AI-Based Risk Model Leverages Mammograms for Personalized Breast Cancer Screening
|
By MedImaging International staff writers Posted on 21 Jan 2022 |
A new technology for creating risk-based screening guidelines use machine learning to provide personalized breast cancer screening.
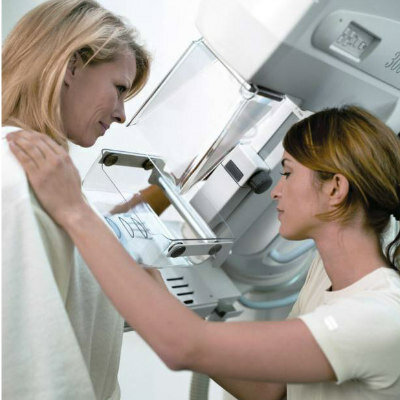
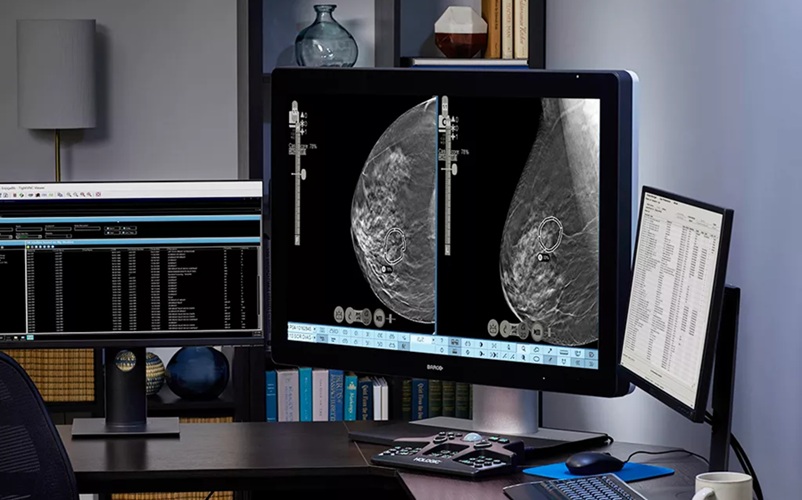
Tempo, developed by scientists from MIT’s Computer Science and Artificial Intelligence Laboratory (CSAIL) and Jameel Clinic for Machine Learning and Health (Cambridge MA, USA), uses an AI-based risk model that looks at who was screened and when they got diagnosed to recommend a patient return for a mammogram at a specific time point in the future, like six months or three years. The same Tempo policy can be easily adapted to a wide range of possible screening preferences, which would let clinicians pick their desired early detection to screening cost trade-off, without training new policies.
While mammograms are currently the gold standard in breast cancer screening, swirls of controversy exist: advocates argue for the ability to save lives, (women 60-69 had a 33% lower risk of dying compared to those who didn’t get mammograms), and another camp argues about costly and potentially traumatic false positives (a meta-analysis of three randomized trials found a 19% over-diagnosis rate from mammography). Even with some saved lives, and some overtreatment and overscreening, current guidelines are still a catch all: women aged 45 to 54 should get mammograms every year. While personalized screening has long been thought of as the answer, tools that can leverage the troves of data to do this lag behind.
Early uses of AI in medicine stem back to the 1960’s, where many refer to the Dendral experiments as kicking off the field. Researchers created a software system that was considered the first expert kind that automated the decision-making and problem-solving behavior of organic chemists. Sixty years later, deep medicine has greatly evolved drug diagnostics, predictive medicine, and patient care.
Tempo uses reinforcement learning, a machine learning method widely known for success in games like Chess and Go, to develop a “policy” that predicts a follow-up recommendation for each patient. The training data here only had information about a patient’s risk at the time points when their mammogram was taken (when they were 50, or 55, for example). The team needed the risk assessment at intermediate points, so they designed their algorithm to learn a patient’s risk at unobserved time points from their observed screenings, which evolved as new mammograms of the patient became available.
