Artificial Intelligence Accurately Predicts Radiation Treatment Side Effects
|
By MedImaging International staff writers Posted on 01 Oct 2019 |

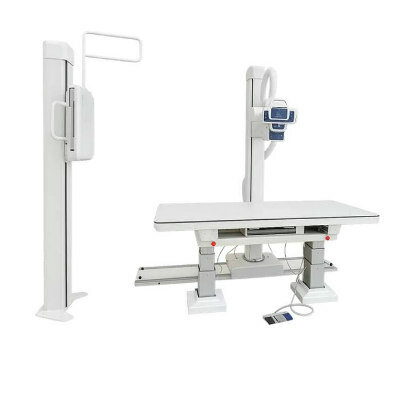
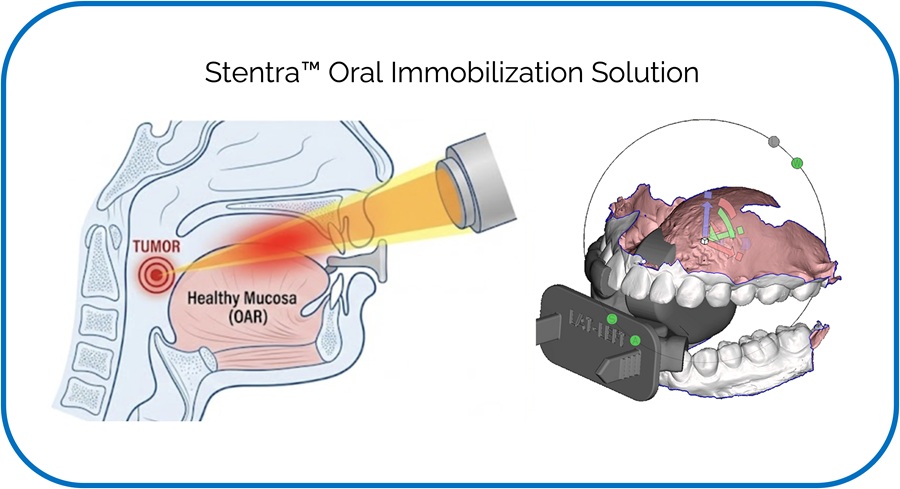
Image: New research has shown that a computer model can predict side effects associated with radiation therapy (Photo courtesy of Technology Networks).
Researchers from the University of Texas MD Anderson Cancer Center (Houston, Texas, USA) have demonstrated that a sophisticated computer model can accurately predict two of the most challenging side effects associated with radiation therapy for head and neck cancer. This precision oncology approach has the potential to better identify patients who might benefit from early interventions that could help prevent significant weight loss after treatment or reduce the need for feeding tube placement.
The team of researchers developed models to analyze large sets of data merged from three sources: electronic health records (Epic), an internal web-based charting tool (Brocade) and the record/verify system (Mosaiq). The data included more than 700 clinical and treatment variables for patients with head and neck cancer (75% male/25% female, with a median age of 62 years) who received more than 2,000 courses of radiation therapy (median dose 60 Gy) across five practice sites at MD Anderson from 2016 to 2018.
The researchers used the models to predict three endpoints: significant weight loss, feeding tube placement and unplanned hospitalizations. Results from the best-performing model were then validated against 225 subsequent consecutive radiation therapy treatments. Models with a performance rate that met a pre-specified threshold of area under the curve (AUC) of 0.70 or higher were considered clinically valid (an AUC score of 1.0 would mean the model’s predictions were 100% accurate, while a score of 0.0 would mean the predictions were never accurate). The models predicted the likelihood of significant weight loss (AUC = 0.751) and need for feeding tube placement (AUC = 0.755) with a high degree of accuracy.
“Being able to identify which patients are at greatest risk would allow radiation oncologists to take steps to prevent or mitigate these possible side effects,” said Jay Reddy, MD, PhD, an assistant professor of radiation oncology at The University of Texas MD Anderson Cancer Center and lead author on the study. “If the patient has an intermediate risk, and they might get through treatment without needing a feeding tube, we could take precautions such as setting them up with a nutritionist and providing them with nutritional supplements. If we know their risk for feeding tube placement is extremely high – a better than 50% chance they would need one – we could place it ahead of time so they wouldn’t have to be admitted to the hospital after treatment. We’d know to keep a closer eye on that patient.”
