Axillary Radiotherapy and SNL Surgery Show Comparable Outcomes
|
By MedImaging International staff writers Posted on 31 Dec 2018 |
Patients with early-stage breast cancer had similar recurrence and survival rates for both axillary lymph node radiotherapy (RT) and dissection, according to a new study.
Researchers at the Netherlands Cancer Institute (NKI; Amsterdam), the European Organisation for Research and Treatment of Cancer (EORTC; Brussels, Belgium), and other institutions conducted a study in 4,806 patients with early-stage, clinically node-negative breast cancer, of whom 1,425 went on to have a positive sentinel lymph node (SLN) biopsy. Of these, 744 were randomly assigned to the axillary lymph node dissection group, and 681 to the axillary RT group. After 10 years, 1.82% of those assigned to axillary RT had axillary recurrence, compared with 0.93% of those assigned to dissection.
In addition, distant metastasis-free survival was 78.2% among those assigned to axillary RT and 81.7% among those assigned to axillary lymph node dissection; overall survival in the two arms was 81.4% percent and 84.6%, respectively. A significantly greater proportion of patients assigned to axillary RT went on to develop a second primary cancer (11%) than did patients assigned to axillary lymph node dissection (7.7%). The difference was mainly due to a higher incidence of contralateral breast cancer in the patients treated with axillary RT. The study was presented at the annual San Antonio Breast Cancer Symposium, held during December 2018 in San Antonio (TX, USA).
“Our new 10-year data show that axillary radiotherapy and axillary lymph node dissection provide excellent and comparable overall survival, distant-metastasis-free survival, and locoregional control,” said lead author and study presenter radiation oncologist Mila Donker, MD, PhD, of NKI. “We believe that axillary radiotherapy should be considered a good option for patients who have a positive sentinel lymph node biopsy, instead of complete surgical clearance of the axillary lymph nodes.”
“Traditionally, those patients who had cancer detected in a SLN biopsy underwent axillary lymph node dissection, which is an effective but invasive surgical procedure that is associated with adverse side effects such as lymphedema and difficulties moving the arm,” said senior author surgical oncologist Emiel Rutgers, MD, PhD. “There may be some patients who do not need axillary treatment, even if they have a positive SLN biopsy. Moving forward, we need to better tailor treatment for each individual patient. Some will still need axillary treatment, and our data indicate that axillary radiotherapy is a good option here.”
Finding metastatic cancer cells during breast cancer surgery requires first identifying the position of the SNLs, which have a diameter of just a few millimeters, and then excising them for hisotpathology. If the cancer has not yet metastasized to an SLN, axillary lymph node excision can be omitted, thus preventing subsequent lymphedema and maintaining the patient's quality of life after surgery.
Related Links:
Netherlands Cancer Institute
European Organisation for Research and Treatment of Cancer
Researchers at the Netherlands Cancer Institute (NKI; Amsterdam), the European Organisation for Research and Treatment of Cancer (EORTC; Brussels, Belgium), and other institutions conducted a study in 4,806 patients with early-stage, clinically node-negative breast cancer, of whom 1,425 went on to have a positive sentinel lymph node (SLN) biopsy. Of these, 744 were randomly assigned to the axillary lymph node dissection group, and 681 to the axillary RT group. After 10 years, 1.82% of those assigned to axillary RT had axillary recurrence, compared with 0.93% of those assigned to dissection.
In addition, distant metastasis-free survival was 78.2% among those assigned to axillary RT and 81.7% among those assigned to axillary lymph node dissection; overall survival in the two arms was 81.4% percent and 84.6%, respectively. A significantly greater proportion of patients assigned to axillary RT went on to develop a second primary cancer (11%) than did patients assigned to axillary lymph node dissection (7.7%). The difference was mainly due to a higher incidence of contralateral breast cancer in the patients treated with axillary RT. The study was presented at the annual San Antonio Breast Cancer Symposium, held during December 2018 in San Antonio (TX, USA).
“Our new 10-year data show that axillary radiotherapy and axillary lymph node dissection provide excellent and comparable overall survival, distant-metastasis-free survival, and locoregional control,” said lead author and study presenter radiation oncologist Mila Donker, MD, PhD, of NKI. “We believe that axillary radiotherapy should be considered a good option for patients who have a positive sentinel lymph node biopsy, instead of complete surgical clearance of the axillary lymph nodes.”
