Post-Surgical X-Rays Predict Bunion Recurrence Risk
|
By MedImaging International staff writers Posted on 10 Aug 2017 |
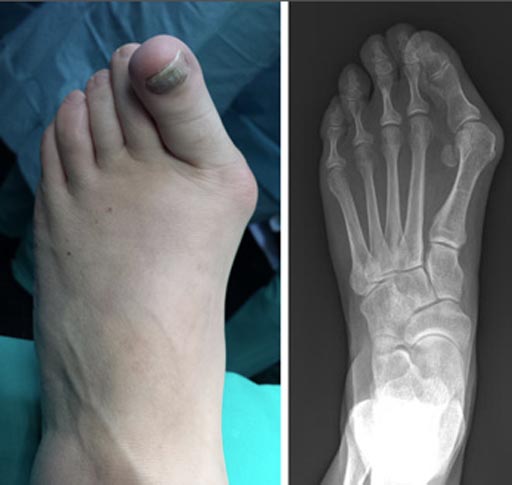
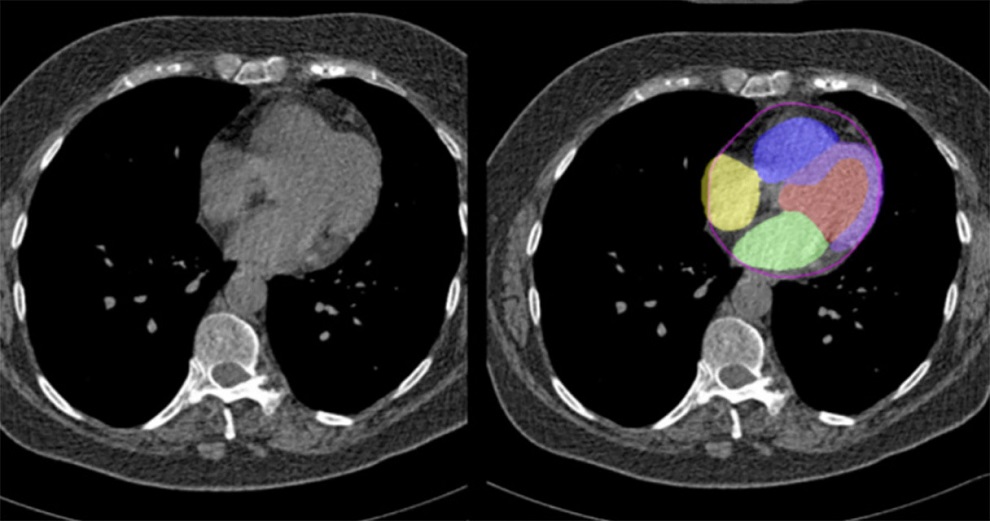
Image: The clinical and radiographic appearance of a bunion (Photo courtesy of AAOS).
Measuring the hallux valgus angle (HVA) on postoperative x-rays immediately following bunion surgery can reliably predict satisfactory correction and risk of recurrence.
Researchers at Yeungnam University (Daegu, South Korea) and Injie University Seoul Paik Hospital (Republic of Korea) conducted a study in 93 patients (for a total of 117 feet) who underwent proximal chevron osteotomy combined with a distal soft-tissue procedure in order to treat moderate to severe hallux valgus deformity. Changes in hallux valgus angle, inter-metatarsal angle, and sesamoid position over time were analyzed by comparing non-weight-bearing radiographs during each postoperative period.
The relative risks of recurrence, as indicated by preoperative and postoperative radiographic parameters were then determined. The results showed that hallux valgus angle and inter-metatarsal angle stabilized at six months after surgery in the nonrecurrence group. Hallux valgus recurrence was associated with an immediate postoperative hallux valgus angle higher than 8°, immediate postoperative sesamoid position of grade 4 or greater, a preoperative metatarsus adductus angle of 23° or higher, and a preoperative hallux valgus angle of higher than 40°. The study was published in the July 2017 issue of The Journal of Bone and Joint Surgery.
“Bunions were 28 times more likely to recur when the postoperative HVA was eight degrees or larger than when the HVA was less than eight degrees. The HVA continued to widen over time in patients with recurrent bunions, but stabilized at six months in those without recurrence,” concluded study authors Chul Hyun Park, MD, PhD, and Woo-Chun Lee, MD, PhD. “The recurrence of hallux valgus is one of the most important complications after surgery because it is closely related to patient satisfaction.”
A bunion is a painful bony bump that develops when the metatarsophalangeal (MTP) joints move out of alignment: the long metatarsal bone shifts toward the inside of the foot, and the phalanx bones of the big toe angle toward the second toe. The MTP joint gets larger and protrudes from the inside of the forefoot. The enlarged joint is often inflamed, red, and swollen. The word bunion, in fact, comes from the Greek word for turnip, hinting to its appearance.
