users said they felt more confident in their abilities.
“Virtual reality will change how we look at a patient’s anatomy during an IR treatment. This technology will allow physicians to travel inside a patient’s body instead of relying solely on 2D, black and white images,” said Wayne Monsky, M.D, PhD, a professor of radiology at the University of Washington and lead author of the study. “Currently, the life-saving potential of IR is limited to hospitals and areas with the resources to invest in image-guided technology. There are three billion people worldwide in rural areas who don't have this access. This technology could allow for portability and accessibility so that these procedures are brought to rural areas using nothing more than a suitcase.”
The researchers conducted a study to demonstrate the feasibility of using a catheter with electromagnetic sensors projected onto a VR headset to see and steer the catheter through the anatomy to certain blood vessels. Using a CT angiography scan, they created a 3D printed model and a holographic image of blood vessels in a patient’s abdomen and pelvis. A team of radiologists guided hi-tech catheters through the 3D printed model while the tracking system showed the image from the catheter through the VR headset. They compared the time taken to steer the catheter from the entry point of the femoral artery to three different targeted vessels versus the time the process took using conventional fluoroscopic guidance, as well as the time taken in similar real-life clinical angiographic procedures.
In 18 simulated procedures, the researchers found the mean time to reach the three targeted vessels using VR was much lower than in fluoroscopy, the standard practice that uses an x-ray image. In the first vessel, VR took 17.6 seconds versus 70.3 seconds using the standard practice on the model and 171.2 seconds in the real-life procedure. With the improved efficiency, the researchers believe that VR technology will create safer treatments by reducing the amount of radiation exposure to both patient and physician, as well as increase access to IR treatments. The researchers also surveyed the practitioners who had tried the technology who reported that VR improved the ease, precision and efficiency of the treatment. Additionally, the users said they felt more confident in their abilities.
“Virtual reality will change how we look at a patient’s anatomy during an IR treatment. This technology will allow physicians to travel inside a patient’s body instead of relying solely on 2D, black and white images,” said Wayne Monsky, M.D, PhD, a professor of radiology at the University of Washington and lead author of the study. “Currently, the life-saving potential of IR is limited to hospitals and areas with the resources to invest in image-guided technology. There are three billion people worldwide in rural areas who don't have this access. This technology could allow for portability and accessibility so that these procedures are brought to rural areas using nothing more than a suitcase.”
Latest Imaging IT News
- Interactive AI Tool Supports Explainable Lung Nodule Assessment
- Breast Imaging Software Enhances Visualization and Tissue Characterization in Challenging Cases
- New Google Cloud Medical Imaging Suite Makes Imaging Healthcare Data More Accessible
- Global AI in Medical Diagnostics Market to Be Driven by Demand for Image Recognition in Radiology
- AI-Based Mammography Triage Software Helps Dramatically Improve Interpretation Process
- Artificial Intelligence (AI) Program Accurately Predicts Lung Cancer Risk from CT Images