“Traditionally, those patients who had cancer detected in a SLN biopsy underwent axillary lymph node dissection, which is an effective but invasive surgical procedure that is associated with adverse side effects such as lymphedema and difficulties moving the arm,” said senior author surgical oncologist Emiel Rutgers, MD, PhD. “There may be some patients who do not need axillary treatment, even if they have a positive SLN biopsy. Moving forward, we need to better tailor treatment for each individual patient. Some will still need axillary treatment, and our data indicate that axillary radiotherapy is a good option here.”
Finding metastatic cancer cells during breast cancer surgery requires first identifying the position of the SNLs, which have a diameter of just a few millimeters, and then excising them for hisotpathology. If the cancer has not yet metastasized to an SLN, axillary lymph node excision can be omitted, thus preventing subsequent lymphedema and maintaining the patient's quality of life after surgery.
Related Links:
Netherlands Cancer Institute
European Organisation for Research and Treatment of Cancer
Latest Nuclear Medicine News
- New PET Agent Rapidly and Accurately Visualizes Lesions in Clear Cell Renal Cell Carcinoma Patients
- New Imaging Technique Monitors Inflammation Disorders without Radiation Exposure
- New SPECT/CT Technique Could Change Imaging Practices and Increase Patient Access
- New Radiotheranostic System Detects and Treats Ovarian Cancer Noninvasively
- AI System Automatically and Reliably Detects Cardiac Amyloidosis Using Scintigraphy Imaging
- Early 30-Minute Dynamic FDG-PET Acquisition Could Halve Lung Scan Times
- New Method for Triggering and Imaging Seizures to Help Guide Epilepsy Surgery
- Radioguided Surgery Accurately Detects and Removes Metastatic Lymph Nodes in Prostate Cancer Patients
- New PET Tracer Detects Inflammatory Arthritis Before Symptoms Appear
- Novel PET Tracer Enhances Lesion Detection in Medullary Thyroid Cancer
- Targeted Therapy Delivers Radiation Directly To Cells in Hard-To-Treat Cancers
- New PET Tracer Noninvasively Identifies Cancer Gene Mutation for More Precise Diagnosis
- Algorithm Predicts Prostate Cancer Recurrence in Patients Treated by Radiation Therapy