Related Links:
Yeungnam University
Injie University Seoul Paik Hospital
Researchers at Yeungnam University (Daegu, South Korea) and Injie University Seoul Paik Hospital (Republic of Korea) conducted a study in 93 patients (for a total of 117 feet) who underwent proximal chevron osteotomy combined with a distal soft-tissue procedure in order to treat moderate to severe hallux valgus deformity. Changes in hallux valgus angle, inter-metatarsal angle, and sesamoid position over time were analyzed by comparing non-weight-bearing radiographs during each postoperative period.
The relative risks of recurrence, as indicated by preoperative and postoperative radiographic parameters were then determined. The results showed that hallux valgus angle and inter-metatarsal angle stabilized at six months after surgery in the nonrecurrence group. Hallux valgus recurrence was associated with an immediate postoperative hallux valgus angle higher than 8°, immediate postoperative sesamoid position of grade 4 or greater, a preoperative metatarsus adductus angle of 23° or higher, and a preoperative hallux valgus angle of higher than 40°. The study was published in the July 2017 issue of The Journal of Bone and Joint Surgery.
“Bunions were 28 times more likely to recur when the postoperative HVA was eight degrees or larger than when the HVA was less than eight degrees. The HVA continued to widen over time in patients with recurrent bunions, but stabilized at six months in those without recurrence,” concluded study authors Chul Hyun Park, MD, PhD, and Woo-Chun Lee, MD, PhD. “The recurrence of hallux valgus is one of the most important complications after surgery because it is closely related to patient satisfaction.”
A bunion is a painful bony bump that develops when the metatarsophalangeal (MTP) joints move out of alignment: the long metatarsal bone shifts toward the inside of the foot, and the phalanx bones of the big toe angle toward the second toe. The MTP joint gets larger and protrudes from the inside of the forefoot. The enlarged joint is often inflamed, red, and swollen. The word bunion, in fact, comes from the Greek word for turnip, hinting to its appearance.
Related Links:
Yeungnam University
Injie University Seoul Paik Hospital
Latest Radiography News
- Novel Breast Imaging System Proves As Effective As Mammography
- AI Assistance Improves Breast-Cancer Screening by Reducing False Positives
- AI Could Boost Clinical Adoption of Chest DDR
- 3D Mammography Almost Halves Breast Cancer Incidence between Two Screening Tests
- AI Model Predicts 5-Year Breast Cancer Risk from Mammograms
- Deep Learning Framework Detects Fractures in X-Ray Images With 99% Accuracy
