Perioperative Ultrasound Monitoring of Radial Artery Catheter Failure
|
By MedImaging International staff writers Posted on 09 Jun 2015 |
Using a hand carry ultrasound system, students and staff from the Department of Radiology/Ultrasound and Anesthesiology at Sidney Kimmel Medical College of Thomas Jefferson University recently finished a study of mechanisms related in the cause of radial artery catheter failure.
The study was presented at the 2015 WFUMB/AIUM Convention [UMB 41(4S):S125, 2015]. Radial artery catheters (RAC) are commonly used in the emergency department, operating rooms and critical care units of a hospital to accurately monitor the arterial blood pressure and acquire blood samples.
With the use of SonoScape’s S9 ultrasound system (SonoScape Medical corp.; Shenzhen, China), the researchers hoped to discover why RAC fail prematurely and the causes of complications related to RAC clinical use. The clinical trial was designed to determine the causes of RAC failure and to confirm if a low artery diameter to catheter diameter ratio leads to decreased local blood flow and thrombosis.
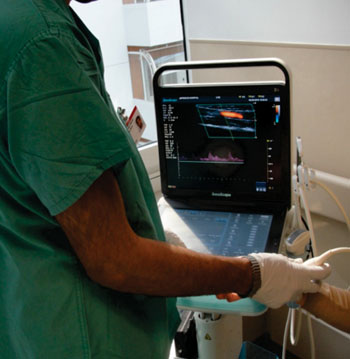
For this IRB-approved study, 25 patients requiring a RAC for clinical care were enrolled. To evaluate and monitor the RAC insertions as well as blood flow dynamics in the radial and ulnar arteries, the 25 patients were scanned with the S9 ultrasound system with a 12 MHz linear array probe.
They were scanned before RAC insertion, immediately after, and intermittently every two to four hours during the day and every four to six hours during the night (for 24 to 36 hours). By using the S9 ultrasound, they were able to literally see what was happening in the ulnar and radial arteries of the patients.
Using the S9’s grayscale and Doppler technology, measurements were taken of blood flow and the diameters of both the ulnar and radial arteries. Assessments of RAC insertion factors also allowed for measurements for the composite vessel trauma score for respective arteries after insertion. To analyze the data, a paired Student t-test and a Wilcoxon Rank-Sum test were used to compare results. For the purpose of the study, a RAC initial failure and final failure were classified as difficulty/inability to aspirate blood through the RAC or a dampening/loss of the blood pressure waveform.
Throughout the study, a total of 211 ultrasound scans were obtained from the 25 patients using the S9 ultrasound system. From the 25 patients, 21 experienced a RAC initial failure and four patients experienced a RAC final failure. With the S9’s high image clarity, the reasons for RAC failure were easily revealed. Each failed for a different reason: ranging from the catheter being outside of the vessel and in the subcutaneous tissue, the RA catheter tip was against the arterial wall, thrombus on the catheter tip partially/completely obstructed the RA catheter lumen, and thrombus within the RA lumen partially/completely obstructed RA blood flow.
Soon after RA catheter insertion, the RA and UA inner diameters increased from 2.21±0.4 mm to 2.54±0.45 mm and from 1.91±0.44 mm to 2.23±0.48 mm respectively (no significant differences in RA and UA diameters).
For the 24 RACs that did not have a final failure, the median number of cannulation attempts was 9 and the median CVTS was 8.5. Comparatively, the CVTS for the four RACS that developed a final failure was 8.3 and the mean number of blood draws was 5±3.3. Median time to initial dampening of the RA waveform was 5.9 hours in 22 different cases.
By using the S9’s color Doppler, the team was able to measure the velocities in the RA and UA arteries after RAC insertion. In the RA artery, the peak velocity decreased from 56.2±18.7 to 36.6 cm/s after the RAC was inserted. Peak velocity in the UA however, increased from 53.7±19.3 to 63.4±20.5 cm/s after insertion of the RAC. Ultrasound scans also did not indicate a difference in vessel diameter or blood flow velocity when comparing successful RACs to that of the four that developed a final failure; however this may be attributed to the limited number of final failures that were observed.
