CT Matches MRI for Late-Window Stroke Evaluation
|
By MedImaging International staff writers Posted on 18 Feb 2019 |
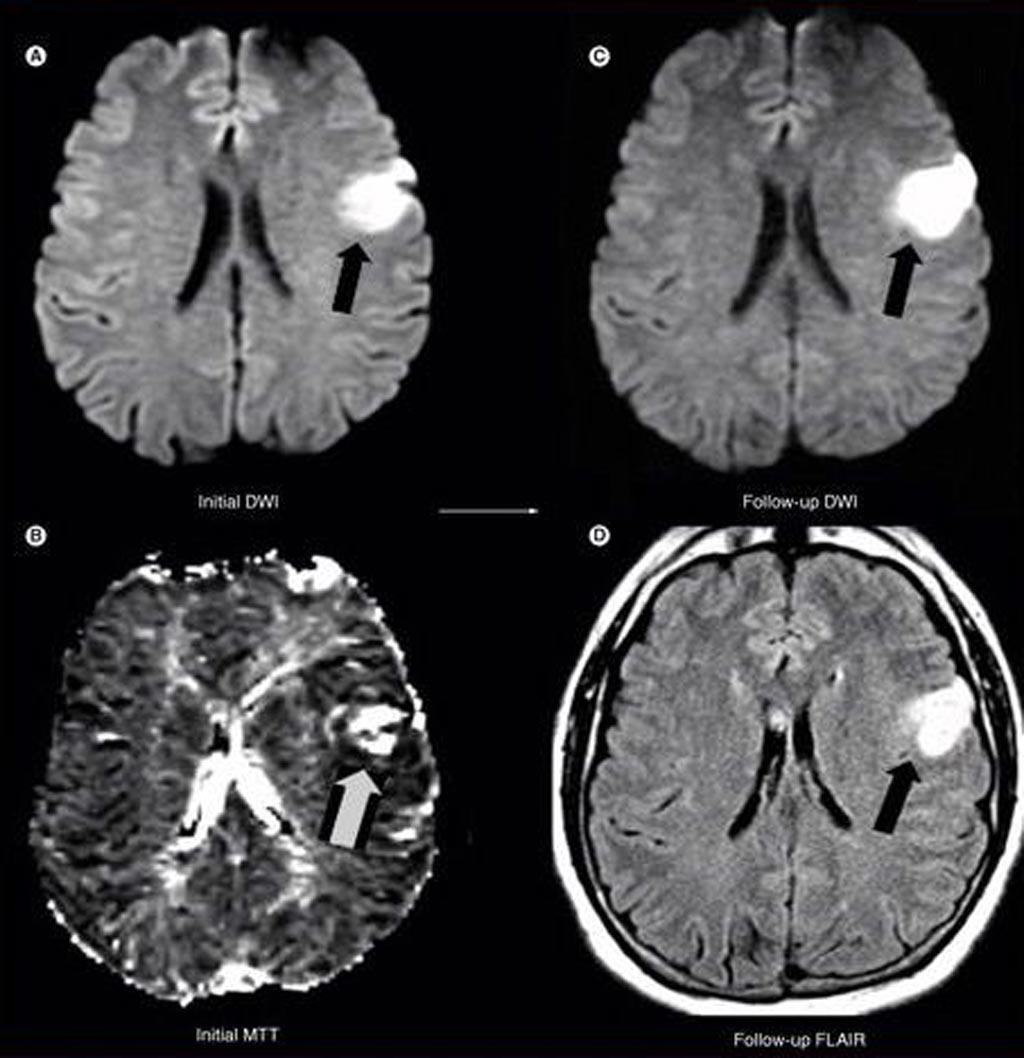
Image: As part of a new study, researchers found that for stroke patients treated 3-6 hours after onset with intravenous tPA, baseline MRI findings can identify subgroups that are likely to benefit from reperfusion therapies and can potentially identify subgroups that are unlikely to benefit or may be harmed (Photo courtesy of Medscape).
Stroke patients who underwent endovascular therapy had similar improvement following treatment, regardless of the perfusion imaging used to confirm their eligibility for surgical procedures, according to a new study.
