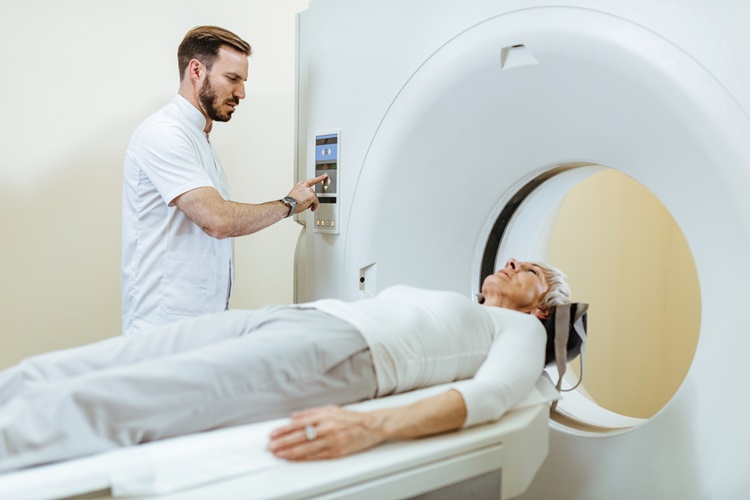
Repeat Nuclear and CT Imaging Increases Breast Cancer Risk
|
By MedImaging International staff writers Posted on 19 Dec 2012 |
Researchers reviewing the records of approximately 250,000 women enrolled in an integrated healthcare delivery system revealed that increased computed tomography (CT) scanning utilization between 2000 and 2010 could result in a rise in the risk of breast cancer for specific women, including younger patients and those who received repeat scans. According to the study, nuclear medicine imaging may also be a factor for increased breast cancer risk.
The study’s findings were presented in November 2012 at the annual meeting of the Radiological Society of North America (RSNA), held in Chicago (IL, USA). CT uses ionizing radiation in the form of X-rays to generate cross-sectional images of the body. In nuclear medicine imaging, a radiopharmaceutical--a compound that includes a small amount of a radioactive material--is delivered inside the body to help visualize internal organs.
“When a woman undergoes CT or nuclear medicine imaging of her chest, abdomen or spine, her breast tissue will absorb some radiation,” said senior author Rebecca Smith-Bindman, MD, professor of radiology and biomedical imaging at the University of California, San Francisco (USA). “Breast tissue is one of the tissues in the body known to be sensitive to developing cancer as a result of radiation exposure.”
The study, led by Ginger Merry, MD, MPH, breast imaging fellow at Prentice Women’s Hospital-Northwestern Memorial Hospital ( Chicago, IL, USA) found that among the system’s female enrollees, CT utilization increased from 99.8 CT scans per 1,000 women in 2000 to 192.4 CT scans per 1,000 women in 2010 (a yearly increase of 6.8%). In 2010, 46% of those CT scans exposed the breast to radiation. Nuclear medicine imaging decreased from 39.3 scans per 1,000 women in 2000 to 27.5 scans per 1,000 women in 2010 (a 3.5% yearly decline); however, in 2010, 84% of nuclear medicine studies exposed the breast to radiation.
“Until now, the impact of this increased use of imaging on radiation exposure to breast tissue and the subsequent risk of breast cancer has not been known,” Dr. Smith-Bindman said. “Our goal was to quantify imaging utilization and radiation exposure to the breast among women enrolled in an integrated healthcare delivery system and to use these data to determine the imaging-related risk of breast cancer from those studies.”
The investigators gathered CT dose data from 1,656 patients who underwent CT scanning that exposed the breast to radiation, and employing a new automated computational strategy, estimated the patients’ effective radiation dose and the amount of radiation absorbed by the breast. The researchers also analyzed the radiopharmaceutical volume and associated radiation exposure used in 5,507 nuclear medicine exams that exposed the breast to radiation.
“We found that the estimated breast radiation doses from CT were highly variable across patients, with the highest doses coming from multiple-phase cardiac and chest CT examinations, where successive images of the organ being studied are captured,” Dr. Smith-Bindman said.