The team first trained a neural network to predict future risk assessments given previous ones. This model then estimates patient risk at unobserved time points, and it enables simulation of the risk-based screening policies. Next, they trained that policy, (also a neural network), to maximize the reward (for example, the combination of early detection and screening cost) to the retrospective training set. Eventually, you’d get a recommendation for when to return for the next screen, ranging from six months to three years in the future, in multiples of six months – the standard is only one or two years.
Let’s say patient A comes in for their first mammogram, and eventually gets diagnosed at year four. In year two, there’s nothing, so they don’t come back for another two years, but then at year four they get a diagnosis. Now there's been two years of gap between the last screen, where a tumor could have grown. Using Tempo, at that first mammogram, year zero, the recommendation might have been to come back in two years. And then at year two, it might have seen that risk is high, and recommended that the patient come back in six months, and in the best case, it would be detectable. The model is dynamically changing the patient’s screening frequency, based on how the risk profile is changing.
Tempo uses a simple metric for early detection, which assumes that cancer can be caught up to 18 months in advance. While Tempo outperformed current guidelines across different settings of this assumption (six months, twelve months), none of these assumptions are perfect as the early detection potential of a tumor depends on that tumor's characteristics. The team suggested that follow up work using tumor growth models could address this issue. Also, the screening cost metric, which counts the total screening volume recommended by Tempo, doesn't provide a full analysis of the entire future cost because it does not explicitly quantify false positive risks or additional screening harms.