- Novel PET Imaging Tracer Noninvasively Identifies Cancer Gene Mutation for More Precise Diagnosis
- Ultrafast Laser Technology to Improve Cancer Treatment
- Low-Dose Radiation Therapy Demonstrates Potential for Treatment of Heart Failure
Channels
Radiography
view channel
Novel Breast Imaging System Proves As Effective As Mammography
Breast cancer remains the most frequently diagnosed cancer among women. It is projected that one in eight women will be diagnosed with breast cancer during her lifetime, and one in 42 women who turn 50... Read more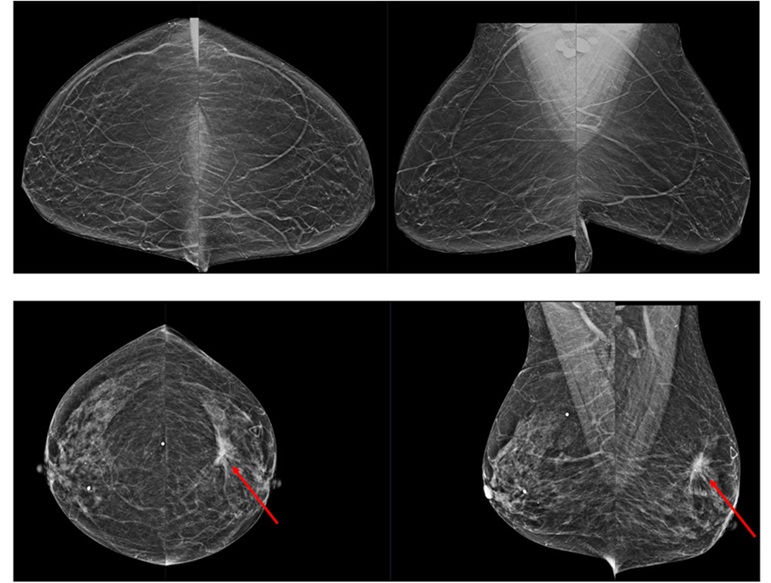
AI Assistance Improves Breast-Cancer Screening by Reducing False Positives
Radiologists typically detect one case of cancer for every 200 mammograms reviewed. However, these evaluations often result in false positives, leading to unnecessary patient recalls for additional testing,... Read moreMRI
view channel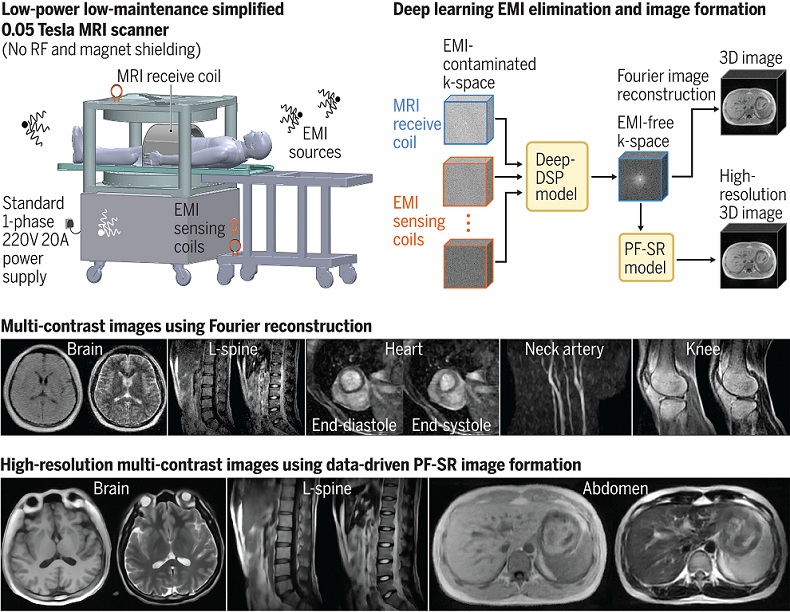
Low-Cost Whole-Body MRI Device Combined with AI Generates High-Quality Results
Magnetic Resonance Imaging (MRI) has significantly transformed healthcare, providing a noninvasive, radiation-free method for detailed imaging. It is especially promising for the future of medical diagnosis... Read more
World's First Whole-Body Ultra-High Field MRI Officially Comes To Market
The world's first whole-body ultra-high field (UHF) MRI has officially come to market, marking a remarkable advancement in diagnostic radiology. United Imaging (Shanghai, China) has secured clearance from the U.... Read moreUltrasound
view channel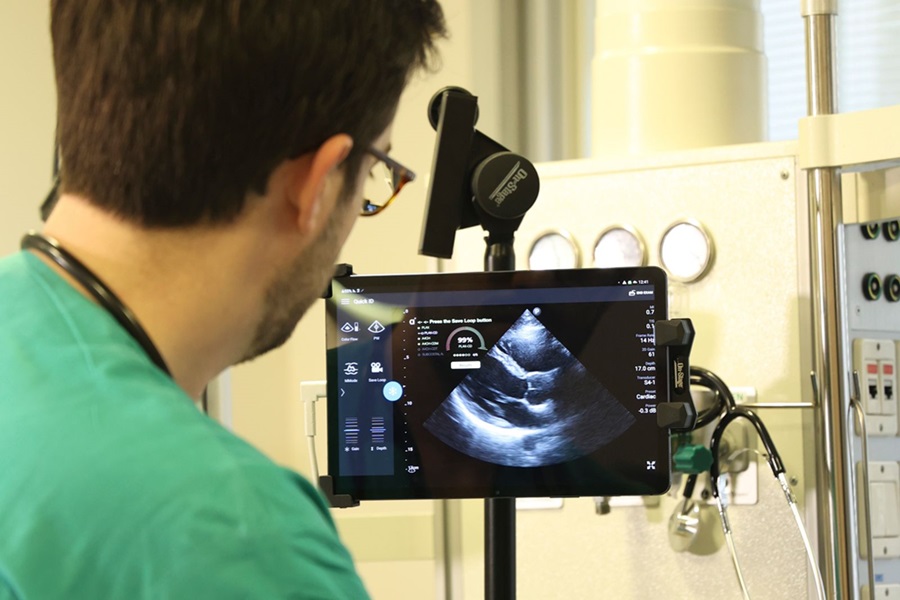
First AI-Powered POC Ultrasound Diagnostic Solution Helps Prioritize Cases Based On Severity
Ultrasound scans are essential for identifying and diagnosing various medical conditions, but often, patients must wait weeks or months for results due to a shortage of qualified medical professionals... Read more
Largest Model Trained On Echocardiography Images Assesses Heart Structure and Function
Foundation models represent an exciting frontier in generative artificial intelligence (AI), yet many lack the specialized medical data needed to make them applicable in healthcare settings.... Read more.jpg)