The machine learning approach cannot isolate the single-most predictive factor or combination of factors that lead to negative side effects, but can provide patients and their clinicians with a better understanding of what to expect during the course of treatment. In addition to predicting the likelihood of side effects, machine learning models could potentially predict which treatment plans would be most effective for different types of patients and allow for more personalized approaches to radiation oncology.
“Machine learning can make doctors more efficient and treatment safer by reducing the risk of error,” added Dr. Reddy. “It has the potential for influencing all aspects of radiation oncology today – anything where a computer can look at data and recognize a pattern.”
Related Links:
University of Texas MD Anderson Cancer Center
The team of researchers developed models to analyze large sets of data merged from three sources: electronic health records (Epic), an internal web-based charting tool (Brocade) and the record/verify system (Mosaiq). The data included more than 700 clinical and treatment variables for patients with head and neck cancer (75% male/25% female, with a median age of 62 years) who received more than 2,000 courses of radiation therapy (median dose 60 Gy) across five practice sites at MD Anderson from 2016 to 2018.
The researchers used the models to predict three endpoints: significant weight loss, feeding tube placement and unplanned hospitalizations. Results from the best-performing model were then validated against 225 subsequent consecutive radiation therapy treatments. Models with a performance rate that met a pre-specified threshold of area under the curve (AUC) of 0.70 or higher were considered clinically valid (an AUC score of 1.0 would mean the model’s predictions were 100% accurate, while a score of 0.0 would mean the predictions were never accurate). The models predicted the likelihood of significant weight loss (AUC = 0.751) and need for feeding tube placement (AUC = 0.755) with a high degree of accuracy.
“Being able to identify which patients are at greatest risk would allow radiation oncologists to take steps to prevent or mitigate these possible side effects,” said Jay Reddy, MD, PhD, an assistant professor of radiation oncology at The University of Texas MD Anderson Cancer Center and lead author on the study. “If the patient has an intermediate risk, and they might get through treatment without needing a feeding tube, we could take precautions such as setting them up with a nutritionist and providing them with nutritional supplements. If we know their risk for feeding tube placement is extremely high – a better than 50% chance they would need one – we could place it ahead of time so they wouldn’t have to be admitted to the hospital after treatment. We’d know to keep a closer eye on that patient.”
The machine learning approach cannot isolate the single-most predictive factor or combination of factors that lead to negative side effects, but can provide patients and their clinicians with a better understanding of what to expect during the course of treatment. In addition to predicting the likelihood of side effects, machine learning models could potentially predict which treatment plans would be most effective for different types of patients and allow for more personalized approaches to radiation oncology.
“Machine learning can make doctors more efficient and treatment safer by reducing the risk of error,” added Dr. Reddy. “It has the potential for influencing all aspects of radiation oncology today – anything where a computer can look at data and recognize a pattern.”