Researchers Stanford University School of Medicine (CA, USA) and the University of Texas Health Science Center (UTHSCSA; Houston, USA) conducted a study to evaluate whether the imaging-based selection criteria--computerized tomography (CT) or magnetic resonance imaging (MRI)--used prior to endovascular therapy showed comparable outcome rates and treatment benefits. The trial comprised 38 stroke centers in the United States and 182 patients (median age 70 years, 51% women) with stroke treated within 6 to 16 hours from last known well.
All patients underwent either perfusion MRI or perfusion CT to confirm that they had sufficient amounts of salvageable tissue to make surgery viable. The results revealed that endovascular therapy benefit was uniform across patients of various ages, regardless of the symptom severity, time to treatment, location of occlusion, and type of perfusion imaging they underwent prior to endovascular therapy, indicating that either modality could be used for patient selection. The study was published on January 28, 2019, in JAMA Neurology.
"Endovascular therapy in the 6-16-hour time window in patients with evidence of salvageable tissue on brain perfusion imaging is beneficial in a broad patient population, including patients who have mild or severe symptoms, and who are selected by CT or MRI,” concluded lead author Maarten Lansberg, PhD, of Stanford University, and colleagues. “These results have health care implications indicating transferring potential candidates for late-window thrombectomy is associated with substantial clinical benefits, and should be encouraged.”
Rapid and effective revascularization is the mainstay of acute ischemic stroke treatment. Until recently, intravenous recombinant tissue-type plasminogen activator (r-tPA) was the only established therapeutic option. New studies have proven the benefit of endovascular treatment, and thrombectomy with stent retrievers is now recommended as the standard of care for acute ischemic strokes with a proximal large vessel occlusion in the anterior circulation.
Related Links:
Stanford University School of Medicine
University of Texas Health Science Center
Researchers Stanford University School of Medicine (CA, USA) and the University of Texas Health Science Center (UTHSCSA; Houston, USA) conducted a study to evaluate whether the imaging-based selection criteria--computerized tomography (CT) or magnetic resonance imaging (MRI)--used prior to endovascular therapy showed comparable outcome rates and treatment benefits. The trial comprised 38 stroke centers in the United States and 182 patients (median age 70 years, 51% women) with stroke treated within 6 to 16 hours from last known well.
All patients underwent either perfusion MRI or perfusion CT to confirm that they had sufficient amounts of salvageable tissue to make surgery viable. The results revealed that endovascular therapy benefit was uniform across patients of various ages, regardless of the symptom severity, time to treatment, location of occlusion, and type of perfusion imaging they underwent prior to endovascular therapy, indicating that either modality could be used for patient selection. The study was published on January 28, 2019, in JAMA Neurology.
"Endovascular therapy in the 6-16-hour time window in patients with evidence of salvageable tissue on brain perfusion imaging is beneficial in a broad patient population, including patients who have mild or severe symptoms, and who are selected by CT or MRI,” concluded lead author Maarten Lansberg, PhD, of Stanford University, and colleagues. “These results have health care implications indicating transferring potential candidates for late-window thrombectomy is associated with substantial clinical benefits, and should be encouraged.”
Rapid and effective revascularization is the mainstay of acute ischemic stroke treatment. Until recently, intravenous recombinant tissue-type plasminogen activator (r-tPA) was the only established therapeutic option. New studies have proven the benefit of endovascular treatment, and thrombectomy with stent retrievers is now recommended as the standard of care for acute ischemic strokes with a proximal large vessel occlusion in the anterior circulation.
