Cardiac Stress Imaging More Frequent in the US among Patients whose Physicians Bill for Procedures
|
By MedImaging International staff writers Posted on 30 Nov 2011 |
In the United States, patients treated by physicians who billed for both technical (practice/equipment) and professional (supervision/ interpretation) elements of nuclear and echocardiographic stress imaging tests were more prone to undergo such tests after coronary revascularization compared with patients of physicians who did not charge for these services, according to a recent study.
The study’s findings were published in the November 9, 2011, issue of the Journal of the American Medical Association (JAMA). “Cardiac stress testing procedures performed in the office setting can enable more rapid, efficient diagnostic testing and use of these procedures has increased significantly during the past decade. However, physician ownership of imaging equipment also could potentially induce testing in more discretionary situations, because the capital outlay for equipment is high and these investments must be recouped via procedure-related “technical fees,” which cover associated equipment and practice costs. Similar concerns have been raised regarding whether physicians who bill for the professional fees covering test interpretation might more often refer their own patients for these tests than those who do not bill for these services. However, little is known about how these reimbursement incentives might affect the routine use of cardiac stress testing,” according to the authors.
The American College of Cardiology Foundation (ACCF; Rockville, MD, USA) has published appropriateness utilization criteria (AUC) to provide guidance to clinicians for appropriate testing. Current AUC guidelines do not recommend routine testing within two years for patients undergoing percutaneous coronary intervention (PCI; procedures such as balloon angioplasty or stent placement used to open narrowed coronary arteries) or within five years for patients having coronary artery bypass graft (CABG) surgery, unless the need for stress testing is motivated by symptoms or events.
Bimal R. Shah, MD, MBA, from Duke University Medical Center (Durham, NC, USA, and colleagues assessed whether there was a link between patients undergoing cardiac stress imaging after coronary revascularization and the pattern of stress imaging billing of the physician practice providing their follow-up care. Using data from a US health insurance carrier, 17,847 patients were identified who between November 2004 and June 2007 had coronary revascularization and an index cardiac outpatient visit more than 90 days following the procedure. Based on overall billings, physicians were categorized into three classifications: physicians who routinely charged for technical and professional fees; physicians who regularly billed for professional fees only; and physicians who did not routinely bill for either service. Analytic models were used to evaluate the association between physician billing and use of stress testing, after adjusting for patient and other physician factors.
During the study period, the overall 30-day incidence of either nuclear stress testing or stress echocardiography testing associated with the index cardiac-related outpatient visit was 12.2%, with an overall incidence of 10.4% for nuclear stress testing and 1.8% for stress echocardiography. The incidence of nuclear stress testing among clinicians who billed for both technical and professional fees, professional-only fees, and neither fee for nuclear stress testing was 12.6%, 8.8%, and 5.0%, respectively. The stress echocardiography testing incidence among physicians who billed for both technical and professional fees, professional-only fees, and neither fee for stress echocardiography was 2.8%, 1.4%, and 0.4%, respectively.
Data analysis revealed that physicians who billed for technical and professional fees for nuclear stress testing and those who billed for professional fees only were more likely to perform nuclear stress tests following revascularization than those not billing (13.3% and 9.4% vs. 5.3%). Physicians who billed for technical and professional fees for stress echocardiography testing or professional fees only were more likely to perform stress echocardiography testing following revascularization than those not billing (3.1% and 1.5 percent vs. 0.5%).
The investigators reported that even though current ACCF AUC do not recommend regular use of early stress testing following coronary revascularization, they found that 12% of patients with a cardiac-related outpatient visit at least three months after revascularization underwent a stress test within 30 days of their visit. Moreover, up to one in 10 patients who were not classified as having symptoms at their outpatient visit still underwent stress testing.
“Our study highlights the need for application of the ACCF AUC in clinical practice and augments findings of other studies that have explicitly examined application of ACCF AUC for nuclear stress and stress echocardiography. The ACCF AUC provides guidance to clinicians regarding when to pursue cardiac stress testing to assist in narrowing variation in testing among clinicians and practices. Discretionary stress testing after revascularization has potential financial and clinical disadvantages for patients, including the costs of the tests, the exposure to ionizing radiation as well as potential down-stream costs, and consequences from following up false-positive test results,” the researchers concluded in their article. “These data suggest the need for broader application of AUC to minimize the possible influence of financial incentives on the decision to perform cardiac stress testing after revascularization.”