- Image Management Platform Streamlines Treatment Plans
- AI-Based Technology for Ultrasound Image Analysis Receives FDA Approval
- AI Technology for Detecting Breast Cancer Receives CE Mark Approval
- Digital Pathology Software Improves Workflow Efficiency
Channels
Radiography
view channel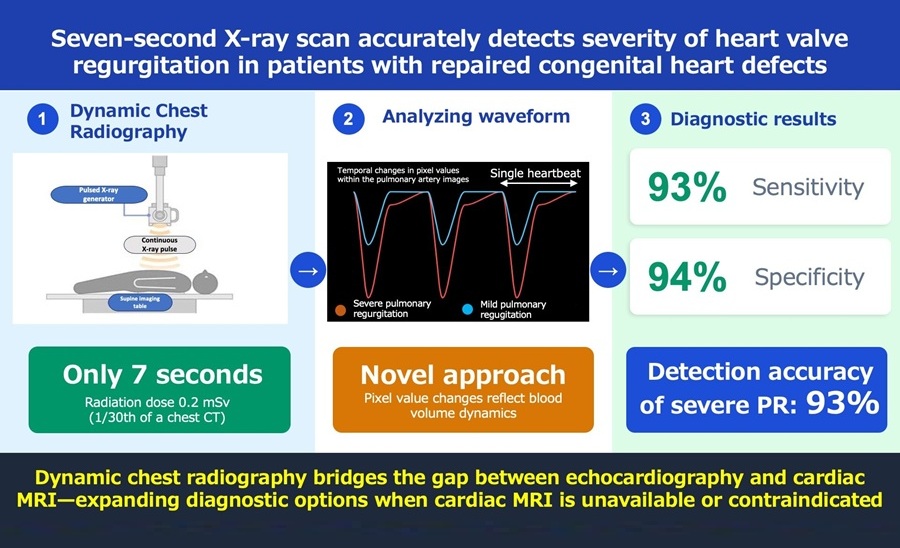
Rapid X-Ray Test Quantifies Pulmonary Regurgitation After Tetralogy of Fallot Repair
Tetralogy of Fallot is the most common cyanotic congenital heart defect and can leave patients with pulmonary valve regurgitation, a backward flow of blood into the right ventricle after repair.... Read more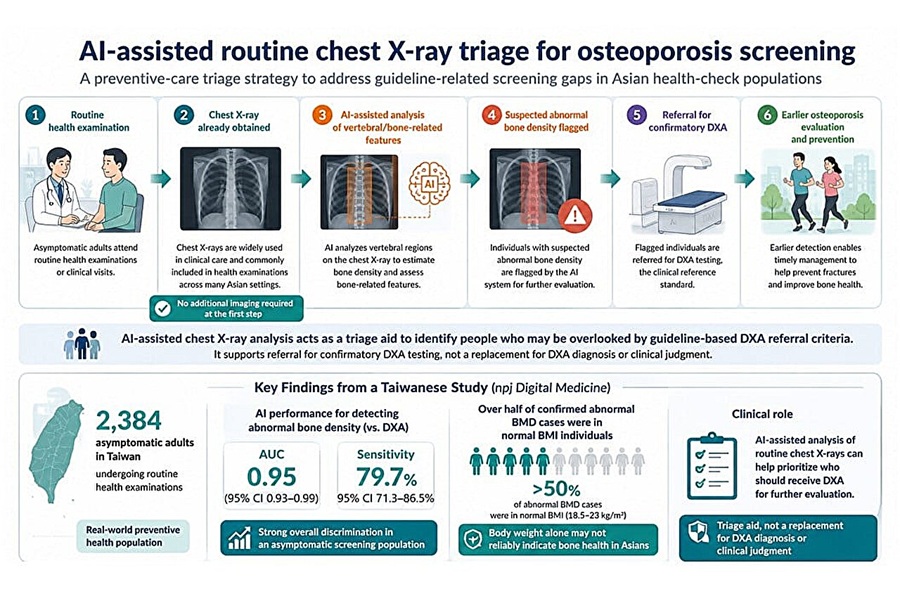
AI Tool Flags Osteoporosis Risk from Routine Chest X-Rays
Osteoporosis is a progressive loss of bone density that is often silent until a fracture occurs. Current screening frameworks concentrate on older women and select high-risk groups. Many men, younger adults,... Read moreMRI
view channel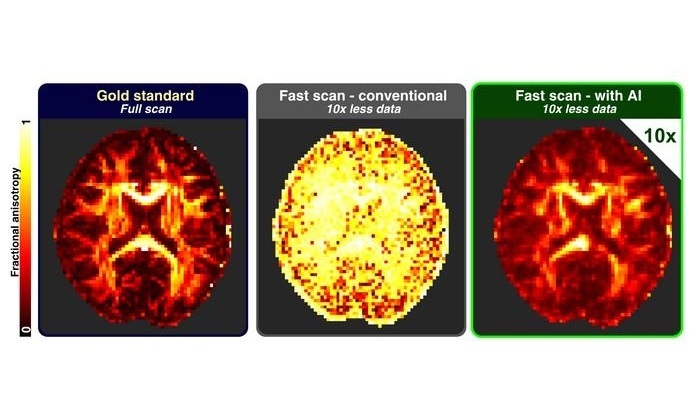
AI Approach Could Shorten Advanced Brain MRI Scans by Up to 90%
Long acquisition times for advanced brain magnetic resonance imaging (MRI) can limit access, extend waiting lists, and disrupt clinical workflows. Reducing data requirements without sacrificing image fidelity... Read more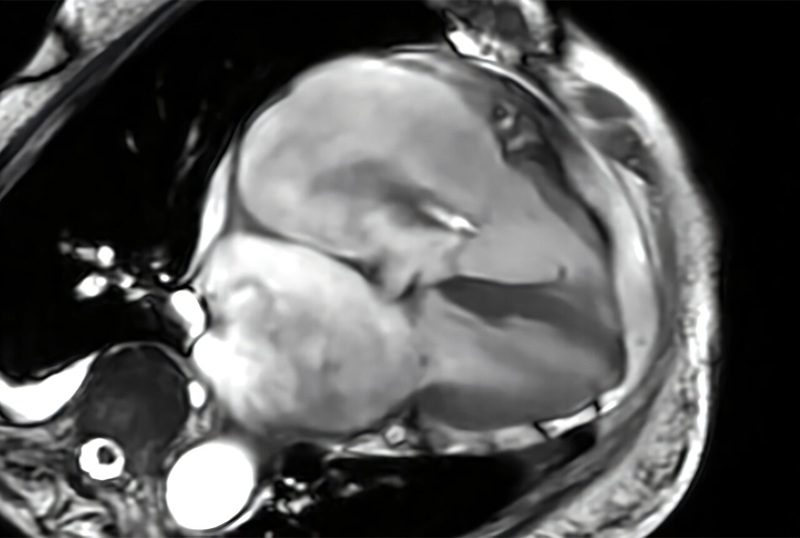
Cardiac MRI Measure Improves Risk Prediction in Tricuspid Regurgitation
Tricuspid regurgitation, in which blood flows back from the right ventricle into the right atrium, can lead to progressive right-sided heart failure. Clinicians need reliable ways to gauge severity and... Read moreUltrasound
view channelAI Robotic Ultrasound System Automates Echocardiography and Improves Consistency
