RT Offers Hope for High-Risk Arrhythmia Patients
|
By MedImaging International staff writers Posted on 09 Oct 2019 |
Image: According to a new study, RT can offer hope the VT patients who have exhausted other options (Photo courtesy of SPL).
A single, high dose of radiation therapy (RT) can dramatically reduce episodes of ventricular tachycardia (VT) for more than two years, according to a new study.
Developed at the Washington University (WUSTL; St. Louis, MO, USA) School of Medicine, the noninvasive, outpatient procedure for treating VT is called EP-guided noninvasive cardiac radioablation (ENCORE). The novel therapy fuses electrocardiogram (ECG) and imaging data to pinpoint the scar tissue in the patient's heart responsible for the arrhythmias, and then targets it with a single dose of stereotactic body radiation therapy (SBRT). ENCORE requires no general anesthesia, and allows patients to go home immediately after treatment.
In a phase I/II prospective trial, 19 patients who had life-threatening VT were treated with a single fraction (25 Gy) of SBRT. ENCORE led to a 94% reduction in VT episodes in the first six months after SBRT, with longer-term follow-up data showing that the effect persisted in 78% of patients for more than two years; overall survival was 52% after the second year. Of the nine patients who died, six suffered from cardiac deaths (heart failure and VT recurrence) and three from non-cardiac deaths (accident, amiodarone toxicity, and pancreatic cancer). The study was presented at the 61st annual meeting of the American Society for Radiation Oncology (ASTRO), held during September 2019 in Chicago (IL, USA).
“Patients come to us as a last line of defense. They have few or no other options. Often, the primary reason we are treating them is because they were too sick to have more catheter ablation,” said lead author and study presenter Clifford Robinson, MD, an associate professor of radiation oncology and cardiology at WUSTL. “Given the relative novelty of this treatment approach, we are following our patients closely, conducting trials to gather more data and being careful not to make assumptions at this point.”
“An additional benefit to treatment was a reduction in the medications patients were taking, which resulted in fewer medication-related side effects and a higher quality of life,” concluded Dr. Robinson. “These patients were on heavy doses of medications, with side effects such as liver damage, lung damage, nausea, and thyroid problems. After they were treated, we could dramatically reduce their medications. We saw reduced VT, reduced medication and improved quality of life, at least in the intermediate term.”
In VT, the electrical signals in the heart’s lower chambers misfire, crippling the relaxation and refilling process and producing rapid arrhythmias. First line treatment for VT includes pharmaceuticals and an implantable cardioverter defibrillator (ICD). Patients with recurrent VT often also undergo catheter ablation, which requires general anesthesia, takes up to nine hours to perform, holds a 5% mortality risk, and has a 50% chance that it won't stop VT arrhythmias from recurring. If catheter ablation does not control the VT, patients are left with few options beyond a heart transplant.
Related Links:
Washington University
Developed at the Washington University (WUSTL; St. Louis, MO, USA) School of Medicine, the noninvasive, outpatient procedure for treating VT is called EP-guided noninvasive cardiac radioablation (ENCORE). The novel therapy fuses electrocardiogram (ECG) and imaging data to pinpoint the scar tissue in the patient's heart responsible for the arrhythmias, and then targets it with a single dose of stereotactic body radiation therapy (SBRT). ENCORE requires no general anesthesia, and allows patients to go home immediately after treatment.
In a phase I/II prospective trial, 19 patients who had life-threatening VT were treated with a single fraction (25 Gy) of SBRT. ENCORE led to a 94% reduction in VT episodes in the first six months after SBRT, with longer-term follow-up data showing that the effect persisted in 78% of patients for more than two years; overall survival was 52% after the second year. Of the nine patients who died, six suffered from cardiac deaths (heart failure and VT recurrence) and three from non-cardiac deaths (accident, amiodarone toxicity, and pancreatic cancer). The study was presented at the 61st annual meeting of the American Society for Radiation Oncology (ASTRO), held during September 2019 in Chicago (IL, USA).
“Patients come to us as a last line of defense. They have few or no other options. Often, the primary reason we are treating them is because they were too sick to have more catheter ablation,” said lead author and study presenter Clifford Robinson, MD, an associate professor of radiation oncology and cardiology at WUSTL. “Given the relative novelty of this treatment approach, we are following our patients closely, conducting trials to gather more data and being careful not to make assumptions at this point.”