- Direct AI-Based Medical X-Ray Imaging System a Paradigm-Shift from Conventional DR and CT
- Chest X-Ray AI Solution Automatically Identifies, Categorizes and Highlights Suspicious Areas
- AI Diagnoses Wrist Fractures As Well As Radiologists
- Annual Mammography Beginning At 40 Cuts Breast Cancer Mortality By 42%
- 3D Human GPS Powered By Light Paves Way for Radiation-Free Minimally-Invasive Surgery
- Novel AI Technology to Revolutionize Cancer Detection in Dense Breasts
- AI Solution Provides Radiologists with 'Second Pair' Of Eyes to Detect Breast Cancers
- AI Helps General Radiologists Achieve Specialist-Level Performance in Interpreting Mammograms
- Novel Imaging Technique Could Transform Breast Cancer Detection
- Computer Program Combines AI and Heat-Imaging Technology for Early Breast Cancer Detection
Channels
MRI
view channel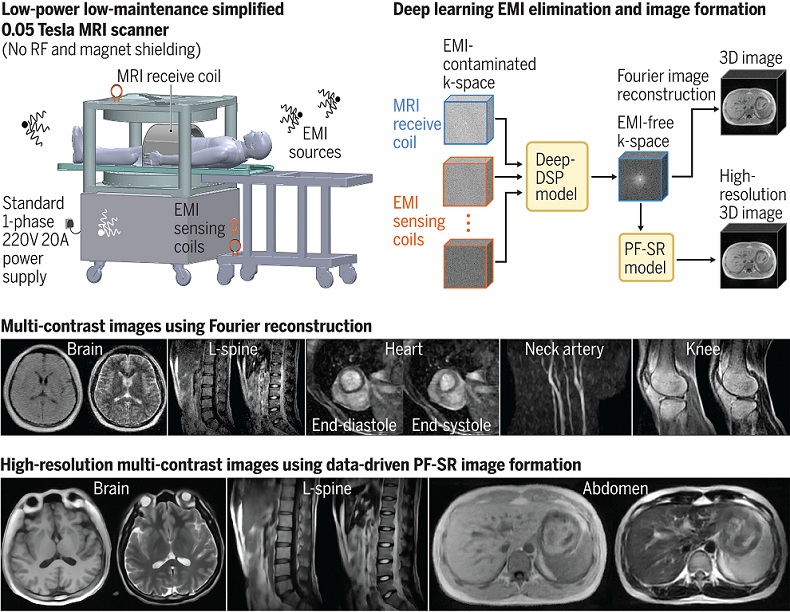
Low-Cost Whole-Body MRI Device Combined with AI Generates High-Quality Results
Magnetic Resonance Imaging (MRI) has significantly transformed healthcare, providing a noninvasive, radiation-free method for detailed imaging. It is especially promising for the future of medical diagnosis... Read more
World's First Whole-Body Ultra-High Field MRI Officially Comes To Market
The world's first whole-body ultra-high field (UHF) MRI has officially come to market, marking a remarkable advancement in diagnostic radiology. United Imaging (Shanghai, China) has secured clearance from the U.... Read moreUltrasound
view channel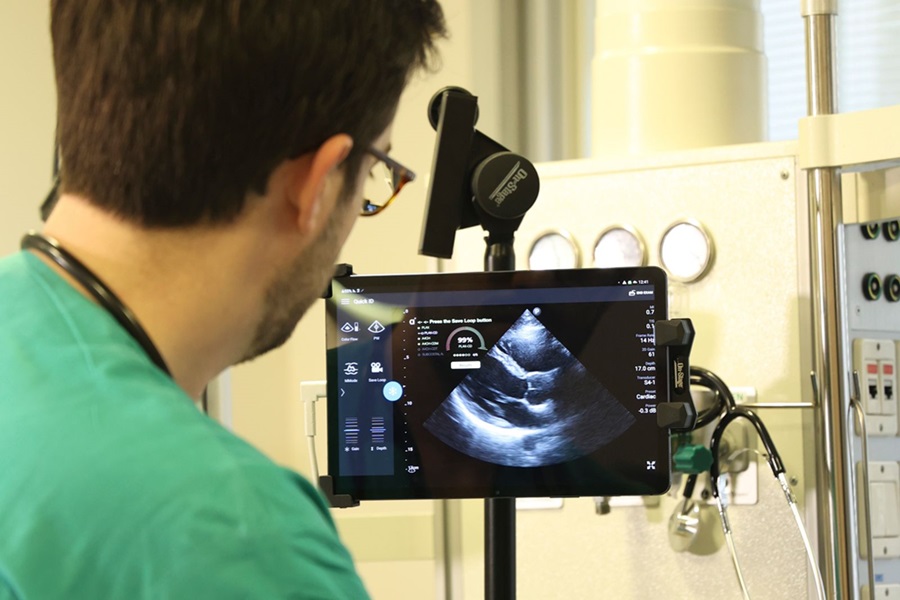
First AI-Powered POC Ultrasound Diagnostic Solution Helps Prioritize Cases Based On Severity
Ultrasound scans are essential for identifying and diagnosing various medical conditions, but often, patients must wait weeks or months for results due to a shortage of qualified medical professionals... Read more
Largest Model Trained On Echocardiography Images Assesses Heart Structure and Function
Foundation models represent an exciting frontier in generative artificial intelligence (AI), yet many lack the specialized medical data needed to make them applicable in healthcare settings.... Read more.jpg)
Groundbreaking Technology Enables Precise, Automatic Measurement of Peripheral Blood Vessels
The current standard of care of using angiographic information is often inadequate for accurately assessing vessel size in the estimated 20 million people in the U.S. who suffer from peripheral vascular disease.... Read moreNuclear Medicine
view channelNew PET Agent Rapidly and Accurately Visualizes Lesions in Clear Cell Renal Cell Carcinoma Patients