There was also no difference in velocity patterns or in diameter in the RACs that failed compared to those that did not fail.
The conclusions from this study are threefold. Both the RA and UA experienced significant dilation after RAC insertion. The data suggested that vasodilation and increased blood flow around the catheter may help to prevent thrombosis and protect the function of the arterial catheter. In some patients, the peak blood flow velocity significantly decreased after insertion of a 20 g catheter, especially in RA with a small inner diameter. With the S9’s high-resolution ultrasound imaging abilities, in vivo observations were possible to reveal what caused RAC failure during the patient’s clinical course. Failures consisted primarily of tortuous vascular anatomy and RAC tip obstruction, thrombus formation on the RAC tip, and partial/complete thrombosis of the RA lumen.
Related Links:
SonoScape Medical corp.
The study was presented at the 2015 WFUMB/AIUM Convention [UMB 41(4S):S125, 2015]. Radial artery catheters (RAC) are commonly used in the emergency department, operating rooms and critical care units of a hospital to accurately monitor the arterial blood pressure and acquire blood samples.
With the use of SonoScape’s S9 ultrasound system (SonoScape Medical corp.; Shenzhen, China), the researchers hoped to discover why RAC fail prematurely and the causes of complications related to RAC clinical use. The clinical trial was designed to determine the causes of RAC failure and to confirm if a low artery diameter to catheter diameter ratio leads to decreased local blood flow and thrombosis.
For this IRB-approved study, 25 patients requiring a RAC for clinical care were enrolled. To evaluate and monitor the RAC insertions as well as blood flow dynamics in the radial and ulnar arteries, the 25 patients were scanned with the S9 ultrasound system with a 12 MHz linear array probe.
They were scanned before RAC insertion, immediately after, and intermittently every two to four hours during the day and every four to six hours during the night (for 24 to 36 hours). By using the S9 ultrasound, they were able to literally see what was happening in the ulnar and radial arteries of the patients.
Using the S9’s grayscale and Doppler technology, measurements were taken of blood flow and the diameters of both the ulnar and radial arteries. Assessments of RAC insertion factors also allowed for measurements for the composite vessel trauma score for respective arteries after insertion. To analyze the data, a paired Student t-test and a Wilcoxon Rank-Sum test were used to compare results. For the purpose of the study, a RAC initial failure and final failure were classified as difficulty/inability to aspirate blood through the RAC or a dampening/loss of the blood pressure waveform.
Throughout the study, a total of 211 ultrasound scans were obtained from the 25 patients using the S9 ultrasound system. From the 25 patients, 21 experienced a RAC initial failure and four patients experienced a RAC final failure. With the S9’s high image clarity, the reasons for RAC failure were easily revealed. Each failed for a different reason: ranging from the catheter being outside of the vessel and in the subcutaneous tissue, the RA catheter tip was against the arterial wall, thrombus on the catheter tip partially/completely obstructed the RA catheter lumen, and thrombus within the RA lumen partially/completely obstructed RA blood flow.
Soon after RA catheter insertion, the RA and UA inner diameters increased from 2.21±0.4 mm to 2.54±0.45 mm and from 1.91±0.44 mm to 2.23±0.48 mm respectively (no significant differences in RA and UA diameters).
For the 24 RACs that did not have a final failure, the median number of cannulation attempts was 9 and the median CVTS was 8.5. Comparatively, the CVTS for the four RACS that developed a final failure was 8.3 and the mean number of blood draws was 5±3.3. Median time to initial dampening of the RA waveform was 5.9 hours in 22 different cases.