Related Links:
American College of Cardiology Foundation
Duke University Medical Center
The study’s findings were published in the November 9, 2011, issue of the Journal of the American Medical Association (JAMA). “Cardiac stress testing procedures performed in the office setting can enable more rapid, efficient diagnostic testing and use of these procedures has increased significantly during the past decade. However, physician ownership of imaging equipment also could potentially induce testing in more discretionary situations, because the capital outlay for equipment is high and these investments must be recouped via procedure-related “technical fees,” which cover associated equipment and practice costs. Similar concerns have been raised regarding whether physicians who bill for the professional fees covering test interpretation might more often refer their own patients for these tests than those who do not bill for these services. However, little is known about how these reimbursement incentives might affect the routine use of cardiac stress testing,” according to the authors.
The American College of Cardiology Foundation (ACCF; Rockville, MD, USA) has published appropriateness utilization criteria (AUC) to provide guidance to clinicians for appropriate testing. Current AUC guidelines do not recommend routine testing within two years for patients undergoing percutaneous coronary intervention (PCI; procedures such as balloon angioplasty or stent placement used to open narrowed coronary arteries) or within five years for patients having coronary artery bypass graft (CABG) surgery, unless the need for stress testing is motivated by symptoms or events.
Bimal R. Shah, MD, MBA, from Duke University Medical Center (Durham, NC, USA, and colleagues assessed whether there was a link between patients undergoing cardiac stress imaging after coronary revascularization and the pattern of stress imaging billing of the physician practice providing their follow-up care. Using data from a US health insurance carrier, 17,847 patients were identified who between November 2004 and June 2007 had coronary revascularization and an index cardiac outpatient visit more than 90 days following the procedure. Based on overall billings, physicians were categorized into three classifications: physicians who routinely charged for technical and professional fees; physicians who regularly billed for professional fees only; and physicians who did not routinely bill for either service. Analytic models were used to evaluate the association between physician billing and use of stress testing, after adjusting for patient and other physician factors.
During the study period, the overall 30-day incidence of either nuclear stress testing or stress echocardiography testing associated with the index cardiac-related outpatient visit was 12.2%, with an overall incidence of 10.4% for nuclear stress testing and 1.8% for stress echocardiography. The incidence of nuclear stress testing among clinicians who billed for both technical and professional fees, professional-only fees, and neither fee for nuclear stress testing was 12.6%, 8.8%, and 5.0%, respectively. The stress echocardiography testing incidence among physicians who billed for both technical and professional fees, professional-only fees, and neither fee for stress echocardiography was 2.8%, 1.4%, and 0.4%, respectively.
Data analysis revealed that physicians who billed for technical and professional fees for nuclear stress testing and those who billed for professional fees only were more likely to perform nuclear stress tests following revascularization than those not billing (13.3% and 9.4% vs. 5.3%). Physicians who billed for technical and professional fees for stress echocardiography testing or professional fees only were more likely to perform stress echocardiography testing following revascularization than those not billing (3.1% and 1.5 percent vs. 0.5%).
The investigators reported that even though current ACCF AUC do not recommend regular use of early stress testing following coronary revascularization, they found that 12% of patients with a cardiac-related outpatient visit at least three months after revascularization underwent a stress test within 30 days of their visit. Moreover, up to one in 10 patients who were not classified as having symptoms at their outpatient visit still underwent stress testing.
“Our study highlights the need for application of the ACCF AUC in clinical practice and augments findings of other studies that have explicitly examined application of ACCF AUC for nuclear stress and stress echocardiography. The ACCF AUC provides guidance to clinicians regarding when to pursue cardiac stress testing to assist in narrowing variation in testing among clinicians and practices. Discretionary stress testing after revascularization has potential financial and clinical disadvantages for patients, including the costs of the tests, the exposure to ionizing radiation as well as potential down-stream costs, and consequences from following up false-positive test results,” the researchers concluded in their article. “These data suggest the need for broader application of AUC to minimize the possible influence of financial incentives on the decision to perform cardiac stress testing after revascularization.”