Related Links:
Stanford University School of Medicine
University of Texas Health Science Center
Latest MRI News
- Blood-Brain Barrier Imaging Adds Risk Insight to Standard Stroke MRI
- AI MRI Tool Quantifies Muscle Fat to Assess Cardiometabolic Risk
- Advanced MRI Visualizes CSF Motion Changes After Mild Traumatic Brain Injury
- MRI Tool Enables Long-Term Tracking of Transplanted Cardiac Cells
- MRI-Based AI Tool Supports Differentiation of Parkinsonian Syndromes
- MRI-Derived Biomarker Improves Risk Stratification in Glioblastoma
- Combined Imaging Approach Identifies Cause of Heart Attack without Coronary Blockage
- Advanced MRI System Detects Impaired Cardiac Oxygen Use in Minutes
- AI-Enhanced MRI Improves Image Quality in Arrhythmia Patients
- Ultra-Detailed Brain Atlas Enhances Early Detection of Neurological Disorders
- Study Finds Advanced Imaging Significantly Reduces Unnecessary Prostate Biopsies
- New Material Boosts MRI Image Quality
- AI Model Reads and Diagnoses Brain MRI in Seconds
- MRI Scan Breakthrough to Help Avoid Risky Invasive Tests for Heart Patients
- MRI Scans Reveal Signature Patterns of Brain Activity to Predict Recovery from TBI
- Novel Imaging Approach to Improve Treatment for Spinal Cord Injuries
Channels
Radiography
view channel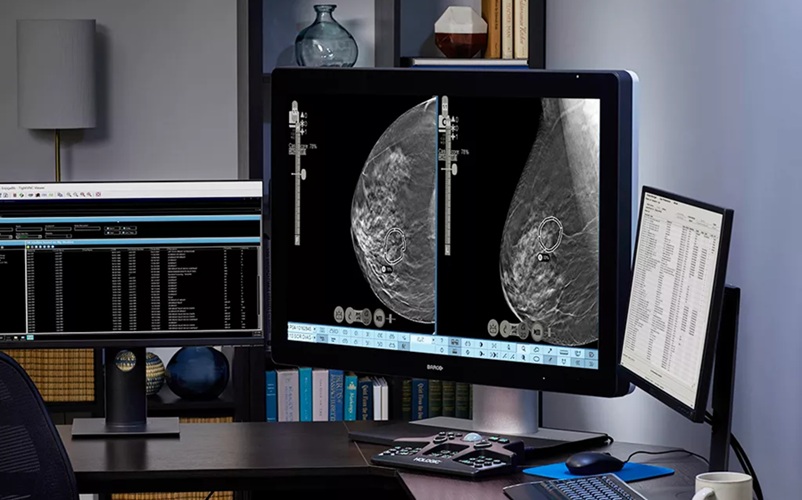
AI Detection Tool Improves Identification of Lobular Breast Cancer
Breast cancer screening seeks early detection, yet some subtypes remain difficult to visualize on mammography, risking delayed diagnosis. On average, 1 in 20 women worldwide will develop breast cancer,... Read more
New Contrast Agent Enables Low-Dose X-Ray Joint Imaging
X-ray imaging offers limited visualization of soft tissues like cartilage, complicating evaluation of joint pain and degenerative disease. Clinicians often rely on joint-space narrowing as a proxy for... Read moreUltrasound