The researchers then estimated the women’s imaging-related risk of breast cancer and compared it to their underlying risk of developing breast cancer. Each woman’s 10-year imaging-related risk of developing breast cancer, starting 10 years after her exposure to imaging and based on her age at exposure, was estimated using the breast-specific radiation data and a statistical risk model. A women’s underlying risk of developing breast cancer was estimated based on data collected by the US National Cancer Institute-funded Breast Cancer Surveillance Consortium.
“Young women receiving several chest and or cardiac CTs had the greatest increased risk of developing breast cancer at approximately 20%,” said Diana Miglioretti, PhD, study coauthor and senior investigator at the Group Health Research Institute (Seattle, WA, USA). “A 15-year-old girl with no risk factors for breast cancer would double her 10-year risk of developing breast cancer at 25.”
Dr. Smith-Bindman noted that, to lower the imaging-related risk of developing breast cancer, imaging providers should assess the radiation doses associated with each exam, reduce the use of multiphase protocols, and employ dose-reduction software wherever possible to lessen exposures.
“If imaging is truly indicated, then the risk of developing cancer is small and should not dissuade women from getting the test they need,” Dr. Smith-Bindman said. “On the other hand, a lot of patients are undergoing repeat chest and cardiac CT, many of which aren’t necessary. Women, and particularly young women, should understand there is a small but real potential risk of breast cancer associated with cardiac and chest CT, and the risk increases with the number of scans.”
Related Links:
University of California, San Francisco
Group Health Research Institute
Prentice Women’s Hospital-Northwestern Memorial Hospital
The study’s findings were presented in November 2012 at the annual meeting of the Radiological Society of North America (RSNA), held in Chicago (IL, USA). CT uses ionizing radiation in the form of X-rays to generate cross-sectional images of the body. In nuclear medicine imaging, a radiopharmaceutical--a compound that includes a small amount of a radioactive material--is delivered inside the body to help visualize internal organs.
“When a woman undergoes CT or nuclear medicine imaging of her chest, abdomen or spine, her breast tissue will absorb some radiation,” said senior author Rebecca Smith-Bindman, MD, professor of radiology and biomedical imaging at the University of California, San Francisco (USA). “Breast tissue is one of the tissues in the body known to be sensitive to developing cancer as a result of radiation exposure.”
The study, led by Ginger Merry, MD, MPH, breast imaging fellow at Prentice Women’s Hospital-Northwestern Memorial Hospital ( Chicago, IL, USA) found that among the system’s female enrollees, CT utilization increased from 99.8 CT scans per 1,000 women in 2000 to 192.4 CT scans per 1,000 women in 2010 (a yearly increase of 6.8%). In 2010, 46% of those CT scans exposed the breast to radiation. Nuclear medicine imaging decreased from 39.3 scans per 1,000 women in 2000 to 27.5 scans per 1,000 women in 2010 (a 3.5% yearly decline); however, in 2010, 84% of nuclear medicine studies exposed the breast to radiation.
“Until now, the impact of this increased use of imaging on radiation exposure to breast tissue and the subsequent risk of breast cancer has not been known,” Dr. Smith-Bindman said. “Our goal was to quantify imaging utilization and radiation exposure to the breast among women enrolled in an integrated healthcare delivery system and to use these data to determine the imaging-related risk of breast cancer from those studies.”
The investigators gathered CT dose data from 1,656 patients who underwent CT scanning that exposed the breast to radiation, and employing a new automated computational strategy, estimated the patients’ effective radiation dose and the amount of radiation absorbed by the breast. The researchers also analyzed the radiopharmaceutical volume and associated radiation exposure used in 5,507 nuclear medicine exams that exposed the breast to radiation.
“We found that the estimated breast radiation doses from CT were highly variable across patients, with the highest doses coming from multiple-phase cardiac and chest CT examinations, where successive images of the organ being studied are captured,” Dr. Smith-Bindman said.
