Hypofractionated Radiation Acceptable for Localized Prostate Cancer
|
By MedImaging International staff writers Posted on 05 Nov 2018 |
A new study supports the use of shortened courses of radiation therapy (RT) for early-stage prostate cancer (PC).
Researchers at the University of Ottawa (Canada), Cedars-Sinai Medical Center (Los Angeles, CA, USA), Vanderbilt University Medical Center (VUMC; Nashville, TN, USA), and other institutions participating in a new task force convened by the American Society for Radiation Oncology (ASTRO) conducted a systematic literature review to address key questions and develop an evidence-based guideline for dose-fractionation RT for early-stage PC.
Among the issues discussed were technical aspects, including normal tissue dose constraints, treatment volumes, and use of image guided RT (IMRT) and intensity modulated RT (IMRT). Based on high-quality evidence, a strong consensus was reached to offer moderate hypofractionation across risk groups to patients choosing external beam RT (EBRT), and recommended ultrahypofractionated RT for low- and intermediate-risk PC. For high-risk patients, the routine use of ultrahypofractionated EBRT was not recommended. The study was published on October 11, 2018, in Practical Radiation Oncology.
“These recommendations are intended to provide guidance on moderate hypofractionation and ultrahypofractionation for localized prostate cancer. Men who opt to receive hypofractionated radiation therapy will be able to receive a shorter course of treatment,” concluded lead author Scott Morgan, MD, of the University of Ottawa, and colleagues. “The limits in the current evidentiary base, especially for ultrahypofractionation, highlight the imperative to support large-scale randomized clinical trials and underscore the importance of shared decision making between clinicians and patients.”
RT fractionation is defined as a fraction size of 180 to 200 cGy. Hypofractionation is subdivided into moderate hypofractionation (240-340 cGy) and ultrahypofractionation (a fraction size higher 500 cGy). These pragmatic definitions reflect two distinct approaches to hypofractionation that have emerged in clinical practice. The fraction size gap created (i.e., the gap from 340 cGy and 500 cGy) represents a little-studied range.
Related Links:
University of Ottawa
Cedars-Sinai Medical Center
Vanderbilt University Medical Center
Researchers at the University of Ottawa (Canada), Cedars-Sinai Medical Center (Los Angeles, CA, USA), Vanderbilt University Medical Center (VUMC; Nashville, TN, USA), and other institutions participating in a new task force convened by the American Society for Radiation Oncology (ASTRO) conducted a systematic literature review to address key questions and develop an evidence-based guideline for dose-fractionation RT for early-stage PC.
Among the issues discussed were technical aspects, including normal tissue dose constraints, treatment volumes, and use of image guided RT (IMRT) and intensity modulated RT (IMRT). Based on high-quality evidence, a strong consensus was reached to offer moderate hypofractionation across risk groups to patients choosing external beam RT (EBRT), and recommended ultrahypofractionated RT for low- and intermediate-risk PC. For high-risk patients, the routine use of ultrahypofractionated EBRT was not recommended. The study was published on October 11, 2018, in Practical Radiation Oncology.
“These recommendations are intended to provide guidance on moderate hypofractionation and ultrahypofractionation for localized prostate cancer. Men who opt to receive hypofractionated radiation therapy will be able to receive a shorter course of treatment,” concluded lead author Scott Morgan, MD, of the University of Ottawa, and colleagues. “The limits in the current evidentiary base, especially for ultrahypofractionation, highlight the imperative to support large-scale randomized clinical trials and underscore the importance of shared decision making between clinicians and patients.”
RT fractionation is defined as a fraction size of 180 to 200 cGy. Hypofractionation is subdivided into moderate hypofractionation (240-340 cGy) and ultrahypofractionation (a fraction size higher 500 cGy). These pragmatic definitions reflect two distinct approaches to hypofractionation that have emerged in clinical practice. The fraction size gap created (i.e., the gap from 340 cGy and 500 cGy) represents a little-studied range.