There are many future directions that can further improve personalized screening algorithms. The team says one avenue would be to build on the metrics used to estimate early detection and screening costs from retrospective data, which would result in more refined guidelines. Tempo could also be adapted to include different types of screening recommendations, such as leveraging MRI or mammograms, and future work could separately model the costs and benefits of each. With better screening policies, recalculating the earliest and latest age that screening is still cost-effective for a patient might be feasible.
“By tailoring the screening to the patient's individual risk, we can improve patient outcomes, reduce over treatment and eliminate health disparities,” said Adam Yala, MIT CSAIL PhD student and lead researcher. Given the massive scale of breast cancer screening, with tens of millions of women getting mammograms every year, improvements to our guidelines are immensely important.”
“Current guidelines divide the population into a few large groups, like younger or older than 55, and recommend the same screening frequency to all the members of a cohort. The development of AI based risk models that operate over raw patient data give us an opportunity to transform screening, giving more frequent screens to those who need it and sparing the rest,” added Yala. “A key aspect of these models is that their predictions can evolve over time as a patient’s raw data changes, suggesting that screening policies need to be attuned to changes in risk and be optimized over long periods of patient data.”
Related Links:
CSAIL
Latest General/Advanced Imaging News
- New SPECT/CT Method Differentiates Inflammation from Fibrosis in Interstitial Lung Disease
- Whole-Body PET/CT Tracks Metabolic Changes After Bariatric Surgery
- PET Tracer Localizes Overactive Adrenal Glands in Primary Aldosteronism
- Multimodal AI Tool Combines CT and Health Records to Predict Heart Risk
- AI Tool Automates Radiotherapy Planning for Cervical and Prostate Cancer
- New Proton Therapy Platform Integrates into Existing Radiotherapy Departments