The researchers then estimated the women’s imaging-related risk of breast cancer and compared it to their underlying risk of developing breast cancer. Each woman’s 10-year imaging-related risk of developing breast cancer, starting 10 years after her exposure to imaging and based on her age at exposure, was estimated using the breast-specific radiation data and a statistical risk model. A women’s underlying risk of developing breast cancer was estimated based on data collected by the US National Cancer Institute-funded Breast Cancer Surveillance Consortium.
“Young women receiving several chest and or cardiac CTs had the greatest increased risk of developing breast cancer at approximately 20%,” said Diana Miglioretti, PhD, study coauthor and senior investigator at the Group Health Research Institute (Seattle, WA, USA). “A 15-year-old girl with no risk factors for breast cancer would double her 10-year risk of developing breast cancer at 25.”
Dr. Smith-Bindman noted that, to lower the imaging-related risk of developing breast cancer, imaging providers should assess the radiation doses associated with each exam, reduce the use of multiphase protocols, and employ dose-reduction software wherever possible to lessen exposures.
“If imaging is truly indicated, then the risk of developing cancer is small and should not dissuade women from getting the test they need,” Dr. Smith-Bindman said. “On the other hand, a lot of patients are undergoing repeat chest and cardiac CT, many of which aren’t necessary. Women, and particularly young women, should understand there is a small but real potential risk of breast cancer associated with cardiac and chest CT, and the risk increases with the number of scans.”
Related Links:
University of California, San Francisco
Group Health Research Institute
Prentice Women’s Hospital-Northwestern Memorial Hospital
Latest Radiography News
- World's Largest Class Single Crystal Diamond Radiation Detector Opens New Possibilities for Diagnostic Imaging