Clear cell renal cell cancer (ccRCC) represents 70-80% of renal cell carcinoma cases. While localized disease can be effectively treated with surgery and ablative therapies, one-third of patients either... Read more
New Imaging Technique Monitors Inflammation Disorders without Radiation Exposure
Imaging inflammation using traditional radiological techniques presents significant challenges, including radiation exposure, poor image quality, high costs, and invasive procedures. Now, new contrast... Read more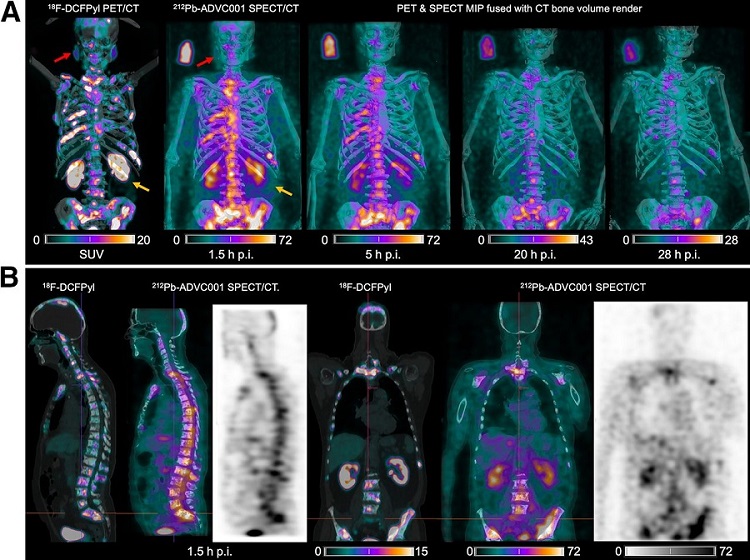
New SPECT/CT Technique Could Change Imaging Practices and Increase Patient Access
The development of lead-212 (212Pb)-PSMA–based targeted alpha therapy (TAT) is garnering significant interest in treating patients with metastatic castration-resistant prostate cancer. The imaging of 212Pb,... Read moreGeneral/Advanced Imaging
view channel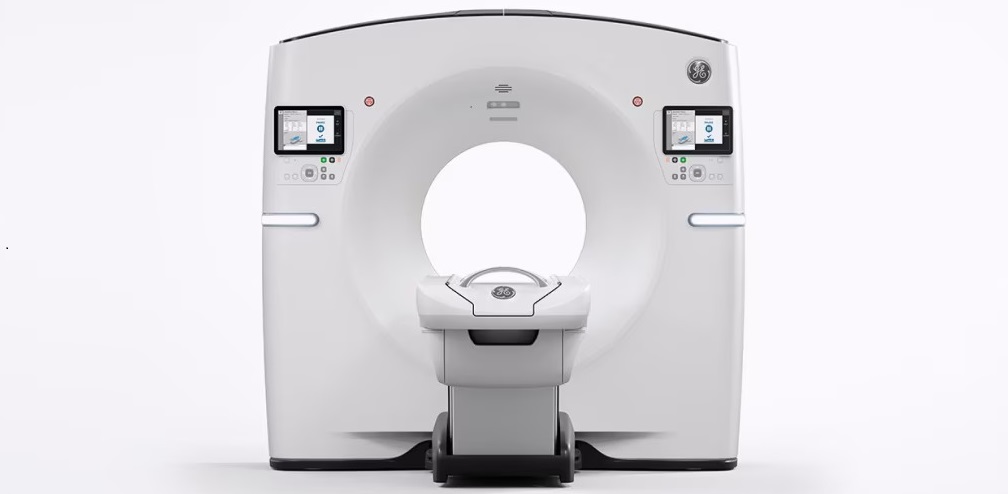
Radiation Therapy Computed Tomography Solution Boosts Imaging Accuracy
One of the most significant challenges in oncology care is disease complexity in terms of the variety of cancer types and the individualized presentation of each patient. This complexity necessitates a... Read more
PET Scans Reveal Hidden Inflammation in Multiple Sclerosis Patients
A key challenge for clinicians treating patients with multiple sclerosis (MS) is that after a certain amount of time, they continue to worsen even though their MRIs show no change. A new study has now... Read moreImaging IT
view channel
New Google Cloud Medical Imaging Suite Makes Imaging Healthcare Data More Accessible
Medical imaging is a critical tool used to diagnose patients, and there are billions of medical images scanned globally each year. Imaging data accounts for about 90% of all healthcare data1 and, until... Read more
Global AI in Medical Diagnostics Market to Be Driven by Demand for Image Recognition in Radiology
The global artificial intelligence (AI) in medical diagnostics market is expanding with early disease detection being one of its key applications and image recognition becoming a compelling consumer proposition... Read moreIndustry News
view channel
Hologic Acquires UK-Based Breast Surgical Guidance Company Endomagnetics Ltd.
Hologic, Inc. (Marlborough, MA, USA) has entered into a definitive agreement to acquire Endomagnetics Ltd. (Cambridge, UK), a privately held developer of breast cancer surgery technologies, for approximately... Read more
Bayer and Google Partner on New AI Product for Radiologists
Medical imaging data comprises around 90% of all healthcare data, and it is a highly complex and rich clinical data modality and serves as a vital tool for diagnosing patients. Each year, billions of medical... Read more