“An additional benefit to treatment was a reduction in the medications patients were taking, which resulted in fewer medication-related side effects and a higher quality of life,” concluded Dr. Robinson. “These patients were on heavy doses of medications, with side effects such as liver damage, lung damage, nausea, and thyroid problems. After they were treated, we could dramatically reduce their medications. We saw reduced VT, reduced medication and improved quality of life, at least in the intermediate term.”
In VT, the electrical signals in the heart’s lower chambers misfire, crippling the relaxation and refilling process and producing rapid arrhythmias. First line treatment for VT includes pharmaceuticals and an implantable cardioverter defibrillator (ICD). Patients with recurrent VT often also undergo catheter ablation, which requires general anesthesia, takes up to nine hours to perform, holds a 5% mortality risk, and has a 50% chance that it won't stop VT arrhythmias from recurring. If catheter ablation does not control the VT, patients are left with few options beyond a heart transplant.
Related Links:
Washington University
Latest Nuclear Medicine News
- New Imaging Tool Sheds Light on Tumor Fat Metabolism
- PET Tracer Enables Noninvasive Measurement of Beta Cell Mass
- Radiopharmaceutical Molecule Marker to Improve Choice of Bladder Cancer Therapies
- Cancer “Flashlight” Shows Who Can Benefit from Targeted Treatments
- PET Imaging of Inflammation Predicts Recovery and Guides Therapy After Heart Attack
- Radiotheranostic Approach Detects, Kills and Reprograms Aggressive Cancers
- New Imaging Solution Improves Survival for Patients with Recurring Prostate Cancer
- PET Tracer Enables Same-Day Imaging of Triple-Negative Breast and Urothelial Cancers
- New Camera Sees Inside Human Body for Enhanced Scanning and Diagnosis
- Novel Bacteria-Specific PET Imaging Approach Detects Hard-To-Diagnose Lung Infections
- New Imaging Approach Could Reduce Need for Biopsies to Monitor Prostate Cancer
