Functional Brain PET Imaging Effectively Forecasts Which Vegetative Patients Can Recover Consciousness
|
By MedImaging International staff writers Posted on 27 Apr 2014 |
Image: A functional brain imaging technique known as positron emission tomography (PET) is a promising tool for determining which severely brain damaged individuals in vegetative states have the potential to recover consciousness (Photo courtesy of sonap / Fotolia).
Positron emission tomography (PET) has the potential for determining which brain damaged individuals in vegetative states have the potential to recover consciousness, according to new research.
The study’s findings were published online April 16, 2014, in the Lancet. It is the first time that researchers have assessed the diagnostic accuracy of functional brain imaging techniques in clinical practice. “Our findings suggest that PET imaging can reveal cognitive processes that aren’t visible through traditional bedside tests, and could substantially complement standard behavioral assessments to identify unresponsive or ‘vegetative’ patients who have the potential for long-term recovery,” stated study leader Prof. Steven Laureys, from the University of Liége (Belgium).
In severely brain-damaged individuals, judging the level of consciousness has proved challenging. Traditionally, bedside clinical examinations have been used to decide whether patients are in a minimally conscious state (MCS), in which there is some evidence of awareness and response to stimuli, or are in a vegetative state (VS) also known as unresponsive wakefulness syndrome, where there is neither, and the chance of recovery is much lower. But up to 40% of patients are misdiagnosed using these scans.
“In patients with substantial cerebral edema, prediction of outcome on the basis of standard clinical examination and structural brain imaging is probably little better than flipping a coin,” wrote Jamie Sleigh from the University of Auckland (New Zealand), and Catherine Warnaby from the University of Oxford (UK), in a linked comment.
The study evaluated whether two new functional brain imaging techniques—PET with the imaging agent fluorodeoxyglucose (FDG) and functional MRI (fMRI) during mental imagery tasks—could differentiate between vegetative and MCS in 126 patients with severe brain injury (81 in a MCS, 41 in a VS, and four with locked-in syndrome—a behaviorally unresponsive but conscious control group) referred to the University Hospital of Liége, from across Europe. The researchers then compared their results with the well-established standardized Coma Recovery Scale-Revised (CSR-R) behavioral test, considered the most confirmed and sensitive technique for discriminating very low awareness.
FDG-PET was better overall than fMRI in differentiating conscious from unconscious patients. Mental imagery fMRI was less sensitive at diagnosis of a MCS than FDG-PET (45% vs. 93%), and had less agreement with behavioral CRS-R scores than FDG-PET (63% vs. 85%). FDG-PET was about 74% accurate in predicting the extent of recovery within the next year, compared with 56% for fMRI.
Significantly, one-third of the 36 patients diagnosed as behaviorally unresponsive on the CSR-R test who were scanned with FDG-PET showed brain activity consistent with the presence of some consciousness. Nine patients in this group consequently recovered a reasonable level of consciousness.
According to Prof. Laureys, “We confirm that a small but substantial proportion of behaviorally unresponsive patients retain brain activity compatible with awareness. Repeated testing with the CRS-R complemented with a cerebral FDG-PET examination provides a simple and reliable diagnostic tool with high sensitivity towards unresponsive but aware patients. fMRI during mental tasks might complement the assessment with information about preserved cognitive capability, but should not be the main or sole diagnostic imaging method.”
The authors noted that the study was conducted in a specialist unit focusing on the diagnostic neuroimaging of disorders of consciousness and therefore deployment might be more challenging in less specialist units.
Commenting on the study Drs. Sleigh and Warnaby added, “From these data, it would be hard to sustain a confident diagnosis of unresponsive wakefulness syndrome solely on behavioral grounds, without PET imaging for confirmation ... [This] work serves as a signpost for future studies. Functional brain imaging is expensive and technically challenging, but it will almost certainly become cheaper and easier. In the future, we will probably look back in amazement at how we were ever able to practice without it.”
Related Links:
University of Liége
The study’s findings were published online April 16, 2014, in the Lancet. It is the first time that researchers have assessed the diagnostic accuracy of functional brain imaging techniques in clinical practice. “Our findings suggest that PET imaging can reveal cognitive processes that aren’t visible through traditional bedside tests, and could substantially complement standard behavioral assessments to identify unresponsive or ‘vegetative’ patients who have the potential for long-term recovery,” stated study leader Prof. Steven Laureys, from the University of Liége (Belgium).
In severely brain-damaged individuals, judging the level of consciousness has proved challenging. Traditionally, bedside clinical examinations have been used to decide whether patients are in a minimally conscious state (MCS), in which there is some evidence of awareness and response to stimuli, or are in a vegetative state (VS) also known as unresponsive wakefulness syndrome, where there is neither, and the chance of recovery is much lower. But up to 40% of patients are misdiagnosed using these scans.