By using the S9’s color Doppler, the team was able to measure the velocities in the RA and UA arteries after RAC insertion. In the RA artery, the peak velocity decreased from 56.2±18.7 to 36.6 cm/s after the RAC was inserted. Peak velocity in the UA however, increased from 53.7±19.3 to 63.4±20.5 cm/s after insertion of the RAC. Ultrasound scans also did not indicate a difference in vessel diameter or blood flow velocity when comparing successful RACs to that of the four that developed a final failure; however this may be attributed to the limited number of final failures that were observed.
There was also no difference in velocity patterns or in diameter in the RACs that failed compared to those that did not fail.
The conclusions from this study are threefold. Both the RA and UA experienced significant dilation after RAC insertion. The data suggested that vasodilation and increased blood flow around the catheter may help to prevent thrombosis and protect the function of the arterial catheter. In some patients, the peak blood flow velocity significantly decreased after insertion of a 20 g catheter, especially in RA with a small inner diameter. With the S9’s high-resolution ultrasound imaging abilities, in vivo observations were possible to reveal what caused RAC failure during the patient’s clinical course. Failures consisted primarily of tortuous vascular anatomy and RAC tip obstruction, thrombus formation on the RAC tip, and partial/complete thrombosis of the RA lumen.
Related Links:
SonoScape Medical corp.
Read the full article by registering today, it's FREE! 

Register now for FREE to MedImaging.net and get complete access to news and events that shape the world of Radiology. 