- AI-Powered Imaging Technique Shows Promise in Evaluating Patients for PCI
- Higher Chest X-Ray Usage Catches Lung Cancer Earlier and Improves Survival
- AI-Powered Mammograms Predict Cardiovascular Risk
- Generative AI Model Significantly Reduces Chest X-Ray Reading Time
- AI-Powered Mammography Screening Boosts Cancer Detection in Single-Reader Settings
- Photon Counting Detectors Promise Fast Color X-Ray Images
- AI Can Flag Mammograms for Supplemental MRI
- 3D CT Imaging from Single X-Ray Projection Reduces Radiation Exposure
- AI Method Accurately Predicts Breast Cancer Risk by Analyzing Multiple Mammograms
- Printable Organic X-Ray Sensors Could Transform Treatment for Cancer Patients
- Highly Sensitive, Foldable Detector to Make X-Rays Safer
- Novel Breast Cancer Screening Technology Could Offer Superior Alternative to Mammogram
- Artificial Intelligence Accurately Predicts Breast Cancer Years Before Diagnosis
- AI-Powered Chest X-Ray Detects Pulmonary Nodules Three Years Before Lung Cancer Symptoms
- AI Model Identifies Vertebral Compression Fractures in Chest Radiographs
Channels
MRI
view channel
AI Tool Tracks Effectiveness of Multiple Sclerosis Treatments Using Brain MRI Scans
Multiple sclerosis (MS) is a condition in which the immune system attacks the brain and spinal cord, leading to impairments in movement, sensation, and cognition. Magnetic Resonance Imaging (MRI) markers... Read more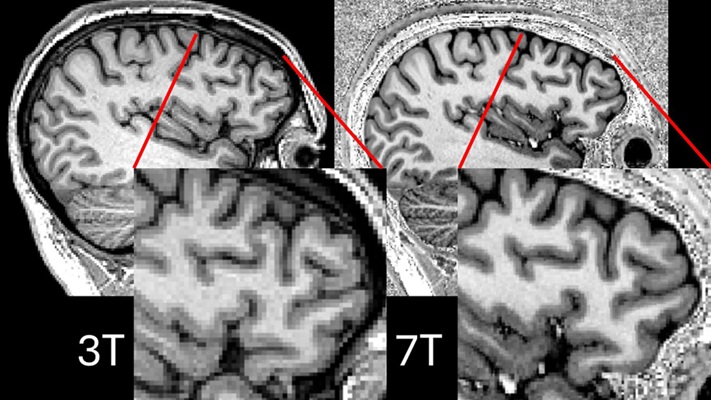
Ultra-Powerful MRI Scans Enable Life-Changing Surgery in Treatment-Resistant Epileptic Patients
Approximately 360,000 individuals in the UK suffer from focal epilepsy, a condition in which seizures spread from one part of the brain. Around a third of these patients experience persistent seizures... Read more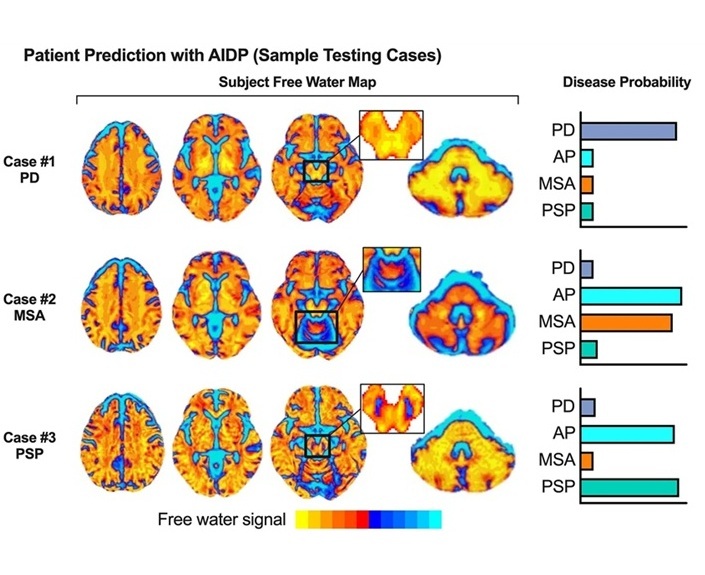
AI-Powered MRI Technology Improves Parkinson’s Diagnoses