- 3D-Printed Intraoral Device Enhances Head and Neck Radiotherapy Accuracy
- Molecular Imaging Agent Shows Promise for Endometriosis Detection and Monitoring
- Automated AI Tool Detects Early Pancreatic Cancer on Routine CT
- Routine Cardiac CT Enhanced to Predict Heart Failure Risk
- New Breast Imaging Viewer Unifies Modalities and Enhances Clinical Workflow
- Radiomics Analysis of CT Scans Enhances Evaluation of Sarcoidosis
- Hybrid AI System Improves Early Lung Cancer Detection on CT
- AI Tool Predicts Side Effects from Lung Cancer Treatment
- AI Tool Offers Prognosis for Patients with Head and Neck Cancer
- New 3D Imaging System Addresses MRI, CT and Ultrasound Limitations
Channels
Radiography
view channel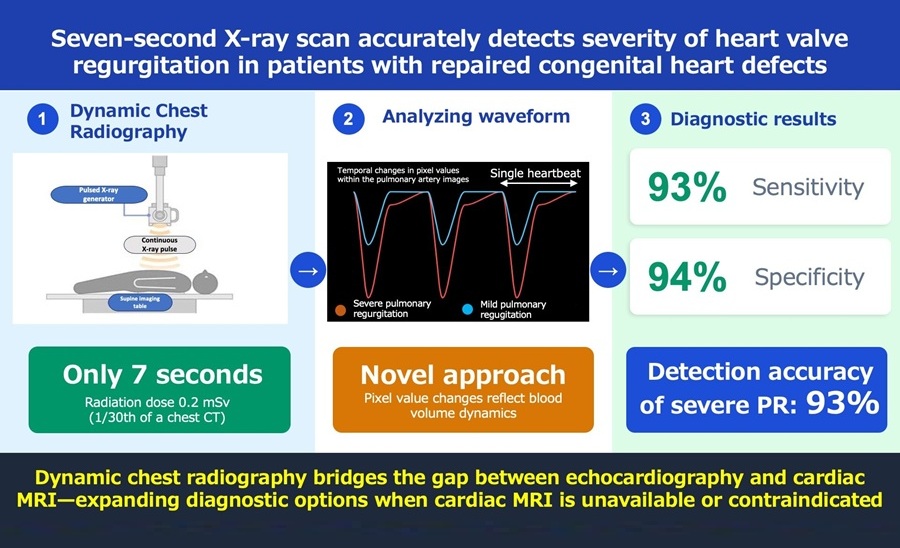
Rapid X-Ray Test Quantifies Pulmonary Regurgitation After Tetralogy of Fallot Repair
Tetralogy of Fallot is the most common cyanotic congenital heart defect and can leave patients with pulmonary valve regurgitation, a backward flow of blood into the right ventricle after repair.... Read more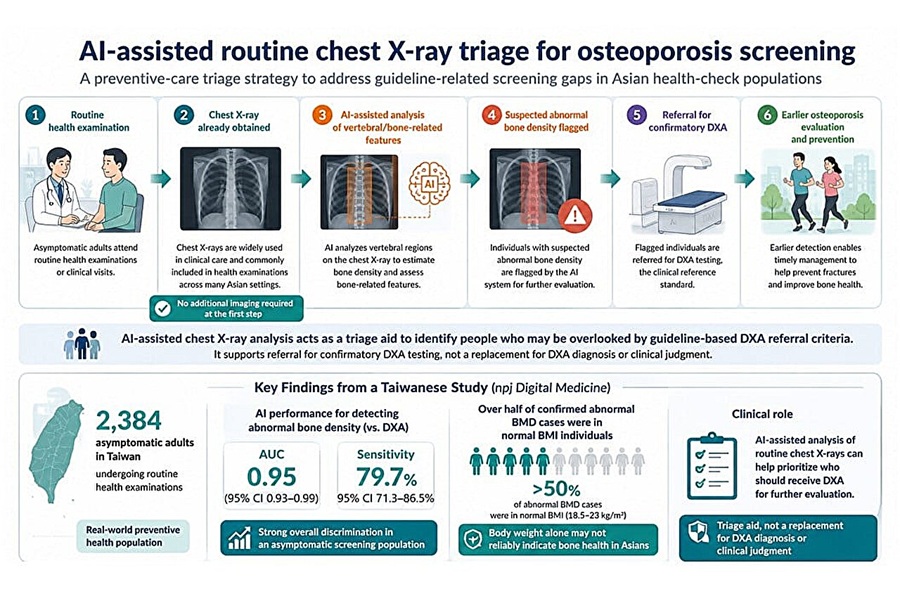
AI Tool Flags Osteoporosis Risk from Routine Chest X-Rays
Osteoporosis is a progressive loss of bone density that is often silent until a fracture occurs. Current screening frameworks concentrate on older women and select high-risk groups. Many men, younger adults,... Read moreMRI
view channel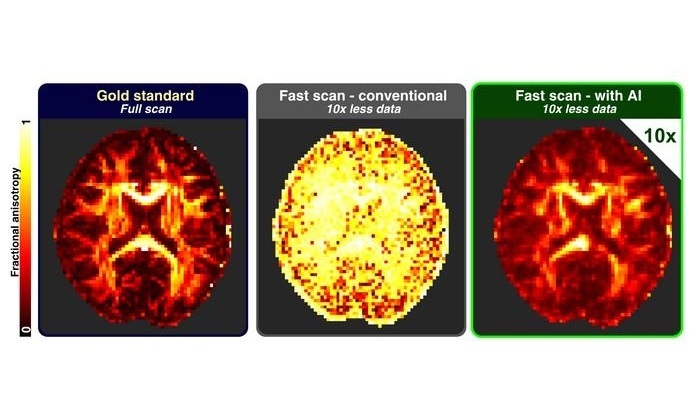
AI Approach Could Shorten Advanced Brain MRI Scans by Up to 90%
Long acquisition times for advanced brain magnetic resonance imaging (MRI) can limit access, extend waiting lists, and disrupt clinical workflows. Reducing data requirements without sacrificing image fidelity... Read more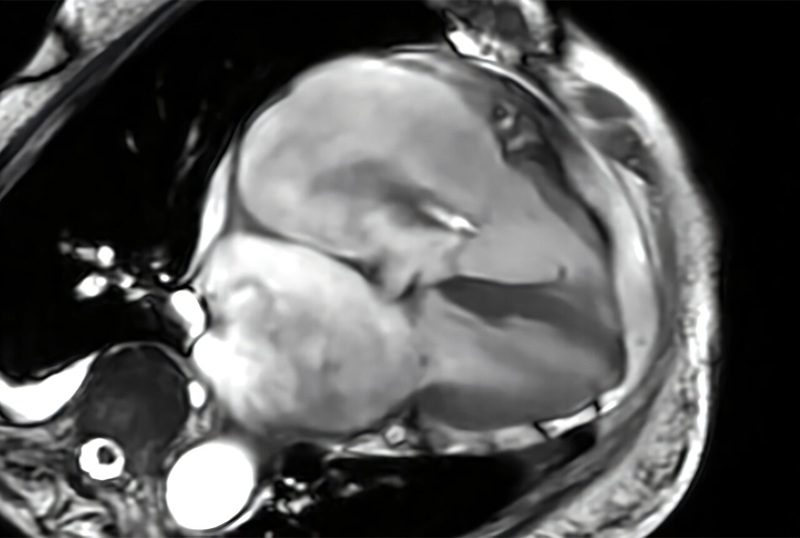
Cardiac MRI Measure Improves Risk Prediction in Tricuspid Regurgitation
Tricuspid regurgitation, in which blood flows back from the right ventricle into the right atrium, can lead to progressive right-sided heart failure. Clinicians need reliable ways to gauge severity and... Read moreUltrasound