- Free digital version edition of Medical Imaging International sent by email on regular basis
- Free print version of Medical Imaging International magazine (available only outside USA and Canada).
- Free and unlimited access to back issues of Medical Imaging International in digital format
- Free Medical Imaging International Newsletter sent every week containing the latest news
- Free breaking news sent via email
- Free access to Events Calendar
- Free access to LinkXpress new product services
- REGISTRATION IS FREE AND EASY!
Sign in: Registered website members
Sign in: Registered magazine subscribers
Latest Ultrasound News
- Tiny Magnetic Robot Takes 3D Scans from Deep Within Body
- High Resolution Ultrasound Speeds Up Prostate Cancer Diagnosis
- World's First Wireless, Handheld, Whole-Body Ultrasound with Single PZT Transducer Makes Imaging More Accessible
- Artificial Intelligence Detects Undiagnosed Liver Disease from Echocardiograms
- Ultrasound Imaging Non-Invasively Tracks Tumor Response to Radiation and Immunotherapy
- AI Improves Detection of Congenital Heart Defects on Routine Prenatal Ultrasounds
- AI Diagnoses Lung Diseases from Ultrasound Videos with 96.57% Accuracy
- New Contrast Agent for Ultrasound Imaging Ensures Affordable and Safer Medical Diagnostics
- Ultrasound-Directed Microbubbles Boost Immune Response Against Tumors
- POC Ultrasound Enhances Early Pregnancy Care and Cuts Emergency Visits
- AI-Based Models Outperform Human Experts at Identifying Ovarian Cancer in Ultrasound Images
- Automated Breast Ultrasound Provides Alternative to Mammography in Low-Resource Settings
- Transparent Ultrasound Transducer for Photoacoustic and Ultrasound Endoscopy to Improve Diagnostic Accuracy