Current research shows that the accuracy of diagnosing Parkinson’s disease typically ranges from 55% to 78% within the first five years of assessment. This is partly due to the similarities shared by Parkinson’s... Read more
Biparametric MRI Combined with AI Enhances Detection of Clinically Significant Prostate Cancer
Artificial intelligence (AI) technologies are transforming the way medical images are analyzed, offering unprecedented capabilities in quantitatively extracting features that go beyond traditional visual... Read moreUltrasound
view channel.jpeg)
AI-Powered Lung Ultrasound Outperforms Human Experts in Tuberculosis Diagnosis
Despite global declines in tuberculosis (TB) rates in previous years, the incidence of TB rose by 4.6% from 2020 to 2023. Early screening and rapid diagnosis are essential elements of the World Health... Read more
AI Identifies Heart Valve Disease from Common Imaging Test
Tricuspid regurgitation is a condition where the heart's tricuspid valve does not close completely during contraction, leading to backward blood flow, which can result in heart failure. A new artificial... Read moreNuclear Medicine
view channel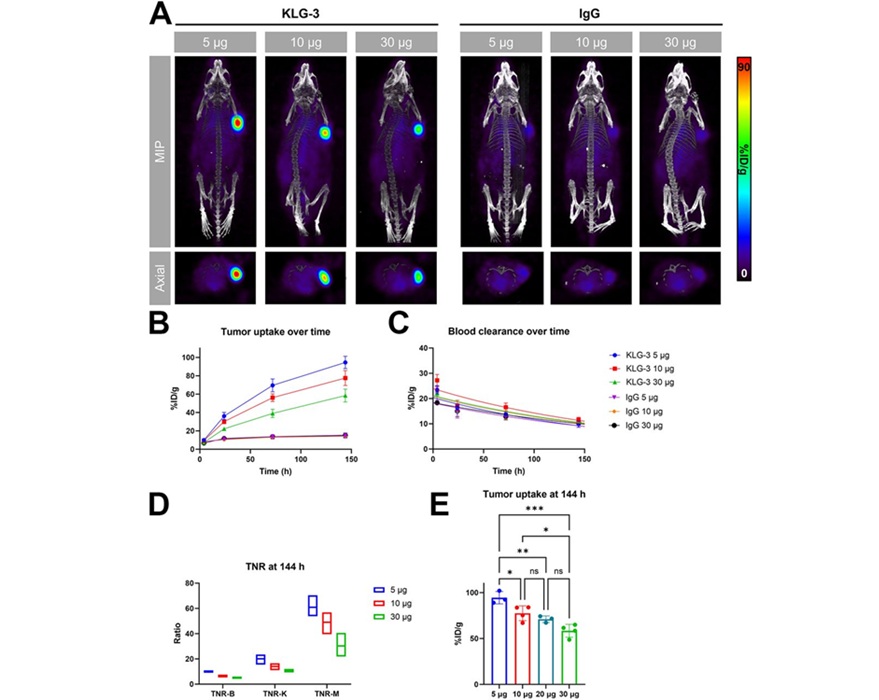
Novel Radiolabeled Antibody Improves Diagnosis and Treatment of Solid Tumors
Interleukin-13 receptor α-2 (IL13Rα2) is a cell surface receptor commonly found in solid tumors such as glioblastoma, melanoma, and breast cancer. It is minimally expressed in normal tissues, making it... Read more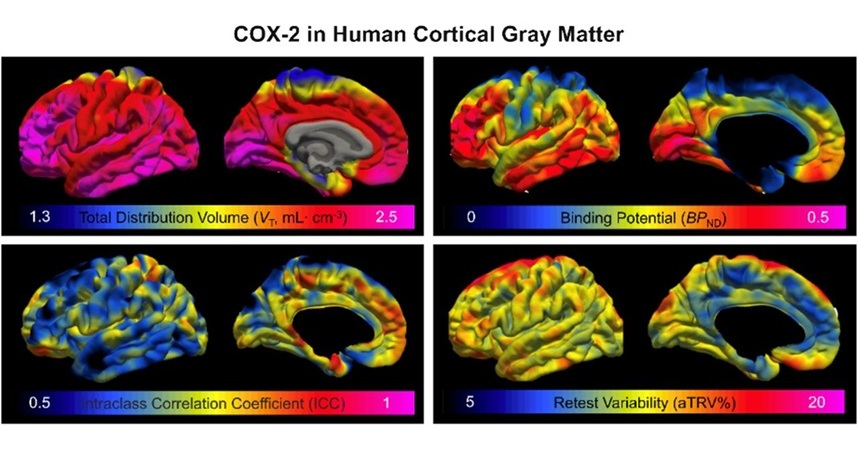
Novel PET Imaging Approach Offers Never-Before-Seen View of Neuroinflammation
COX-2, an enzyme that plays a key role in brain inflammation, can be significantly upregulated by inflammatory stimuli and neuroexcitation. Researchers suggest that COX-2 density in the brain could serve... Read moreGeneral/Advanced Imaging
view channel
AI-Powered Imaging System Improves Lung Cancer Diagnosis