view channelAI Robotic Ultrasound System Automates Echocardiography and Improves Consistency
Echocardiography, an ultrasound examination of the heart, is central to diagnosing and managing cardiovascular disease. Many services struggle with limited availability of skilled sonographers, variable... Read more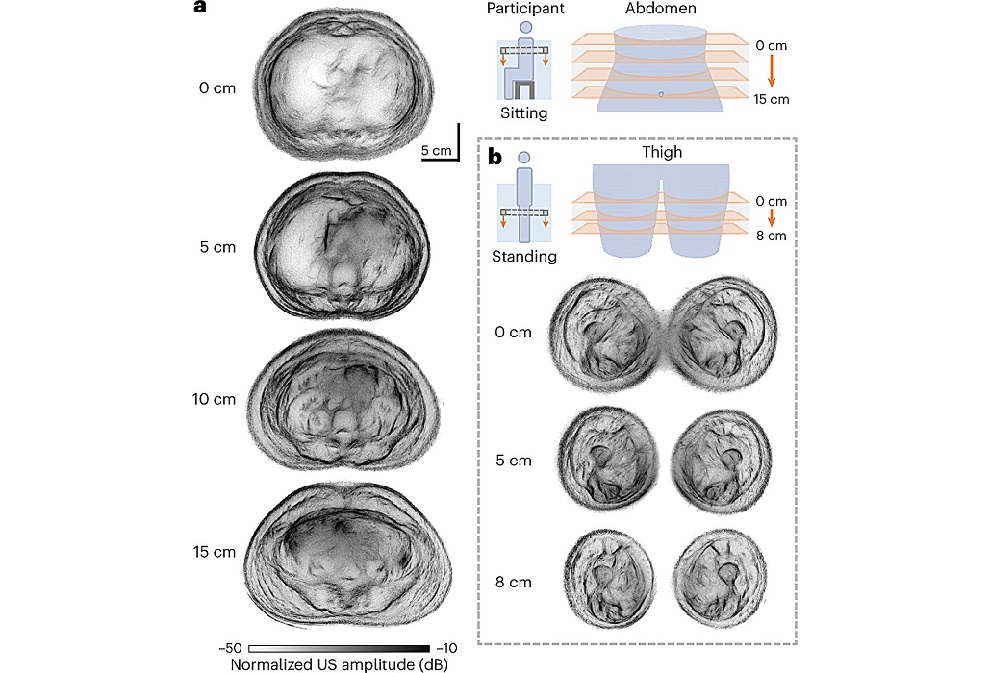
Whole Cross-Section Ultrasound System Enables Operator-Independent Imaging
Conventional ultrasound is central to bedside imaging but is limited by a narrow field of view and operator variability. Comprehensive cross-sectional assessment typically requires computed tomography... Read moreNuclear Medicine
view channel![Image: (A-C) Representative whole-body maximum-intensity projection images and regional fused PET/CT images from three histologically confirmed osteosarcoma patients who underwent paired [68Ga]Ga-B7-H3-BCH PET/CT and 18F-FDGE PET/CT within 7 days. (D) Multimodal imaging evaluation of patient 3, including X-ray, MRI (T2-weighted imaging, T2WI), CT, and B7-H3 PET/CT. (Photo courtesy of SNMMI) Image: (A-C) Representative whole-body maximum-intensity projection images and regional fused PET/CT images from three histologically confirmed osteosarcoma patients who underwent paired [68Ga]Ga-B7-H3-BCH PET/CT and 18F-FDGE PET/CT within 7 days. (D) Multimodal imaging evaluation of patient 3, including X-ray, MRI (T2-weighted imaging, T2WI), CT, and B7-H3 PET/CT. (Photo courtesy of SNMMI)](https://globetechcdn.com/mobile_medicalimaging/images/stories/articles/article_images/2026-06-07/294811110_image_1.jpg)
Targeted PET Platform Guides Osteosarcoma Resection and Margin Verification
Osteosarcoma, an aggressive primary bone cancer that mainly affects children and adolescents, demands wide excision to prevent local recurrence. Surgeons must achieve negative margins while preserving... Read more
Portable PET System Enables Real-Time Bedside Guidance for Biopsies and Ablations
Interventional radiology procedures typically rely on ultrasound, X-ray fluoroscopy, or computed tomography for image guidance. These modalities visualize anatomy but offer limited molecular information,... Read moreImaging IT