- Wearable Ultrasound Patch Enables Continuous Blood Pressure Monitoring
- AI Image-Recognition Program Reads Echocardiograms Faster, Cuts Results Wait Time
- Ultrasound Device Non-Invasively Improves Blood Circulation in Lower Limbs
Channels
Radiography
view channel
AI-Powered Imaging Technique Shows Promise in Evaluating Patients for PCI
Percutaneous coronary intervention (PCI), also known as coronary angioplasty, is a minimally invasive procedure where small metal tubes called stents are inserted into partially blocked coronary arteries... Read more
Higher Chest X-Ray Usage Catches Lung Cancer Earlier and Improves Survival
Lung cancer continues to be the leading cause of cancer-related deaths worldwide. While advanced technologies like CT scanners play a crucial role in detecting lung cancer, more accessible and affordable... Read moreMRI
view channel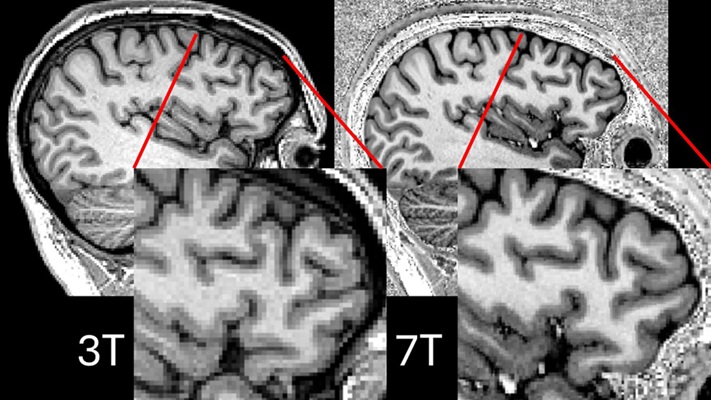
Ultra-Powerful MRI Scans Enable Life-Changing Surgery in Treatment-Resistant Epileptic Patients
Approximately 360,000 individuals in the UK suffer from focal epilepsy, a condition in which seizures spread from one part of the brain. Around a third of these patients experience persistent seizures... Read more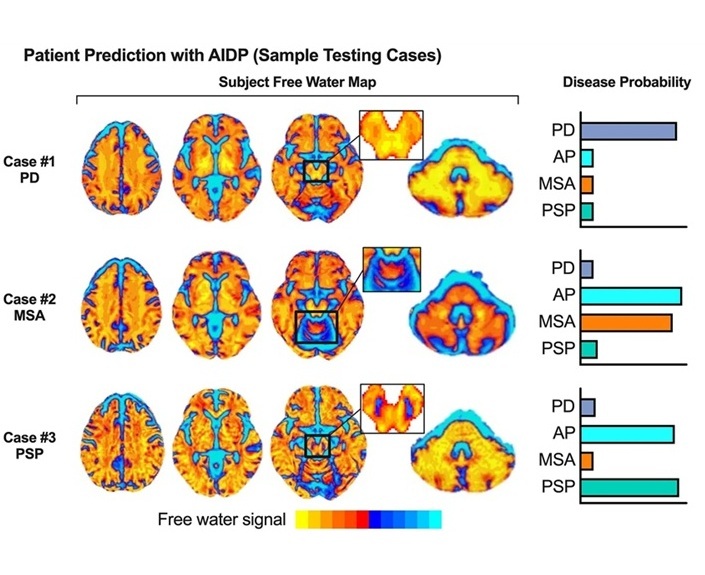
AI-Powered MRI Technology Improves Parkinson’s Diagnoses
Current research shows that the accuracy of diagnosing Parkinson’s disease typically ranges from 55% to 78% within the first five years of assessment. This is partly due to the similarities shared by Parkinson’s... Read more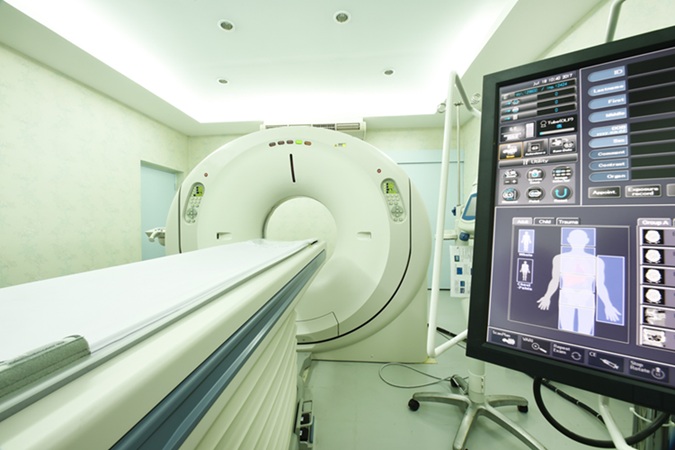
Biparametric MRI Combined with AI Enhances Detection of Clinically Significant Prostate Cancer