Related Links:
University of Texas MD Anderson Cancer Center
Latest Industry News News
- GE HealthCare Highlights AI-Supported Radiation Therapy Tools at ESTRO 2026
- Nuclear Medicine Set for Continued Growth Driven by Demand for Precision Diagnostics
- GE HealthCare and NVIDIA Collaboration to Reimagine Diagnostic Imaging
- Patient-Specific 3D-Printed Phantoms Transform CT Imaging
- Siemens and Sectra Collaborate on Enhancing Radiology Workflows
- Bracco Diagnostics and ColoWatch Partner to Expand Availability CRC Screening Tests Using Virtual Colonoscopy
- Mindray Partners with TeleRay to Streamline Ultrasound Delivery
- Philips and Medtronic Partner on Stroke Care
- Siemens and Medtronic Enter into Global Partnership for Advancing Spine Care Imaging Technologies
- RSNA 2024 Technical Exhibits to Showcase Latest Advances in Radiology
- Bracco Collaborates with Arrayus on Microbubble-Assisted Focused Ultrasound Therapy for Pancreatic Cancer
- Innovative Collaboration to Enhance Ischemic Stroke Detection and Elevate Standards in Diagnostic Imaging
- RSNA 2024 Registration Opens
- Microsoft collaborates with Leading Academic Medical Systems to Advance AI in Medical Imaging
- GE HealthCare Acquires Intelligent Ultrasound Group’s Clinical Artificial Intelligence Business
- Bayer and Rad AI Collaborate on Expanding Use of Cutting Edge AI Radiology Operational Solutions
Channels
Radiography
view channel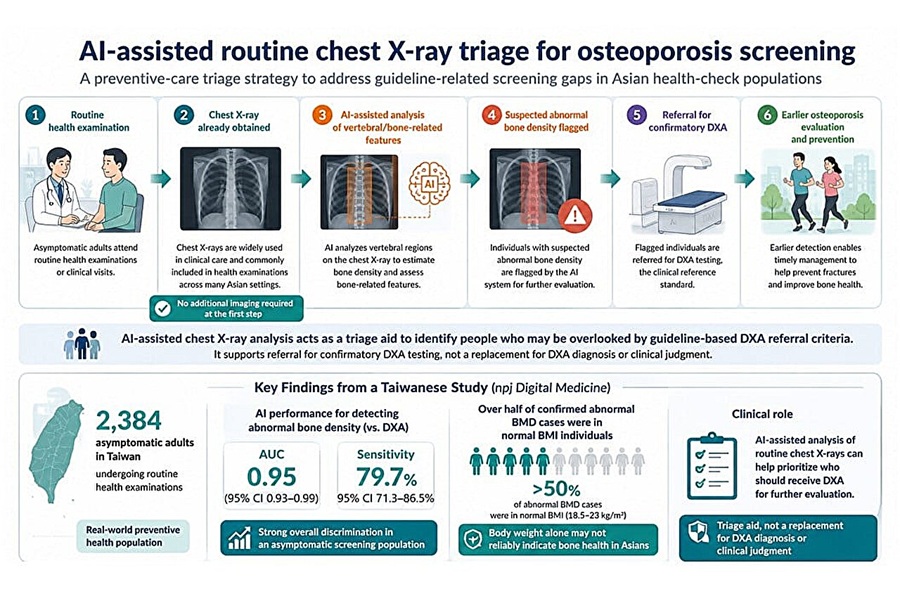
AI Tool Flags Osteoporosis Risk from Routine Chest X-Rays