view channelAI Robotic Ultrasound System Automates Echocardiography and Improves Consistency
Echocardiography, an ultrasound examination of the heart, is central to diagnosing and managing cardiovascular disease. Many services struggle with limited availability of skilled sonographers, variable... Read more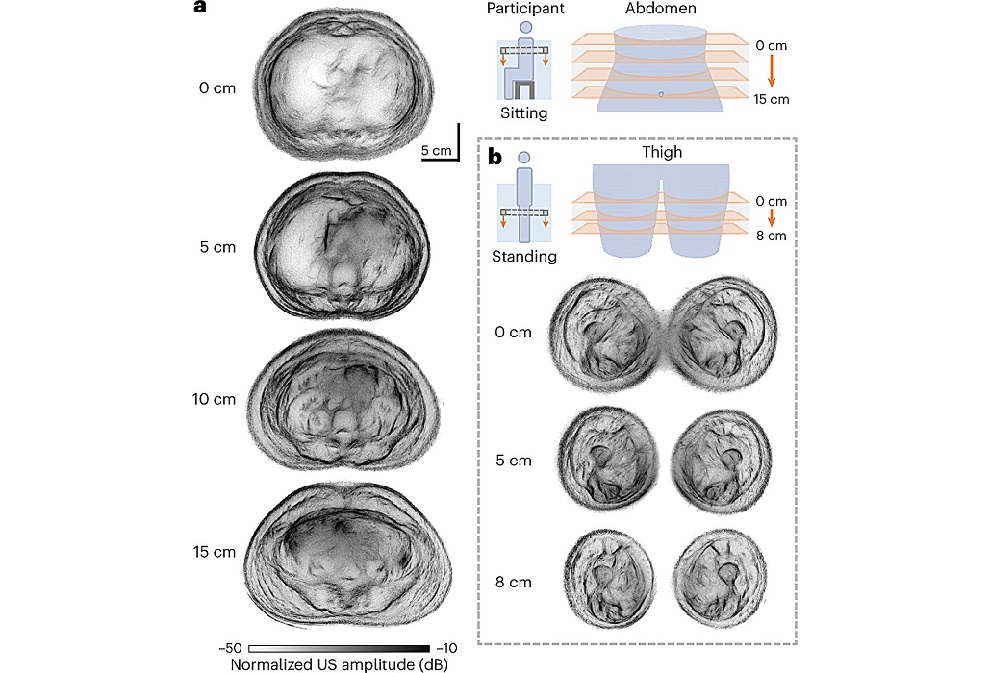
Whole Cross-Section Ultrasound System Enables Operator-Independent Imaging
Conventional ultrasound is central to bedside imaging but is limited by a narrow field of view and operator variability. Comprehensive cross-sectional assessment typically requires computed tomography... Read moreNuclear Medicine
view channelMR-Guided Cardiac Mapping System Enables Radiation-Free Procedures
Cardiac electrophysiology procedures are typically guided by X-ray fluoroscopy, which limits soft-tissue visualization and exposes patients and clinical staff to ionizing radiation. Real-time mapping that... Read more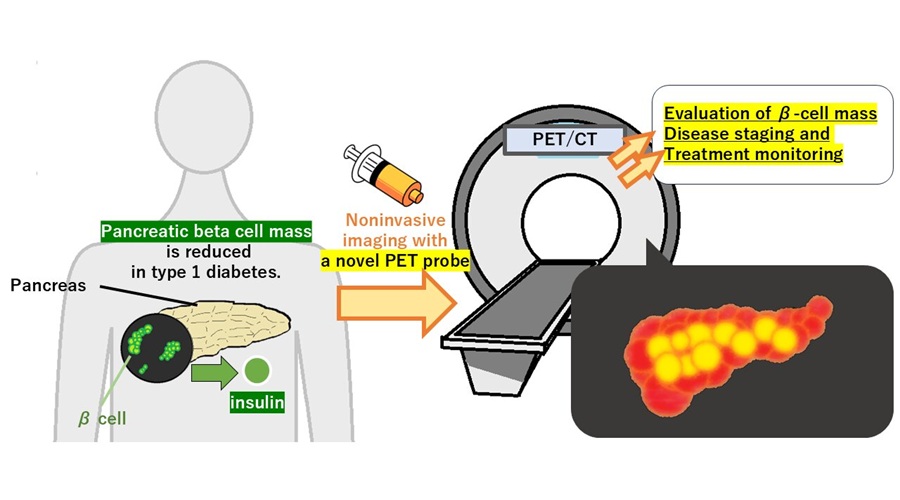
PET Tracer Enables Noninvasive Measurement of Beta Cell Mass
Type 1 diabetes is an autoimmune disease in which the immune system destroys insulin-producing pancreatic beta cells. Loss of these cells destabilizes glucose control and drives complications.... Read more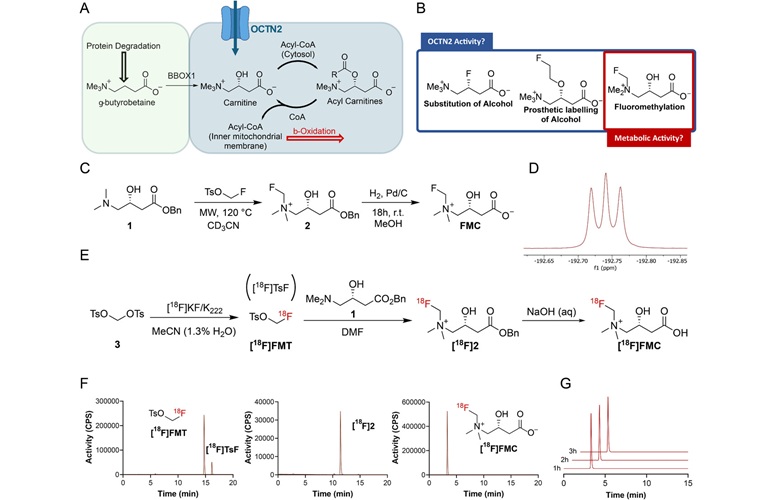
New Imaging Tool Sheds Light on Tumor Fat Metabolism
Rapidly growing tumors reprogram metabolism to meet high energy demands. While many cancers preferentially consume glucose, lipid utilization by malignant cells is difficult to measure in living subjects.... Read more
Radiopharmaceutical Molecule Marker to Improve Choice of Bladder Cancer Therapies
Targeted cancer therapies only work when tumor cells express the specific molecular structures they are designed to attack. In urothelial carcinoma, a common form of bladder cancer, the cell surface protein... Read moreGeneral/Advanced Imaging
view channel