Related Links:
University of Ottawa
Cedars-Sinai Medical Center
Vanderbilt University Medical Center
Latest Nuclear Medicine News
- New SPECT/CT Technique Could Change Imaging Practices and Increase Patient Access
- New Radiotheranostic System Detects and Treats Ovarian Cancer Noninvasively
- AI System Automatically and Reliably Detects Cardiac Amyloidosis Using Scintigraphy Imaging
- Early 30-Minute Dynamic FDG-PET Acquisition Could Halve Lung Scan Times
- New Method for Triggering and Imaging Seizures to Help Guide Epilepsy Surgery
- Radioguided Surgery Accurately Detects and Removes Metastatic Lymph Nodes in Prostate Cancer Patients
- New PET Tracer Detects Inflammatory Arthritis Before Symptoms Appear
- Novel PET Tracer Enhances Lesion Detection in Medullary Thyroid Cancer
- Targeted Therapy Delivers Radiation Directly To Cells in Hard-To-Treat Cancers
- New PET Tracer Noninvasively Identifies Cancer Gene Mutation for More Precise Diagnosis
- Algorithm Predicts Prostate Cancer Recurrence in Patients Treated by Radiation Therapy
- Novel PET Imaging Tracer Noninvasively Identifies Cancer Gene Mutation for More Precise Diagnosis
- Ultrafast Laser Technology to Improve Cancer Treatment
- Low-Dose Radiation Therapy Demonstrates Potential for Treatment of Heart Failure
- New PET Radiotracer Aids Early, Noninvasive Detection of Inflammatory Bowel Disease
- Combining Amino Acid PET and MRI Imaging to Help Treat Aggressive Brain Tumors
Channels
Radiography
view channel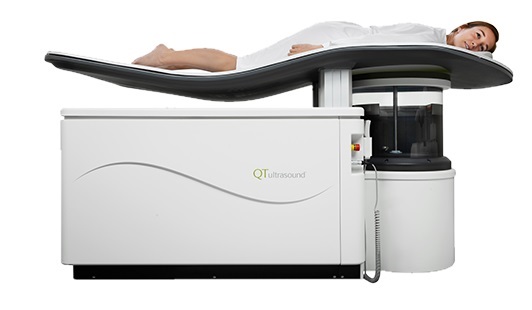
Novel Breast Imaging System Proves As Effective As Mammography