Related Links:
American College of Cardiology Foundation
Duke University Medical Center
Latest Ultrasound News
- Smart Ultrasound-Activated Immune Cells Destroy Cancer Cells for Extended Periods
- Tiny Magnetic Robot Takes 3D Scans from Deep Within Body
- High Resolution Ultrasound Speeds Up Prostate Cancer Diagnosis
- World's First Wireless, Handheld, Whole-Body Ultrasound with Single PZT Transducer Makes Imaging More Accessible
- Artificial Intelligence Detects Undiagnosed Liver Disease from Echocardiograms
- Ultrasound Imaging Non-Invasively Tracks Tumor Response to Radiation and Immunotherapy
- AI Improves Detection of Congenital Heart Defects on Routine Prenatal Ultrasounds
- AI Diagnoses Lung Diseases from Ultrasound Videos with 96.57% Accuracy
- New Contrast Agent for Ultrasound Imaging Ensures Affordable and Safer Medical Diagnostics
- Ultrasound-Directed Microbubbles Boost Immune Response Against Tumors
- POC Ultrasound Enhances Early Pregnancy Care and Cuts Emergency Visits
- AI-Based Models Outperform Human Experts at Identifying Ovarian Cancer in Ultrasound Images
- Automated Breast Ultrasound Provides Alternative to Mammography in Low-Resource Settings
- Transparent Ultrasound Transducer for Photoacoustic and Ultrasound Endoscopy to Improve Diagnostic Accuracy
- Wearable Ultrasound Patch Enables Continuous Blood Pressure Monitoring
- AI Image-Recognition Program Reads Echocardiograms Faster, Cuts Results Wait Time
Channels
Radiography
view channel
AI-Powered Imaging Technique Shows Promise in Evaluating Patients for PCI