“In patients with substantial cerebral edema, prediction of outcome on the basis of standard clinical examination and structural brain imaging is probably little better than flipping a coin,” wrote Jamie Sleigh from the University of Auckland (New Zealand), and Catherine Warnaby from the University of Oxford (UK), in a linked comment.
The study evaluated whether two new functional brain imaging techniques—PET with the imaging agent fluorodeoxyglucose (FDG) and functional MRI (fMRI) during mental imagery tasks—could differentiate between vegetative and MCS in 126 patients with severe brain injury (81 in a MCS, 41 in a VS, and four with locked-in syndrome—a behaviorally unresponsive but conscious control group) referred to the University Hospital of Liége, from across Europe. The researchers then compared their results with the well-established standardized Coma Recovery Scale-Revised (CSR-R) behavioral test, considered the most confirmed and sensitive technique for discriminating very low awareness.
FDG-PET was better overall than fMRI in differentiating conscious from unconscious patients. Mental imagery fMRI was less sensitive at diagnosis of a MCS than FDG-PET (45% vs. 93%), and had less agreement with behavioral CRS-R scores than FDG-PET (63% vs. 85%). FDG-PET was about 74% accurate in predicting the extent of recovery within the next year, compared with 56% for fMRI.
Significantly, one-third of the 36 patients diagnosed as behaviorally unresponsive on the CSR-R test who were scanned with FDG-PET showed brain activity consistent with the presence of some consciousness. Nine patients in this group consequently recovered a reasonable level of consciousness.
According to Prof. Laureys, “We confirm that a small but substantial proportion of behaviorally unresponsive patients retain brain activity compatible with awareness. Repeated testing with the CRS-R complemented with a cerebral FDG-PET examination provides a simple and reliable diagnostic tool with high sensitivity towards unresponsive but aware patients. fMRI during mental tasks might complement the assessment with information about preserved cognitive capability, but should not be the main or sole diagnostic imaging method.”
The authors noted that the study was conducted in a specialist unit focusing on the diagnostic neuroimaging of disorders of consciousness and therefore deployment might be more challenging in less specialist units.