- Novel Radiolabeled Antibody Improves Diagnosis and Treatment of Solid Tumors
- Novel PET Imaging Approach Offers Never-Before-Seen View of Neuroinflammation
- Novel Radiotracer Identifies Biomarker for Triple-Negative Breast Cancer
- Innovative PET Imaging Technique to Help Diagnose Neurodegeneration
- New Molecular Imaging Test to Improve Lung Cancer Diagnosis
Channels
Radiography
view channel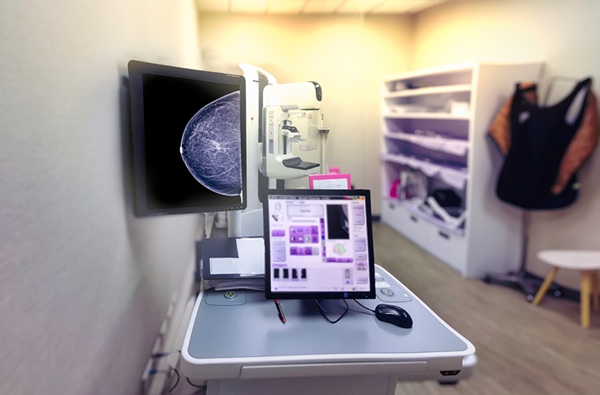
AI Boosts Breast Cancer Detection and Cuts Screening Workload
Breast cancer screening programs face rising demand and persistent workforce shortages, straining double-reading workflows and delaying care. Early detection is critical to reduce mortality and minimize... Read more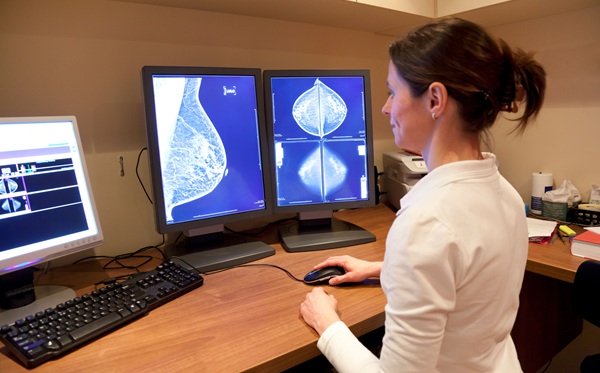
AI Tool Predicts Breast Cancer Risk Years Ahead Using Routine Mammograms
Breast cancer screening saves lives but still relies largely on uniform schedules despite wide differences in individual risk. This one-size-fits-all approach can miss cancers in higher-risk women while... Read moreMRI
view channel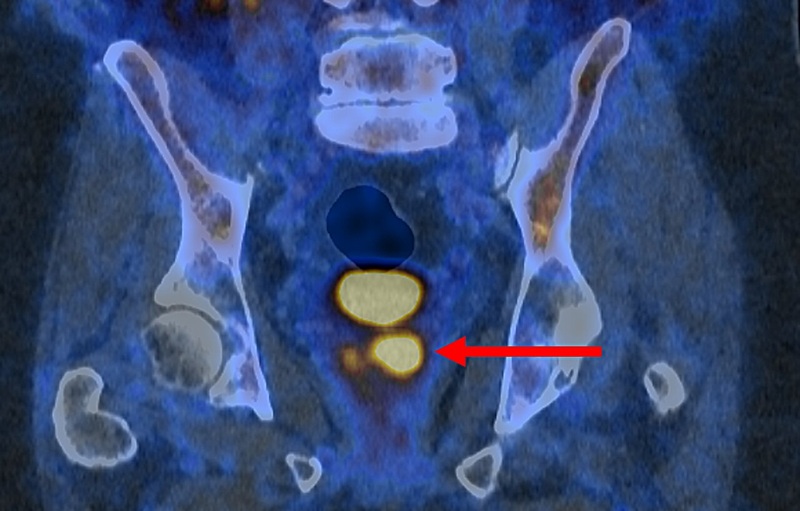
Study Finds Advanced Imaging Significantly Reduces Unnecessary Prostate Biopsies
Many men with suspected prostate cancer face an invasive biopsy when magnetic resonance imaging (MRI) is inconclusive. Biopsies can be uncomfortable, carry risks, and may contribute to overdiagnosis and... Read more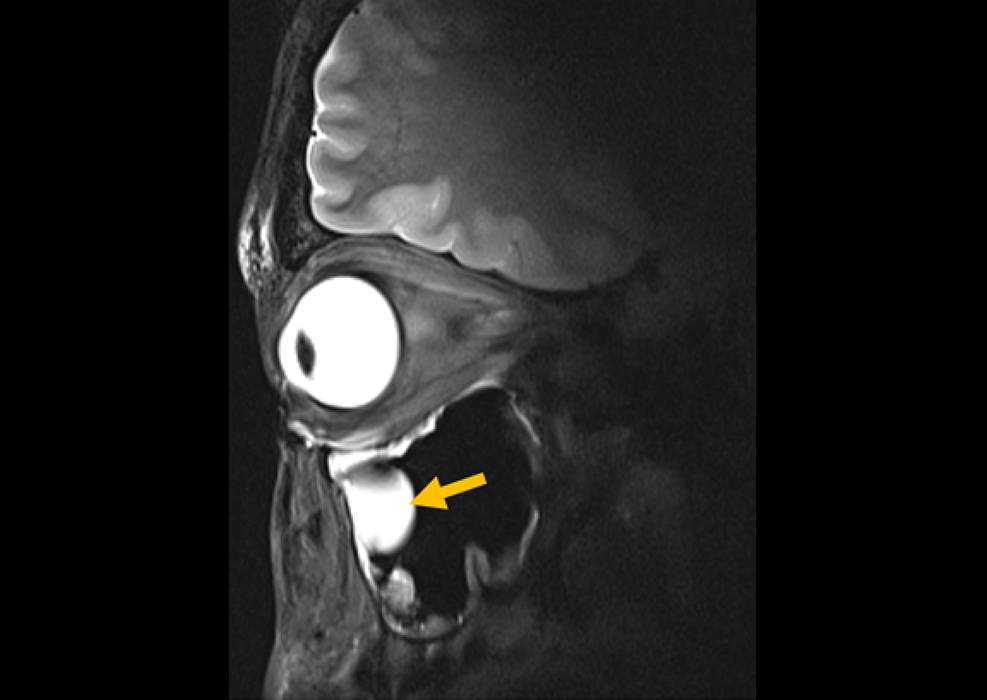
New Material Boosts MRI Image Quality
Magnetic resonance imaging (MRI) is a cornerstone of modern diagnostics, yet certain deep or anatomically complex tissues, including delicate structures of the eye and orbit, remain difficult to visualize clearly.... Read moreUltrasound
view channel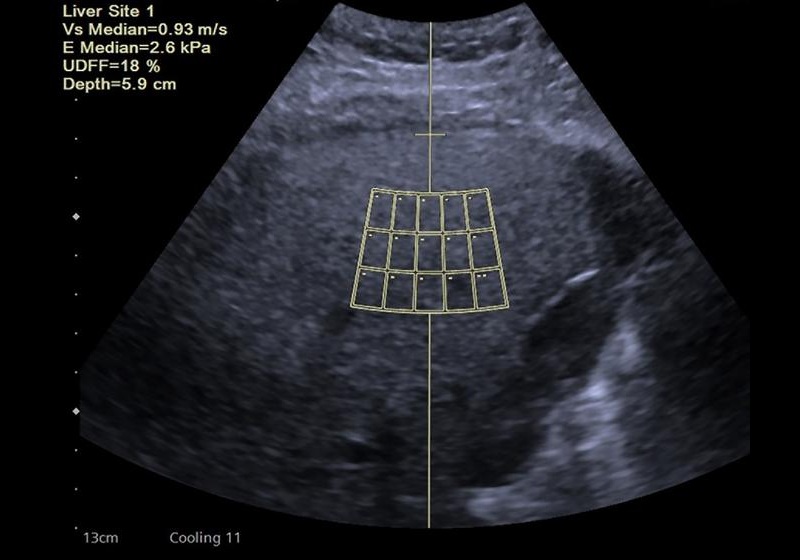
New Consensus Standardizes Ultrasound-Based Fatty Liver Assessment
Metabolic dysfunction-associated steatotic liver disease (MASLD) is rising along with obesity and diabetes, making accurate, scalable measurement of hepatic fat a clinical priority. Biopsy is invasive... Read more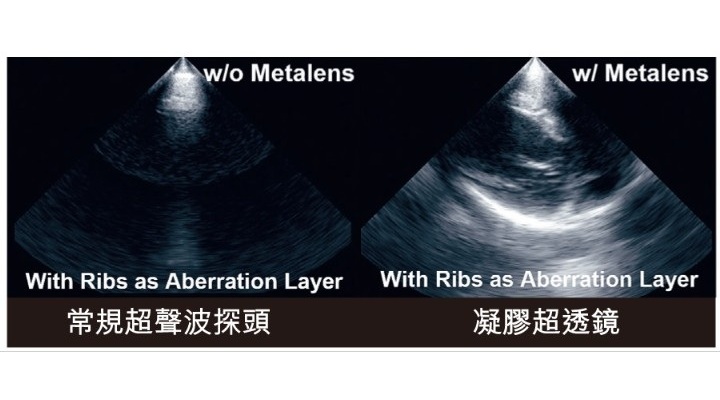