Percutaneous coronary intervention (PCI), also known as coronary angioplasty, is a minimally invasive procedure where small metal tubes called stents are inserted into partially blocked coronary arteries... Read more
Higher Chest X-Ray Usage Catches Lung Cancer Earlier and Improves Survival
Lung cancer continues to be the leading cause of cancer-related deaths worldwide. While advanced technologies like CT scanners play a crucial role in detecting lung cancer, more accessible and affordable... Read moreMRI
view channel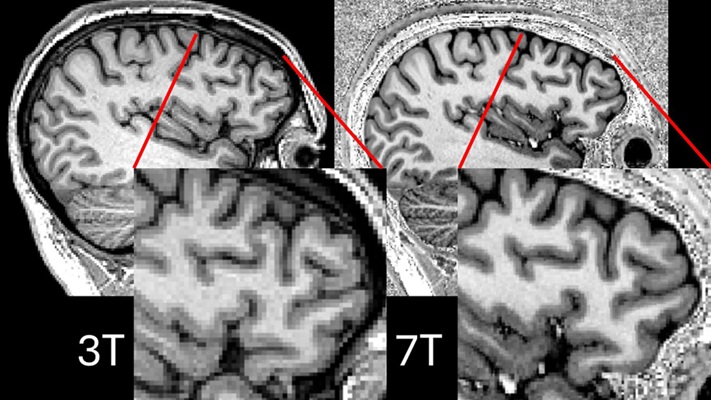
Ultra-Powerful MRI Scans Enable Life-Changing Surgery in Treatment-Resistant Epileptic Patients
Approximately 360,000 individuals in the UK suffer from focal epilepsy, a condition in which seizures spread from one part of the brain. Around a third of these patients experience persistent seizures... Read more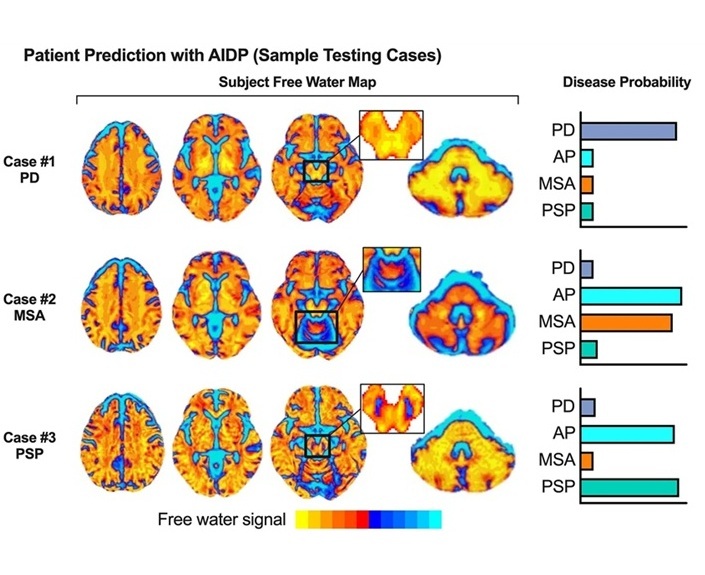
AI-Powered MRI Technology Improves Parkinson’s Diagnoses
Current research shows that the accuracy of diagnosing Parkinson’s disease typically ranges from 55% to 78% within the first five years of assessment. This is partly due to the similarities shared by Parkinson’s... Read more
Biparametric MRI Combined with AI Enhances Detection of Clinically Significant Prostate Cancer
Artificial intelligence (AI) technologies are transforming the way medical images are analyzed, offering unprecedented capabilities in quantitatively extracting features that go beyond traditional visual... Read more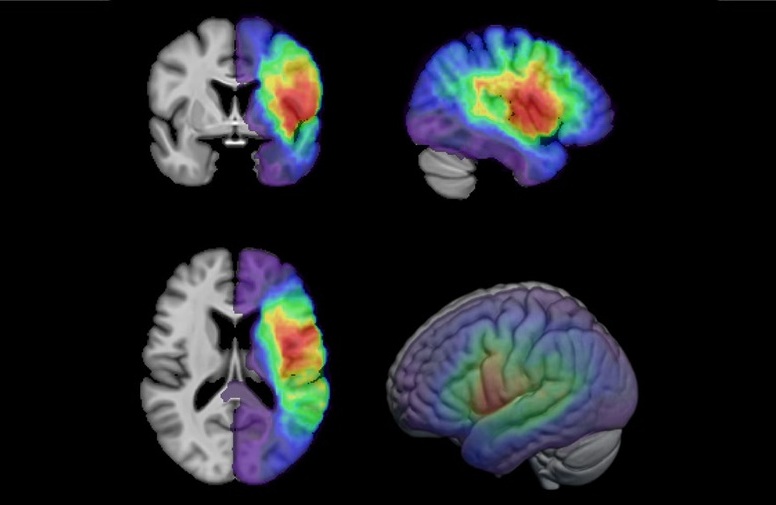
First-Of-Its-Kind AI-Driven Brain Imaging Platform to Better Guide Stroke Treatment Options