Commenting on the study Drs. Sleigh and Warnaby added, “From these data, it would be hard to sustain a confident diagnosis of unresponsive wakefulness syndrome solely on behavioral grounds, without PET imaging for confirmation ... [This] work serves as a signpost for future studies. Functional brain imaging is expensive and technically challenging, but it will almost certainly become cheaper and easier. In the future, we will probably look back in amazement at how we were ever able to practice without it.”
Related Links:
University of Liége
Latest Nuclear Medicine News
- New Imaging Tool Sheds Light on Tumor Fat Metabolism
- PET Tracer Enables Noninvasive Measurement of Beta Cell Mass
- Radiopharmaceutical Molecule Marker to Improve Choice of Bladder Cancer Therapies
- Cancer “Flashlight” Shows Who Can Benefit from Targeted Treatments
- PET Imaging of Inflammation Predicts Recovery and Guides Therapy After Heart Attack
- Radiotheranostic Approach Detects, Kills and Reprograms Aggressive Cancers
- New Imaging Solution Improves Survival for Patients with Recurring Prostate Cancer
- PET Tracer Enables Same-Day Imaging of Triple-Negative Breast and Urothelial Cancers
- New Camera Sees Inside Human Body for Enhanced Scanning and Diagnosis
- Novel Bacteria-Specific PET Imaging Approach Detects Hard-To-Diagnose Lung Infections
- New Imaging Approach Could Reduce Need for Biopsies to Monitor Prostate Cancer
- Novel Radiolabeled Antibody Improves Diagnosis and Treatment of Solid Tumors
- Novel PET Imaging Approach Offers Never-Before-Seen View of Neuroinflammation
- Novel Radiotracer Identifies Biomarker for Triple-Negative Breast Cancer
- Innovative PET Imaging Technique to Help Diagnose Neurodegeneration
- New Molecular Imaging Test to Improve Lung Cancer Diagnosis
Channels
Radiography
view channel
AI Tool Predicts Breast Cancer Risk Years Ahead Using Routine Mammograms
Breast cancer screening saves lives but still relies largely on uniform schedules despite wide differences in individual risk. This one-size-fits-all approach can miss cancers in higher-risk women while... Read more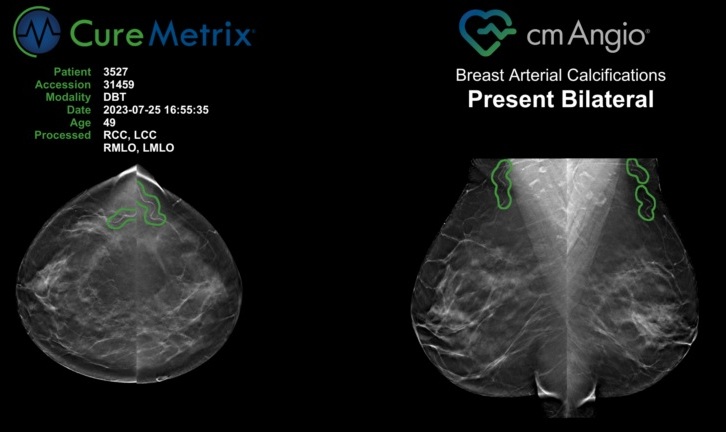
Routine Mammograms Could Predict Future Cardiovascular Disease in Women
Mammograms are widely used to screen for breast cancer, but they may also contain overlooked clues about cardiovascular health. Calcium deposits in the arteries of the breast signal stiffening blood vessels,... Read moreMRI
view channel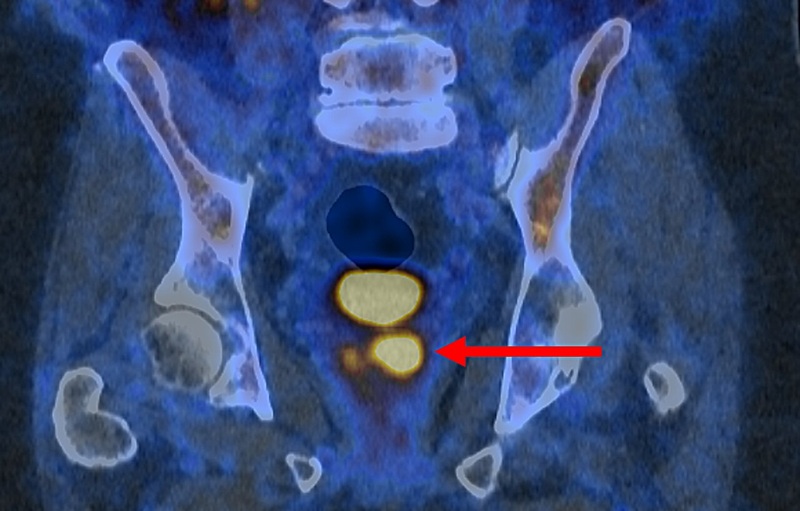
Study Finds Advanced Imaging Significantly Reduces Unnecessary Prostate Biopsies
Many men with suspected prostate cancer face an invasive biopsy when magnetic resonance imaging (MRI) is inconclusive. Biopsies can be uncomfortable, carry risks, and may contribute to overdiagnosis and... Read more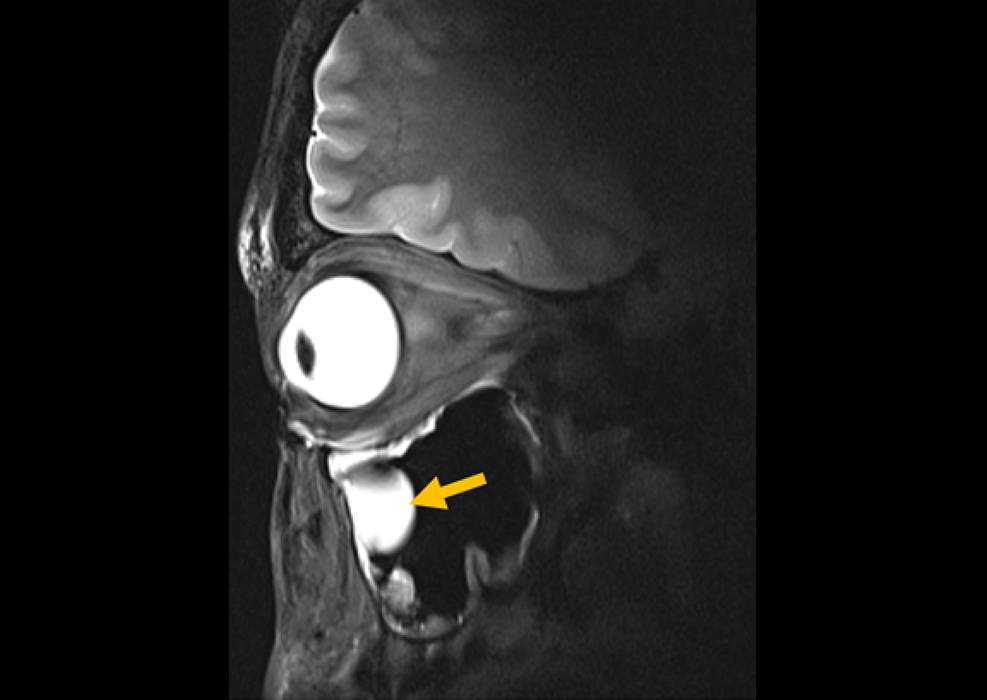