Groundbreaking Technology to Enhance Precision in Emergency and Critical Care
Rapid and accurate imaging is essential for diagnosing life-threatening conditions such as myocardial infarction, heart failure, and pulmonary embolism. However, conventional ultrasound imaging of the... Read moreGeneral/Advanced Imaging
view channel
AI Tool Predicts Side Effects from Lung Cancer Treatment
Radiation therapy is a central treatment for lung cancer, but even carefully targeted radiation can affect surrounding healthy tissue. Patients may develop side effects such as lung inflammation, coughing,... Read more
AI Tool Offers Prognosis for Patients with Head and Neck Cancer
Oropharyngeal cancer is a form of head and neck cancer that can spread through lymph nodes, significantly affecting survival and treatment decisions. Current therapies often involve combinations of surgery,... Read moreImaging IT
view channel
New Google Cloud Medical Imaging Suite Makes Imaging Healthcare Data More Accessible
Medical imaging is a critical tool used to diagnose patients, and there are billions of medical images scanned globally each year. Imaging data accounts for about 90% of all healthcare data1 and, until... Read more
Global AI in Medical Diagnostics Market to Be Driven by Demand for Image Recognition in Radiology
The global artificial intelligence (AI) in medical diagnostics market is expanding with early disease detection being one of its key applications and image recognition becoming a compelling consumer proposition... Read moreIndustry News
view channel
Nuclear Medicine Set for Continued Growth Driven by Demand for Precision Diagnostics
Clinical imaging services face rising demand for precise molecular diagnostics and targeted radiopharmaceutical therapy as cancer and chronic disease rates climb. A new market analysis projects rapid expansion... Read more