Molecular Imaging Agent Shows Promise for Endometriosis Detection and Monitoring
Diagnosing endometriosis remains challenging, particularly for superficial peritoneal endometriosis, the most common subtype, which is often missed on conventional imaging and typically requires laparoscopic... Read more
Automated AI Tool Detects Early Pancreatic Cancer on Routine CT
Pancreatic ductal adenocarcinoma, the most common form of pancreatic cancer, is often diagnosed at a late stage and carries poor survival because early disease produces few symptoms and subtle tissue changes... Read moreImaging IT
view channel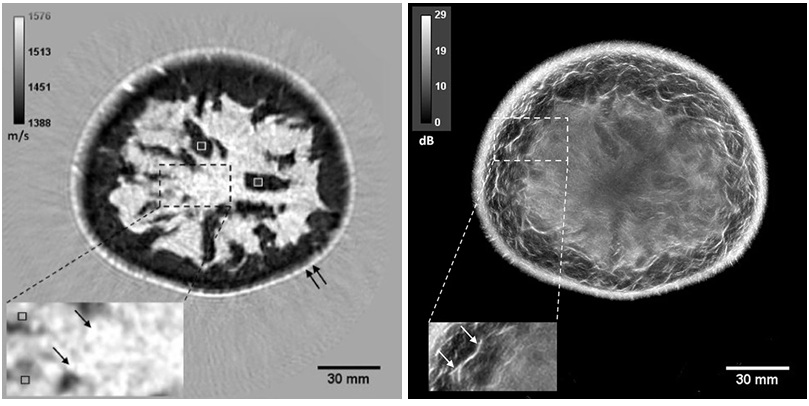
Breast Imaging Software Enhances Visualization and Tissue Characterization in Challenging Cases
Breast imaging can be particularly challenging in cases involving small breasts or implants, where image reconstruction and tissue characterization may be limited. Clinicians also need reproducible analysis... Read more
New Google Cloud Medical Imaging Suite Makes Imaging Healthcare Data More Accessible
Medical imaging is a critical tool used to diagnose patients, and there are billions of medical images scanned globally each year. Imaging data accounts for about 90% of all healthcare data1 and, until... Read more
Global AI in Medical Diagnostics Market to Be Driven by Demand for Image Recognition in Radiology
The global artificial intelligence (AI) in medical diagnostics market is expanding with early disease detection being one of its key applications and image recognition becoming a compelling consumer proposition... Read moreIndustry News
view channel
Nuclear Medicine Set for Continued Growth Driven by Demand for Precision Diagnostics
Clinical imaging services face rising demand for precise molecular diagnostics and targeted radiopharmaceutical therapy as cancer and chronic disease rates climb. A new market analysis projects rapid expansion... Read more