Given the need to detect lung cancer at earlier stages, there is an increasing need for a definitive diagnostic pathway for patients with suspicious pulmonary nodules. However, obtaining tissue samples... Read more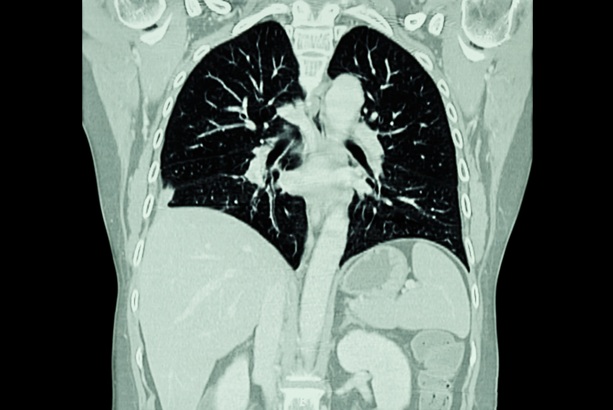
AI Model Significantly Enhances Low-Dose CT Capabilities
Lung cancer remains one of the most challenging diseases, making early diagnosis vital for effective treatment. Fortunately, advancements in artificial intelligence (AI) are revolutionizing lung cancer... Read moreImaging IT
view channel
New Google Cloud Medical Imaging Suite Makes Imaging Healthcare Data More Accessible
Medical imaging is a critical tool used to diagnose patients, and there are billions of medical images scanned globally each year. Imaging data accounts for about 90% of all healthcare data1 and, until... Read more
Global AI in Medical Diagnostics Market to Be Driven by Demand for Image Recognition in Radiology
The global artificial intelligence (AI) in medical diagnostics market is expanding with early disease detection being one of its key applications and image recognition becoming a compelling consumer proposition... Read moreIndustry News
view channel
GE HealthCare and NVIDIA Collaboration to Reimagine Diagnostic Imaging
GE HealthCare (Chicago, IL, USA) has entered into a collaboration with NVIDIA (Santa Clara, CA, USA), expanding the existing relationship between the two companies to focus on pioneering innovation in... Read more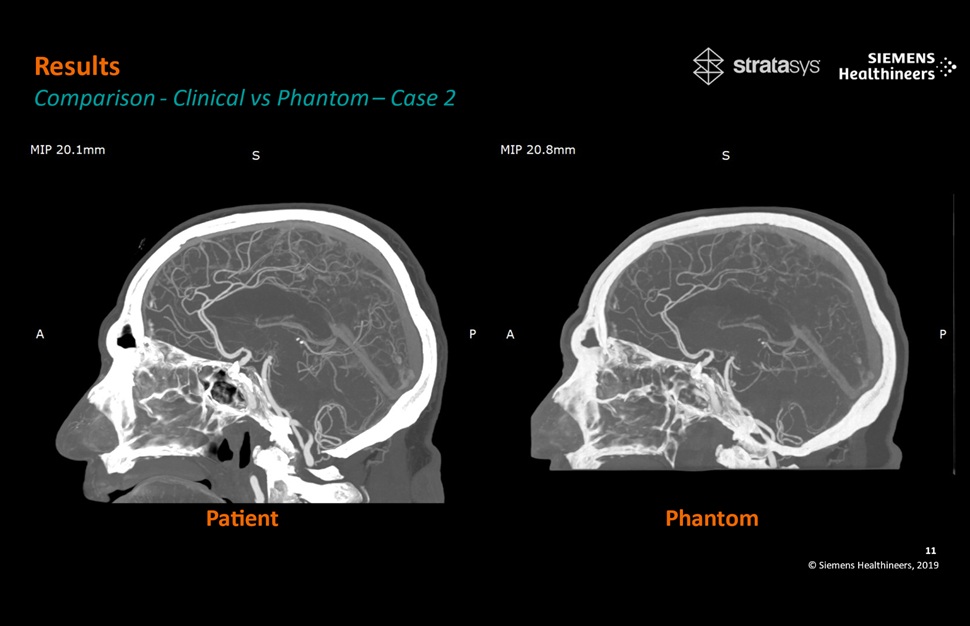
Patient-Specific 3D-Printed Phantoms Transform CT Imaging
New research has highlighted how anatomically precise, patient-specific 3D-printed phantoms are proving to be scalable, cost-effective, and efficient tools in the development of new CT scan algorithms... Read more
Siemens and Sectra Collaborate on Enhancing Radiology Workflows
Siemens Healthineers (Forchheim, Germany) and Sectra (Linköping, Sweden) have entered into a collaboration aimed at enhancing radiologists' diagnostic capabilities and, in turn, improving patient care... Read more