Osteoporosis is a progressive loss of bone density that is often silent until a fracture occurs. Current screening frameworks concentrate on older women and select high-risk groups. Many men, younger adults,... Read more
Simple Chest X-Ray Measure Predicts Survival After Lung Cancer Surgery
Obstructive ventilatory disorder, marked by airflow limitation that reduces breathing efficiency, increases postoperative risk in patients with lung cancer. Although surgery offers the best chance of cure,... Read moreMRI
view channel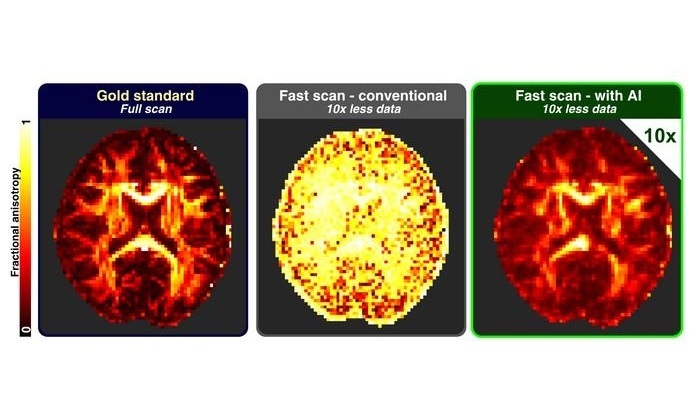
AI Approach Could Shorten Advanced Brain MRI Scans by Up to 90%
Long acquisition times for advanced brain magnetic resonance imaging (MRI) can limit access, extend waiting lists, and disrupt clinical workflows. Reducing data requirements without sacrificing image fidelity... Read more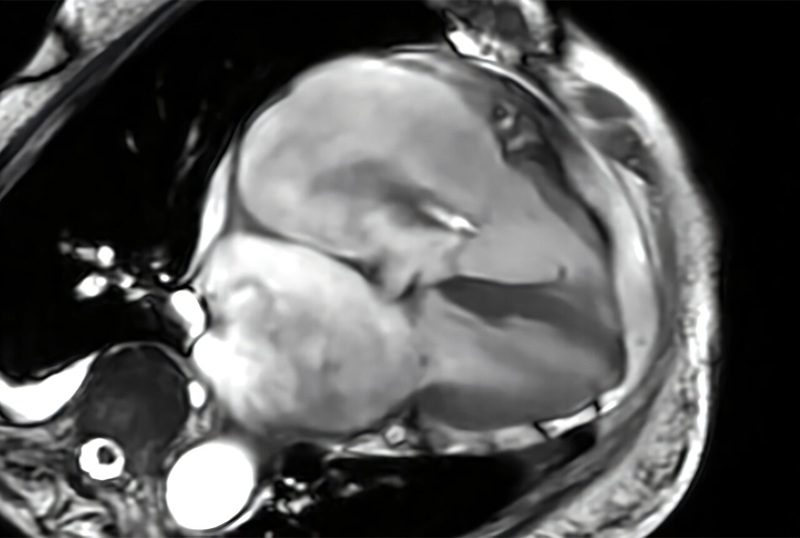
Cardiac MRI Measure Improves Risk Prediction in Tricuspid Regurgitation
Tricuspid regurgitation, in which blood flows back from the right ventricle into the right atrium, can lead to progressive right-sided heart failure. Clinicians need reliable ways to gauge severity and... Read moreUltrasound
view channelAI Robotic Ultrasound System Automates Echocardiography and Improves Consistency
Echocardiography, an ultrasound examination of the heart, is central to diagnosing and managing cardiovascular disease. Many services struggle with limited availability of skilled sonographers, variable... Read more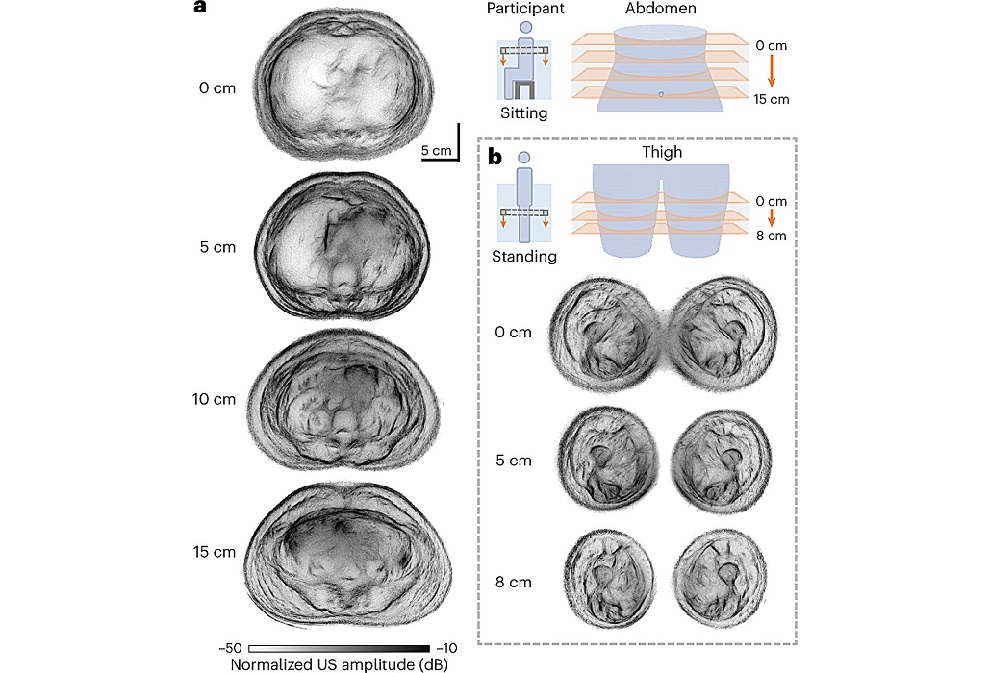
Whole Cross-Section Ultrasound System Enables Operator-Independent Imaging