Echocardiography, an ultrasound examination of the heart, is central to diagnosing and managing cardiovascular disease. Many services struggle with limited availability of skilled sonographers, variable... Read more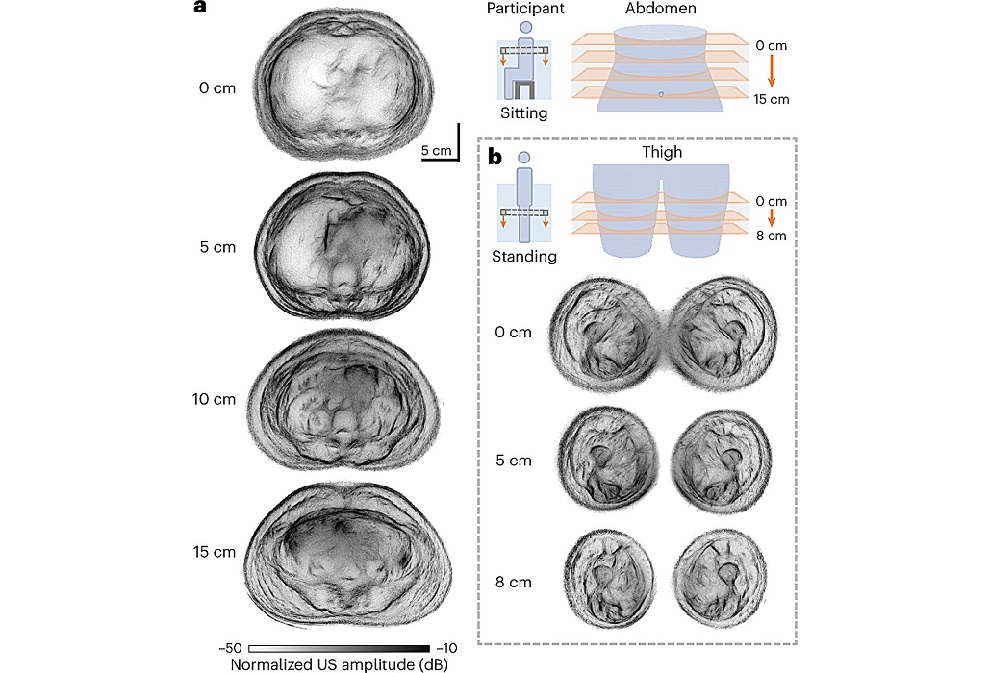
Whole Cross-Section Ultrasound System Enables Operator-Independent Imaging
Conventional ultrasound is central to bedside imaging but is limited by a narrow field of view and operator variability. Comprehensive cross-sectional assessment typically requires computed tomography... Read moreNuclear Medicine
view channel![Image: (A-C) Representative whole-body maximum-intensity projection images and regional fused PET/CT images from three histologically confirmed osteosarcoma patients who underwent paired [68Ga]Ga-B7-H3-BCH PET/CT and 18F-FDGE PET/CT within 7 days. (D) Multimodal imaging evaluation of patient 3, including X-ray, MRI (T2-weighted imaging, T2WI), CT, and B7-H3 PET/CT. (Photo courtesy of SNMMI) Image: (A-C) Representative whole-body maximum-intensity projection images and regional fused PET/CT images from three histologically confirmed osteosarcoma patients who underwent paired [68Ga]Ga-B7-H3-BCH PET/CT and 18F-FDGE PET/CT within 7 days. (D) Multimodal imaging evaluation of patient 3, including X-ray, MRI (T2-weighted imaging, T2WI), CT, and B7-H3 PET/CT. (Photo courtesy of SNMMI)](https://globetechcdn.com/mobile_medicalimaging/images/stories/articles/article_images/2026-06-07/294811110_image_1.jpg)
Targeted PET Platform Guides Osteosarcoma Resection and Margin Verification
Osteosarcoma, an aggressive primary bone cancer that mainly affects children and adolescents, demands wide excision to prevent local recurrence. Surgeons must achieve negative margins while preserving... Read more
Portable PET System Enables Real-Time Bedside Guidance for Biopsies and Ablations