Artificial intelligence (AI) technologies are transforming the way medical images are analyzed, offering unprecedented capabilities in quantitatively extracting features that go beyond traditional visual... Read more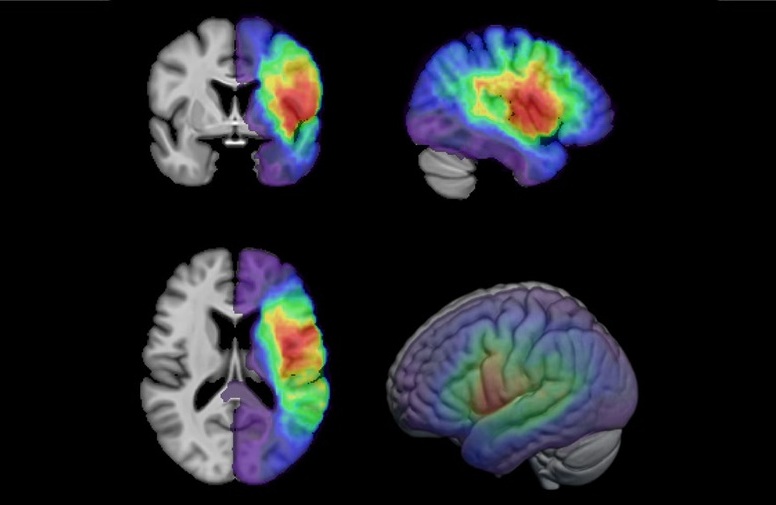
First-Of-Its-Kind AI-Driven Brain Imaging Platform to Better Guide Stroke Treatment Options
Each year, approximately 800,000 people in the U.S. experience strokes, with marginalized and minoritized groups being disproportionately affected. Strokes vary in terms of size and location within the... Read moreNuclear Medicine
view channel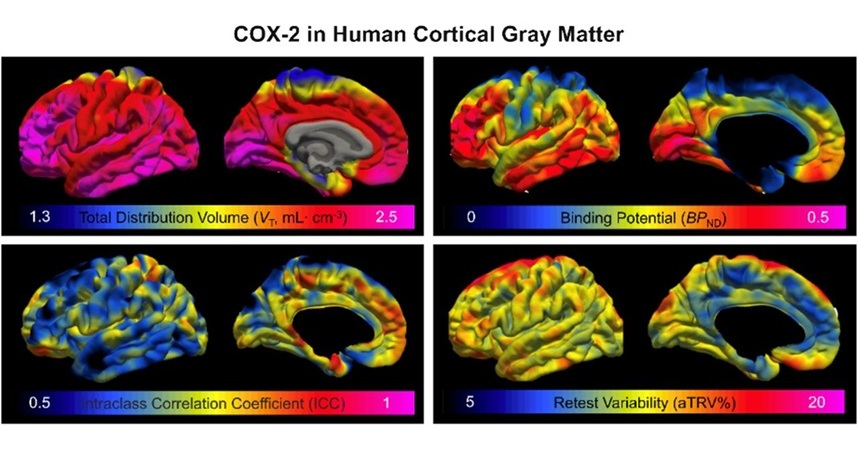
Novel PET Imaging Approach Offers Never-Before-Seen View of Neuroinflammation
COX-2, an enzyme that plays a key role in brain inflammation, can be significantly upregulated by inflammatory stimuli and neuroexcitation. Researchers suggest that COX-2 density in the brain could serve... Read more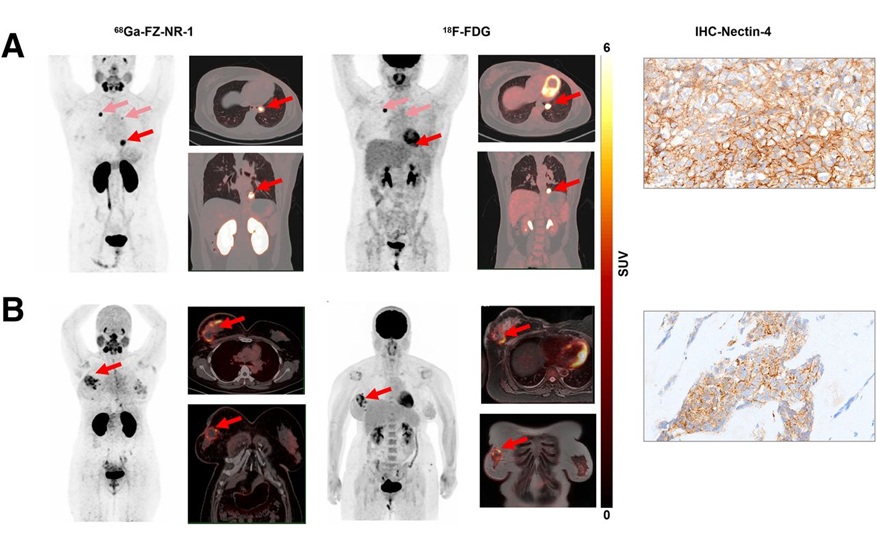
Novel Radiotracer Identifies Biomarker for Triple-Negative Breast Cancer
Triple-negative breast cancer (TNBC), which represents 15-20% of all breast cancer cases, is one of the most aggressive subtypes, with a five-year survival rate of about 40%. Due to its significant heterogeneity... Read moreGeneral/Advanced Imaging
view channel
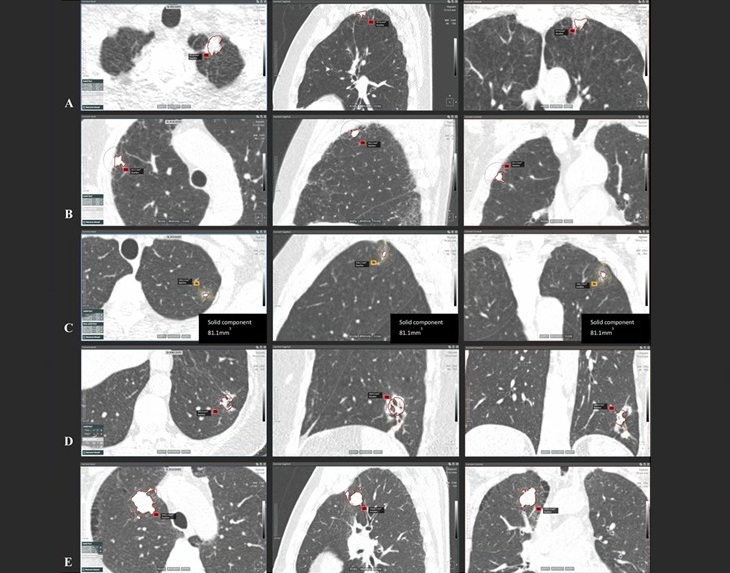
AI-Powered Imaging System Improves Lung Cancer Diagnosis
Given the need to detect lung cancer at earlier stages, there is an increasing need for a definitive diagnostic pathway for patients with suspicious pulmonary nodules. However, obtaining tissue samples... Read more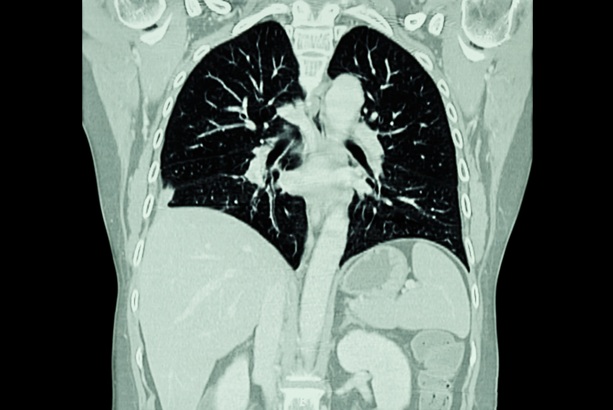
AI Model Significantly Enhances Low-Dose CT Capabilities