New Material Boosts MRI Image Quality
Magnetic resonance imaging (MRI) is a cornerstone of modern diagnostics, yet certain deep or anatomically complex tissues, including delicate structures of the eye and orbit, remain difficult to visualize clearly.... Read moreUltrasound
view channel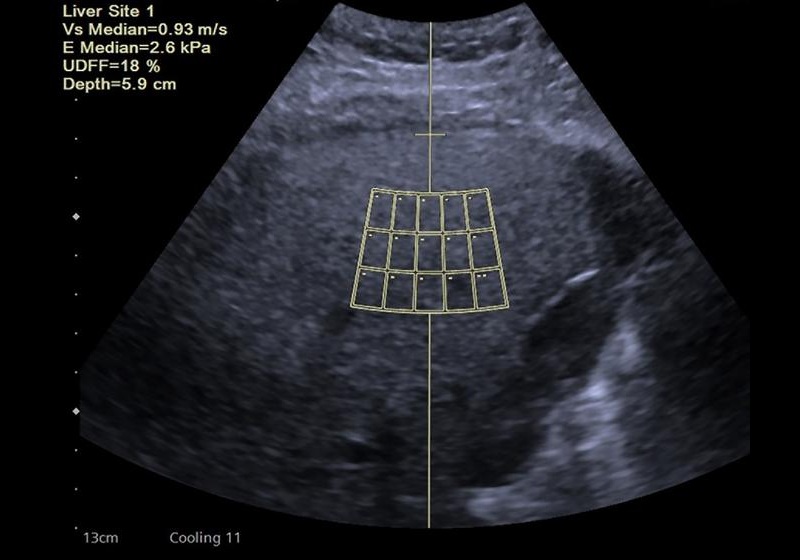
New Consensus Standardizes Ultrasound-Based Fatty Liver Assessment
Metabolic dysfunction-associated steatotic liver disease (MASLD) is rising along with obesity and diabetes, making accurate, scalable measurement of hepatic fat a clinical priority. Biopsy is invasive... Read more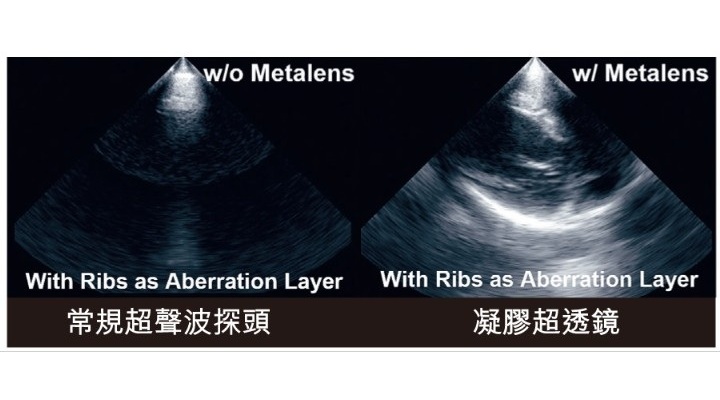
Groundbreaking Technology to Enhance Precision in Emergency and Critical Care
Rapid and accurate imaging is essential for diagnosing life-threatening conditions such as myocardial infarction, heart failure, and pulmonary embolism. However, conventional ultrasound imaging of the... Read moreGeneral/Advanced Imaging
view channel
AI Tool Predicts Side Effects from Lung Cancer Treatment
Radiation therapy is a central treatment for lung cancer, but even carefully targeted radiation can affect surrounding healthy tissue. Patients may develop side effects such as lung inflammation, coughing,... Read more
AI Tool Offers Prognosis for Patients with Head and Neck Cancer
Oropharyngeal cancer is a form of head and neck cancer that can spread through lymph nodes, significantly affecting survival and treatment decisions. Current therapies often involve combinations of surgery,... Read moreImaging IT
view channel
New Google Cloud Medical Imaging Suite Makes Imaging Healthcare Data More Accessible
Medical imaging is a critical tool used to diagnose patients, and there are billions of medical images scanned globally each year. Imaging data accounts for about 90% of all healthcare data1 and, until... Read more
Global AI in Medical Diagnostics Market to Be Driven by Demand for Image Recognition in Radiology
The global artificial intelligence (AI) in medical diagnostics market is expanding with early disease detection being one of its key applications and image recognition becoming a compelling consumer proposition... Read moreIndustry News
view channel
Nuclear Medicine Set for Continued Growth Driven by Demand for Precision Diagnostics
Clinical imaging services face rising demand for precise molecular diagnostics and targeted radiopharmaceutical therapy as cancer and chronic disease rates climb. A new market analysis projects rapid expansion... Read more