Interventional radiology procedures typically rely on ultrasound, X-ray fluoroscopy, or computed tomography for image guidance. These modalities visualize anatomy but offer limited molecular information,... Read moreGeneral/Advanced Imaging
view channelNew SPECT/CT Method Differentiates Inflammation from Fibrosis in Interstitial Lung Disease
Interstitial lung disease (ILD) encompasses more than 200 disorders that inflame or scar the lung interstitium and can lead to progressive respiratory failure. Determining whether active inflammation is... Read more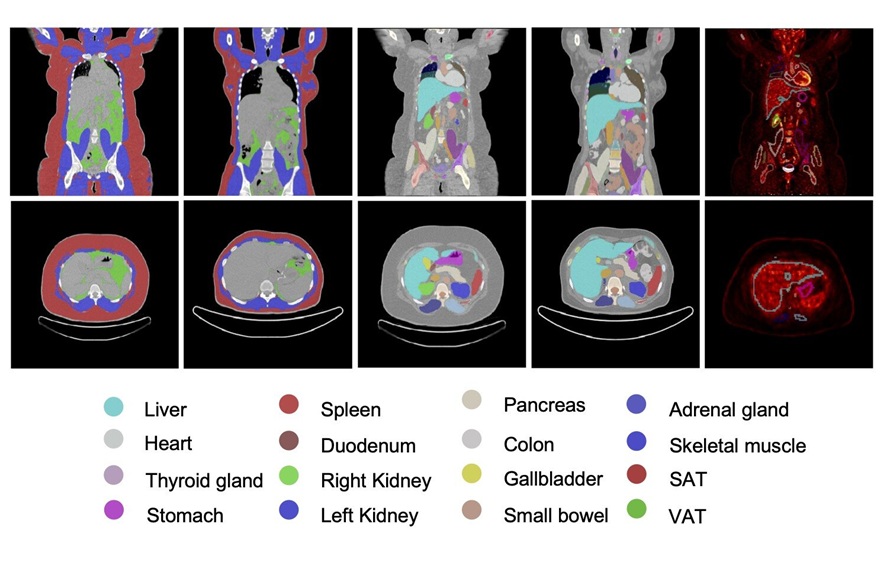
Whole-Body PET/CT Tracks Metabolic Changes After Bariatric Surgery
Obesity surgery improves weight and comorbidity profiles, yet clinicians lack tools to monitor organ-level metabolic recovery after the procedure. A clear view of systemic changes could refine follow-up... Read moreImaging IT
view channel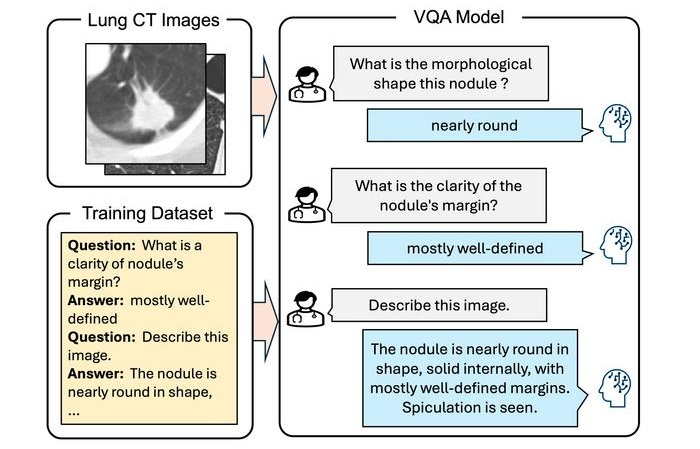
Interactive AI Tool Supports Explainable Lung Nodule Assessment
Lung cancer is a leading cause of cancer mortality, and timely characterization of pulmonary nodules on chest computed tomography (CT) is essential for directing care. Interpreting nodule morphology demands... Read more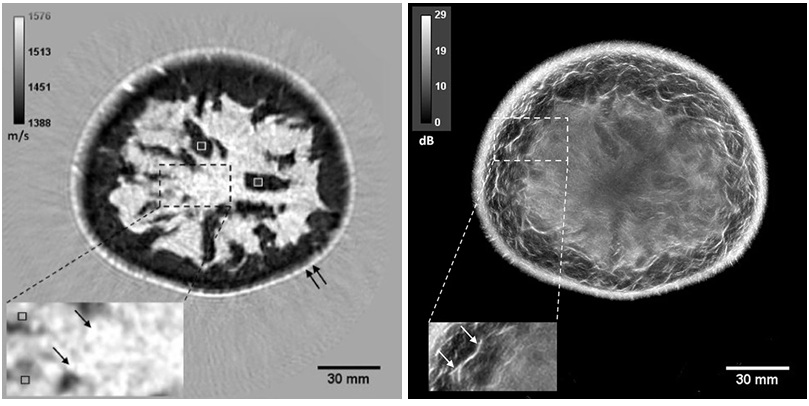
Breast Imaging Software Enhances Visualization and Tissue Characterization in Challenging Cases
Breast imaging can be particularly challenging in cases involving small breasts or implants, where image reconstruction and tissue characterization may be limited. Clinicians also need reproducible analysis... Read more
New Google Cloud Medical Imaging Suite Makes Imaging Healthcare Data More Accessible
Medical imaging is a critical tool used to diagnose patients, and there are billions of medical images scanned globally each year. Imaging data accounts for about 90% of all healthcare data1 and, until... Read more