Breast cancer remains the most frequently diagnosed cancer among women. It is projected that one in eight women will be diagnosed with breast cancer during her lifetime, and one in 42 women who turn 50... Read more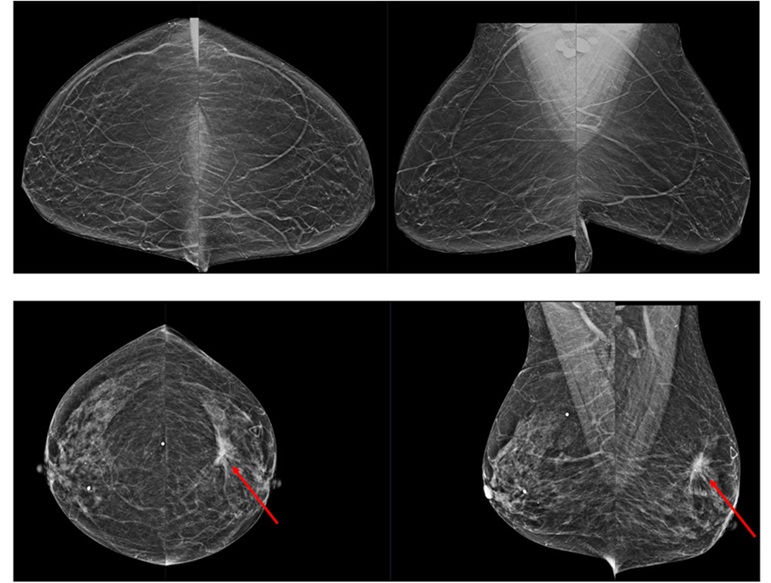
AI Assistance Improves Breast-Cancer Screening by Reducing False Positives
Radiologists typically detect one case of cancer for every 200 mammograms reviewed. However, these evaluations often result in false positives, leading to unnecessary patient recalls for additional testing,... Read moreMRI
view channel.jpg)
Combining MRI with PSA Testing Improves Clinical Outcomes for Prostate Cancer Patients
Prostate cancer is a leading health concern globally, consistently being one of the most common types of cancer among men and a major cause of cancer-related deaths. In the United States, it is the most... Read more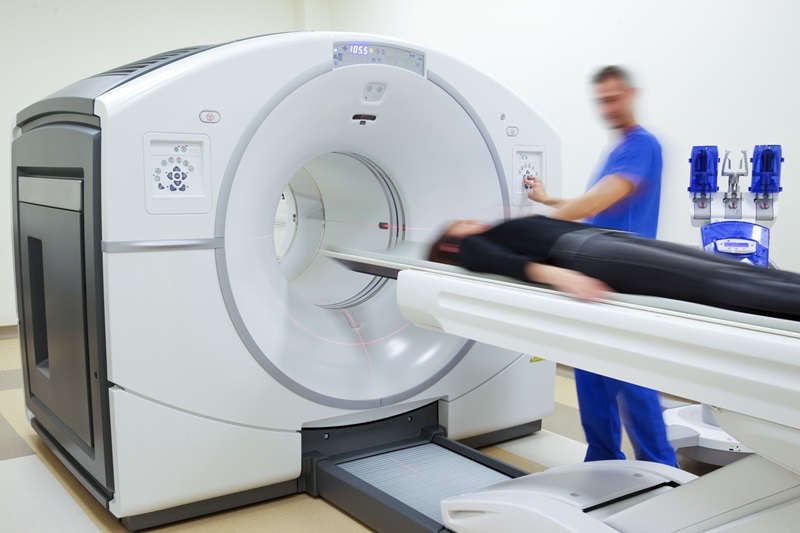
PET/MRI Improves Diagnostic Accuracy for Prostate Cancer Patients
The Prostate Imaging Reporting and Data System (PI-RADS) is a five-point scale to assess potential prostate cancer in MR images. PI-RADS category 3 which offers an unclear suggestion of clinically significant... Read more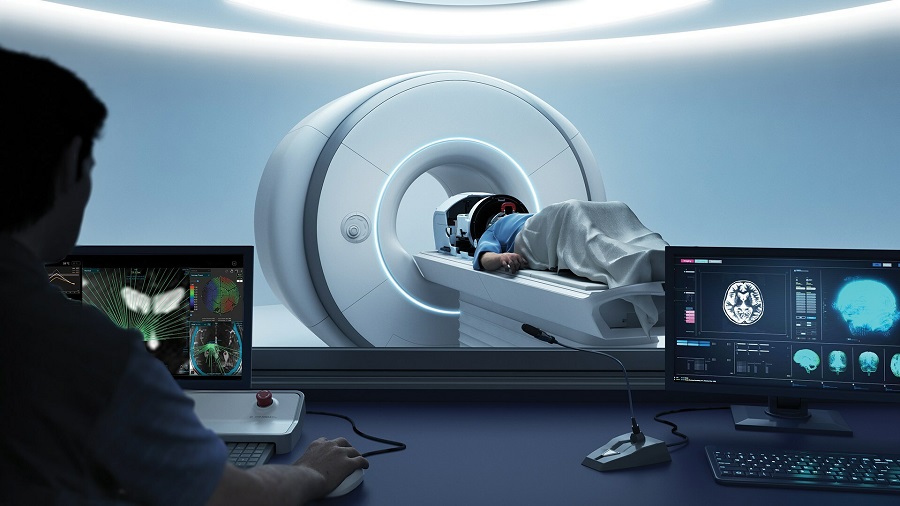
Next Generation MR-Guided Focused Ultrasound Ushers In Future of Incisionless Neurosurgery
Essential tremor, often called familial, idiopathic, or benign tremor, leads to uncontrollable shaking that significantly affects a person’s life. When traditional medications do not alleviate symptoms,... Read more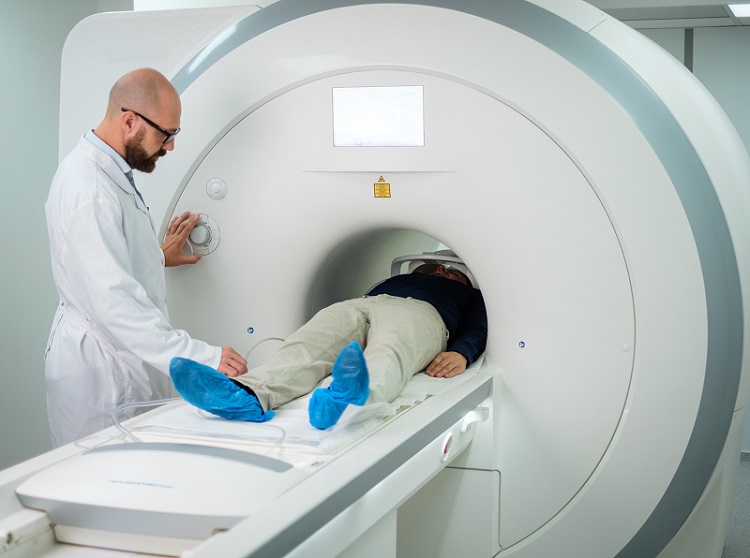
Two-Part MRI Scan Detects Prostate Cancer More Quickly without Compromising Diagnostic Quality