view channel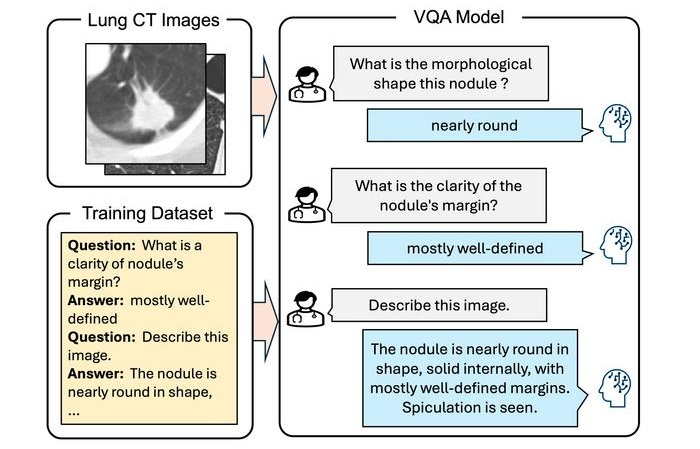
Interactive AI Tool Supports Explainable Lung Nodule Assessment
Lung cancer is a leading cause of cancer mortality, and timely characterization of pulmonary nodules on chest computed tomography (CT) is essential for directing care. Interpreting nodule morphology demands... Read more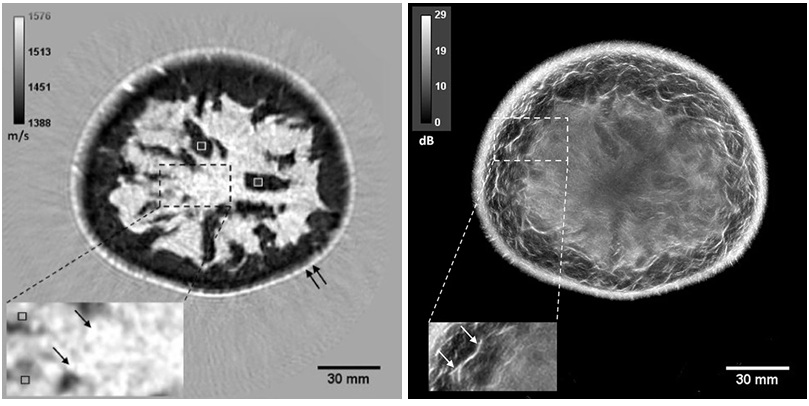
Breast Imaging Software Enhances Visualization and Tissue Characterization in Challenging Cases
Breast imaging can be particularly challenging in cases involving small breasts or implants, where image reconstruction and tissue characterization may be limited. Clinicians also need reproducible analysis... Read more
New Google Cloud Medical Imaging Suite Makes Imaging Healthcare Data More Accessible
Medical imaging is a critical tool used to diagnose patients, and there are billions of medical images scanned globally each year. Imaging data accounts for about 90% of all healthcare data1 and, until... Read more
Global AI in Medical Diagnostics Market to Be Driven by Demand for Image Recognition in Radiology
The global artificial intelligence (AI) in medical diagnostics market is expanding with early disease detection being one of its key applications and image recognition becoming a compelling consumer proposition... Read moreIndustry News
view channel
GE HealthCare Showcases AI-Enabled Nuclear Medicine Portfolio at SNMMI 2026
Nuclear medicine is expanding rapidly as health systems adopt theranostics and broaden access to radiopharmaceuticals, increasing demand for scalable operations and consistent diagnostic confidence.... Read more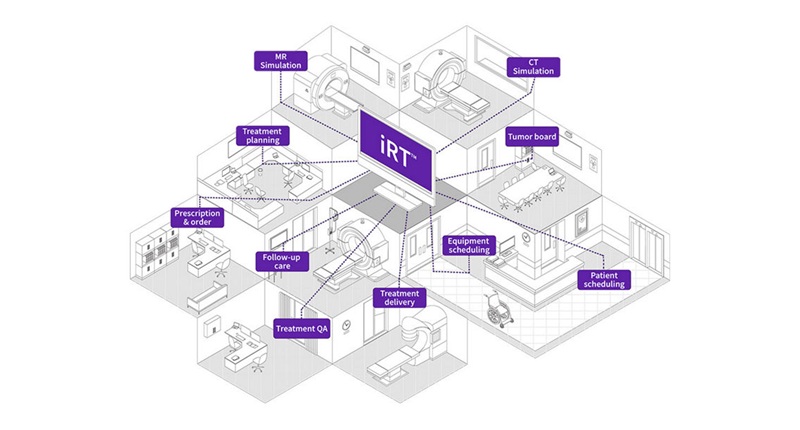
GE HealthCare Highlights AI-Supported Radiation Therapy Tools at ESTRO 2026
At the European Society for Radiotherapy and Oncology (ESTRO) 2026 Congress in Stockholm, GE HealthCare is highlighting Intelligent Radiation Therapy (iRT), MIM Software innovations, and BK Medical surgical... Read more