Each year, approximately 800,000 people in the U.S. experience strokes, with marginalized and minoritized groups being disproportionately affected. Strokes vary in terms of size and location within the... Read moreNuclear Medicine
view channel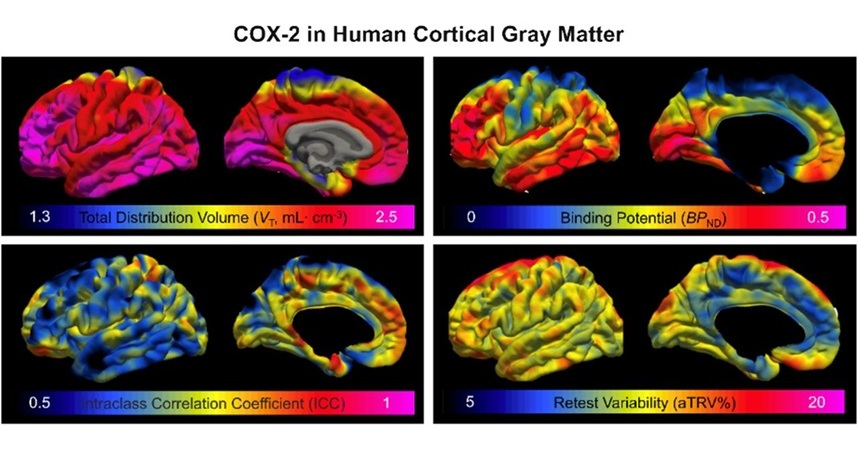
Novel PET Imaging Approach Offers Never-Before-Seen View of Neuroinflammation
COX-2, an enzyme that plays a key role in brain inflammation, can be significantly upregulated by inflammatory stimuli and neuroexcitation. Researchers suggest that COX-2 density in the brain could serve... Read more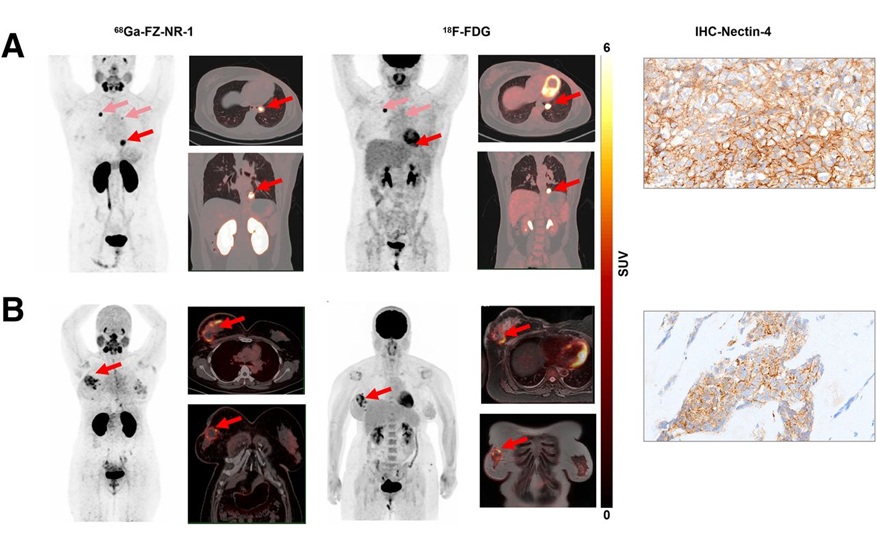
Novel Radiotracer Identifies Biomarker for Triple-Negative Breast Cancer
Triple-negative breast cancer (TNBC), which represents 15-20% of all breast cancer cases, is one of the most aggressive subtypes, with a five-year survival rate of about 40%. Due to its significant heterogeneity... Read moreGeneral/Advanced Imaging
view channel
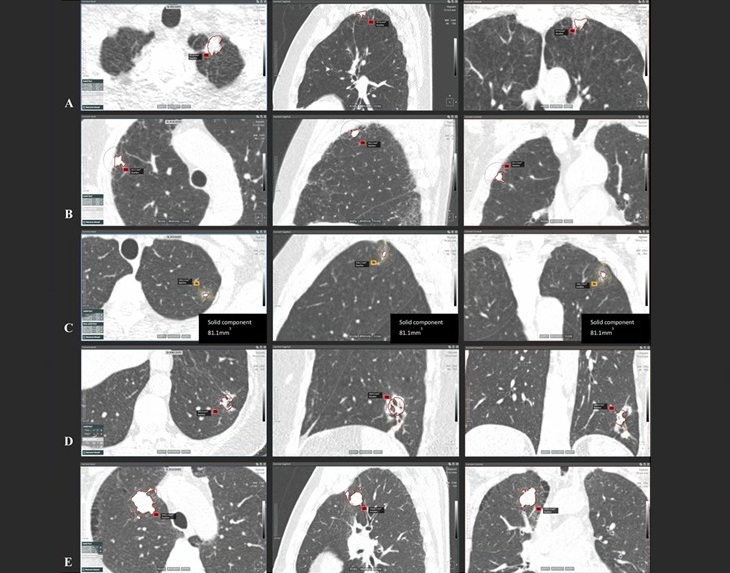
AI-Powered Imaging System Improves Lung Cancer Diagnosis
Given the need to detect lung cancer at earlier stages, there is an increasing need for a definitive diagnostic pathway for patients with suspicious pulmonary nodules. However, obtaining tissue samples... Read more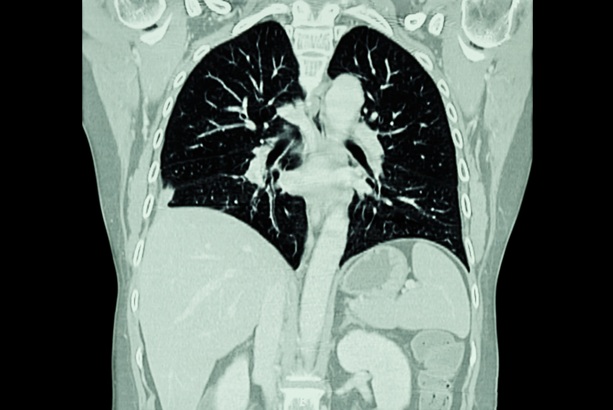
AI Model Significantly Enhances Low-Dose CT Capabilities
Lung cancer remains one of the most challenging diseases, making early diagnosis vital for effective treatment. Fortunately, advancements in artificial intelligence (AI) are revolutionizing lung cancer... Read moreImaging IT