Groundbreaking Technology Enables Precise, Automatic Measurement of Peripheral Blood Vessels
The current standard of care of using angiographic information is often inadequate for accurately assessing vessel size in the estimated 20 million people in the U.S. who suffer from peripheral vascular disease.... Read moreGeneral/Advanced Imaging
view channel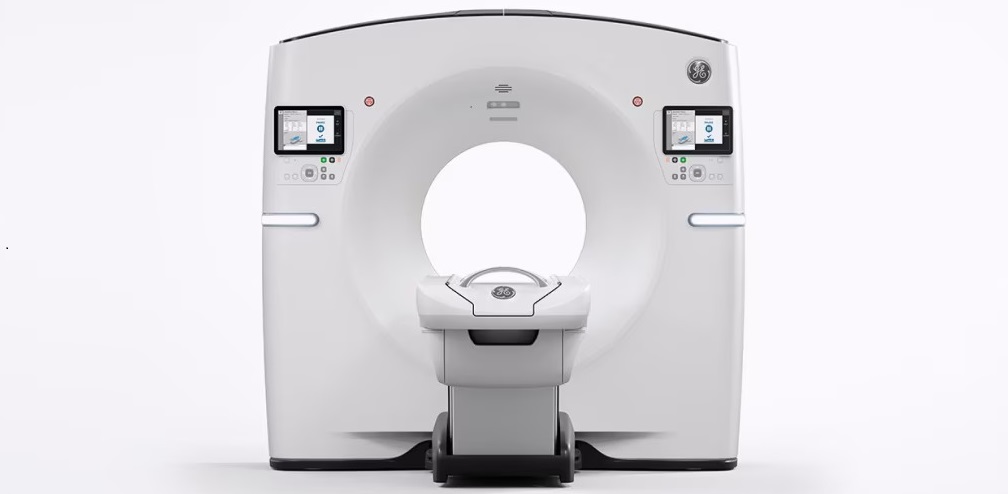
Radiation Therapy Computed Tomography Solution Boosts Imaging Accuracy
One of the most significant challenges in oncology care is disease complexity in terms of the variety of cancer types and the individualized presentation of each patient. This complexity necessitates a... Read more
PET Scans Reveal Hidden Inflammation in Multiple Sclerosis Patients
A key challenge for clinicians treating patients with multiple sclerosis (MS) is that after a certain amount of time, they continue to worsen even though their MRIs show no change. A new study has now... Read moreImaging IT
view channel
New Google Cloud Medical Imaging Suite Makes Imaging Healthcare Data More Accessible
Medical imaging is a critical tool used to diagnose patients, and there are billions of medical images scanned globally each year. Imaging data accounts for about 90% of all healthcare data1 and, until... Read more
Global AI in Medical Diagnostics Market to Be Driven by Demand for Image Recognition in Radiology
The global artificial intelligence (AI) in medical diagnostics market is expanding with early disease detection being one of its key applications and image recognition becoming a compelling consumer proposition... Read moreIndustry News
view channel
Hologic Acquires UK-Based Breast Surgical Guidance Company Endomagnetics Ltd.
Hologic, Inc. (Marlborough, MA, USA) has entered into a definitive agreement to acquire Endomagnetics Ltd. (Cambridge, UK), a privately held developer of breast cancer surgery technologies, for approximately... Read more
Bayer and Google Partner on New AI Product for Radiologists
Medical imaging data comprises around 90% of all healthcare data, and it is a highly complex and rich clinical data modality and serves as a vital tool for diagnosing patients. Each year, billions of medical... Read more