Prostate cancer ranks as the most prevalent cancer among men. Over the last decade, the introduction of MRI scans has significantly transformed the diagnosis process, marking the most substantial advancement... Read moreUltrasound
view channel.jpg)
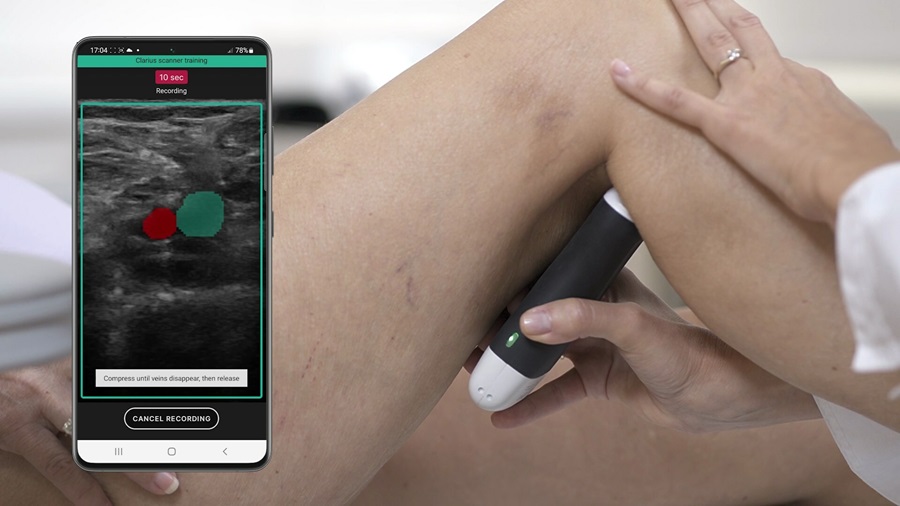
Groundbreaking Technology Enables Precise, Automatic Measurement of Peripheral Blood Vessels
The current standard of care of using angiographic information is often inadequate for accurately assessing vessel size in the estimated 20 million people in the U.S. who suffer from peripheral vascular disease.... Read more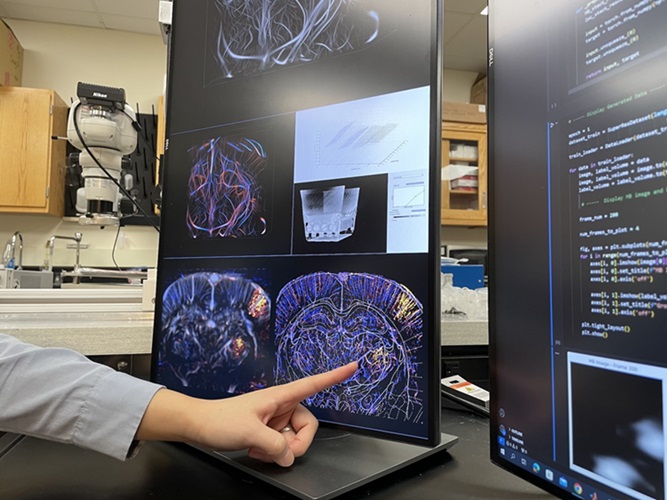
Deep Learning Advances Super-Resolution Ultrasound Imaging
Ultrasound localization microscopy (ULM) is an advanced imaging technique that offers high-resolution visualization of microvascular structures. It employs microbubbles, FDA-approved contrast agents, injected... Read more
Novel Ultrasound-Launched Targeted Nanoparticle Eliminates Biofilm and Bacterial Infection
Biofilms, formed by bacteria aggregating into dense communities for protection against harsh environmental conditions, are a significant contributor to various infectious diseases. Biofilms frequently... Read moreGeneral/Advanced Imaging
view channel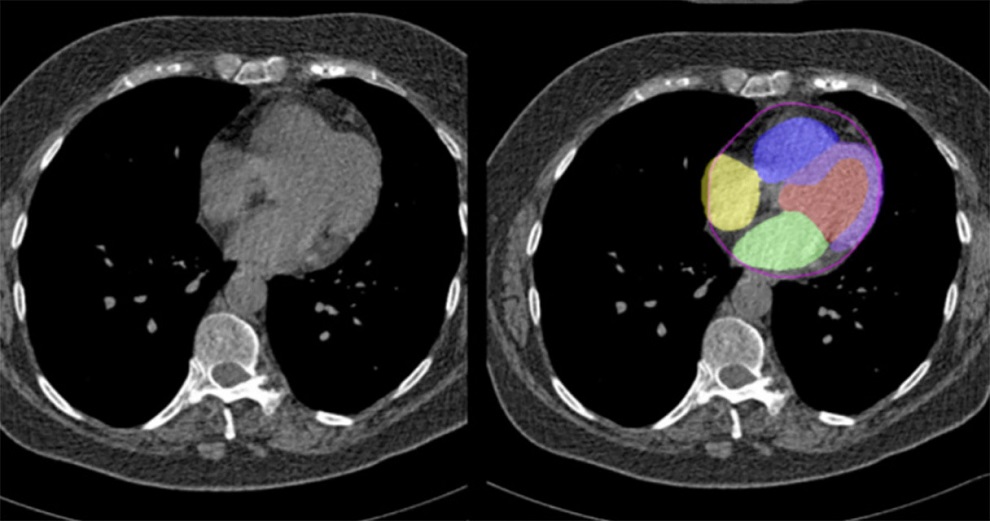
Artificial Intelligence Evaluates Cardiovascular Risk from CT Scans
Chest computed tomography (CT) is a common diagnostic tool, with approximately 15 million scans conducted each year in the United States, though many are underutilized or not fully explored.... Read more
New AI Method Captures Uncertainty in Medical Images