view channel
New Google Cloud Medical Imaging Suite Makes Imaging Healthcare Data More Accessible
Medical imaging is a critical tool used to diagnose patients, and there are billions of medical images scanned globally each year. Imaging data accounts for about 90% of all healthcare data1 and, until... Read more
Global AI in Medical Diagnostics Market to Be Driven by Demand for Image Recognition in Radiology
The global artificial intelligence (AI) in medical diagnostics market is expanding with early disease detection being one of its key applications and image recognition becoming a compelling consumer proposition... Read moreIndustry News
view channel
GE HealthCare and NVIDIA Collaboration to Reimagine Diagnostic Imaging
GE HealthCare (Chicago, IL, USA) has entered into a collaboration with NVIDIA (Santa Clara, CA, USA), expanding the existing relationship between the two companies to focus on pioneering innovation in... Read more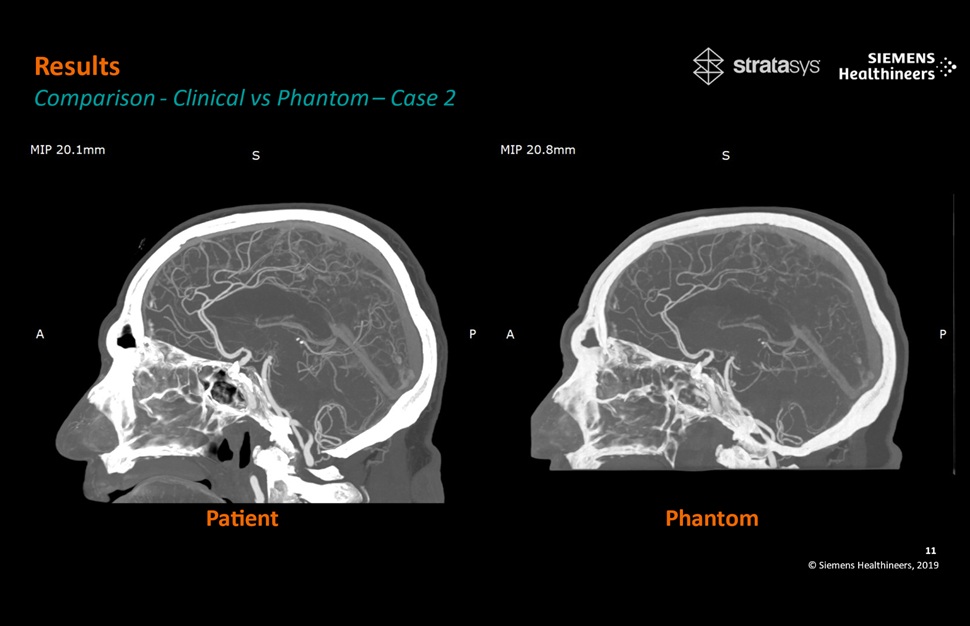
Patient-Specific 3D-Printed Phantoms Transform CT Imaging
New research has highlighted how anatomically precise, patient-specific 3D-printed phantoms are proving to be scalable, cost-effective, and efficient tools in the development of new CT scan algorithms... Read more
Siemens and Sectra Collaborate on Enhancing Radiology Workflows
Siemens Healthineers (Forchheim, Germany) and Sectra (Linköping, Sweden) have entered into a collaboration aimed at enhancing radiologists' diagnostic capabilities and, in turn, improving patient care... Read more