Lung cancer remains one of the most challenging diseases, making early diagnosis vital for effective treatment. Fortunately, advancements in artificial intelligence (AI) are revolutionizing lung cancer... Read moreImaging IT
view channel
New Google Cloud Medical Imaging Suite Makes Imaging Healthcare Data More Accessible
Medical imaging is a critical tool used to diagnose patients, and there are billions of medical images scanned globally each year. Imaging data accounts for about 90% of all healthcare data1 and, until... Read more
Global AI in Medical Diagnostics Market to Be Driven by Demand for Image Recognition in Radiology
The global artificial intelligence (AI) in medical diagnostics market is expanding with early disease detection being one of its key applications and image recognition becoming a compelling consumer proposition... Read moreIndustry News
view channel
GE HealthCare and NVIDIA Collaboration to Reimagine Diagnostic Imaging
GE HealthCare (Chicago, IL, USA) has entered into a collaboration with NVIDIA (Santa Clara, CA, USA), expanding the existing relationship between the two companies to focus on pioneering innovation in... Read more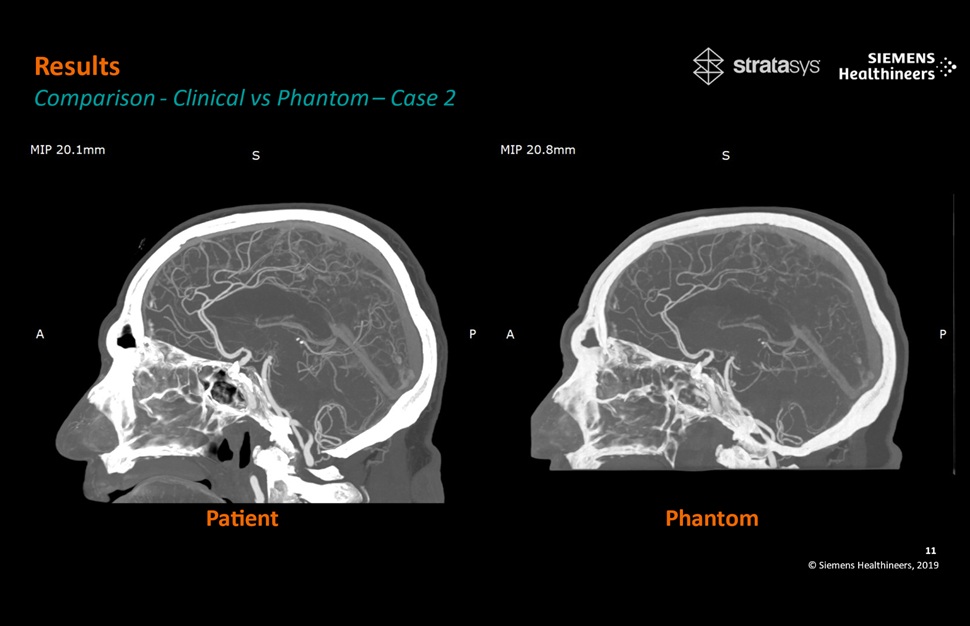
Patient-Specific 3D-Printed Phantoms Transform CT Imaging
New research has highlighted how anatomically precise, patient-specific 3D-printed phantoms are proving to be scalable, cost-effective, and efficient tools in the development of new CT scan algorithms... Read more
Siemens and Sectra Collaborate on Enhancing Radiology Workflows
Siemens Healthineers (Forchheim, Germany) and Sectra (Linköping, Sweden) have entered into a collaboration aimed at enhancing radiologists' diagnostic capabilities and, in turn, improving patient care... Read more






 Guided Devices.jpg)