In the field of biomedicine, segmentation is the process of annotating pixels from an important structure in medical images, such as organs or cells. Artificial Intelligence (AI) models are utilized to... Read more.jpg)
CT Coronary Angiography Reduces Need for Invasive Tests to Diagnose Coronary Artery Disease
Coronary artery disease (CAD), one of the leading causes of death worldwide, involves the narrowing of coronary arteries due to atherosclerosis, resulting in insufficient blood flow to the heart muscle.... Read more
Novel Blood Test Could Reduce Need for PET Imaging of Patients with Alzheimer’s
Alzheimer's disease (AD), a condition marked by cognitive decline and the presence of beta-amyloid (Aβ) plaques and neurofibrillary tangles in the brain, poses diagnostic challenges. Amyloid positron emission... Read moreImaging IT
view channel
New Google Cloud Medical Imaging Suite Makes Imaging Healthcare Data More Accessible
Medical imaging is a critical tool used to diagnose patients, and there are billions of medical images scanned globally each year. Imaging data accounts for about 90% of all healthcare data1 and, until... Read more
Global AI in Medical Diagnostics Market to Be Driven by Demand for Image Recognition in Radiology
The global artificial intelligence (AI) in medical diagnostics market is expanding with early disease detection being one of its key applications and image recognition becoming a compelling consumer proposition... Read moreIndustry News
view channel
Bayer and Google Partner on New AI Product for Radiologists
Medical imaging data comprises around 90% of all healthcare data, and it is a highly complex and rich clinical data modality and serves as a vital tool for diagnosing patients. Each year, billions of medical... Read more