Conventional ultrasound is central to bedside imaging but is limited by a narrow field of view and operator variability. Comprehensive cross-sectional assessment typically requires computed tomography... Read moreNuclear Medicine
view channel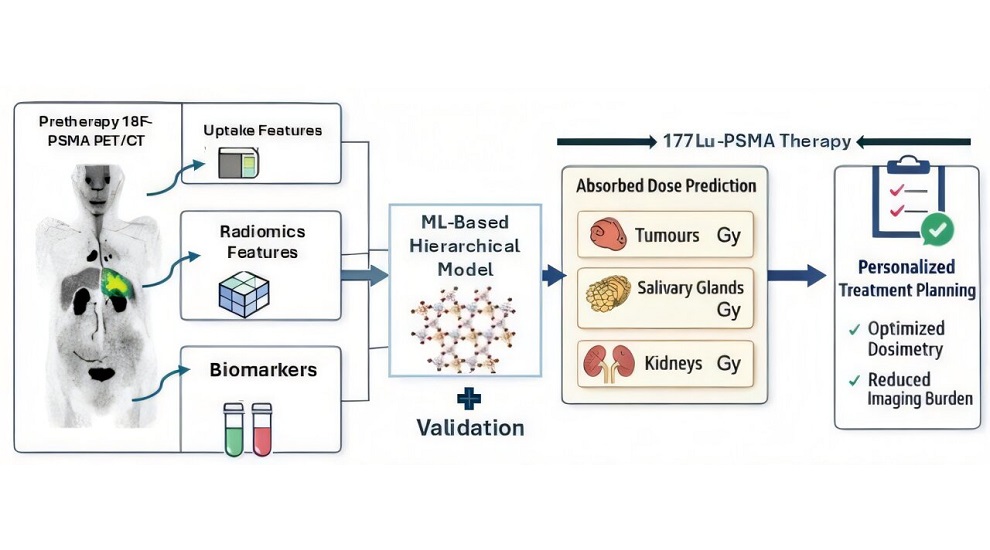
AI Model Predicts Radiation Dose Before Prostate Cancer Therapy
Metastatic castration-resistant prostate cancer (mCRPC) is an advanced form of disease that progresses despite androgen-deprivation therapy and frequently spreads to bone and visceral organs.... Read more
Vault-Free Radiosurgery Platform Expands Access to Cranial Tumor Care
Brain tumors and certain skull base lesions often require precise, non-invasive treatment that protects nearby critical structures. Although stereotactic radiosurgery (SRS) enables outpatient therapy without... Read moreGeneral/Advanced Imaging
view channelMultimodal AI Tool Combines CT and Health Records to Predict Heart Risk
Cardiovascular disease is a leading cause of death and an underrecognized risk for people treated for breast cancer. Cardiac complications can affect survival and quality of life. Clinicians need tools... Read more
AI Tool Automates Radiotherapy Planning for Cervical and Prostate Cancer
Cervical cancer causes most of its global mortality in low- and middle-income countries, where radiotherapy capacity and specialist staff are limited. Treatment planning is labor-intensive and can delay... Read moreImaging IT
view channel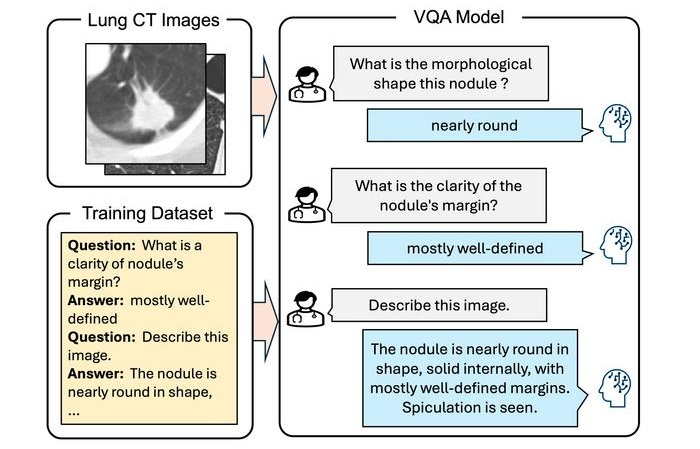
Interactive AI Tool Supports Explainable Lung Nodule Assessment
Lung cancer is a leading cause of cancer mortality, and timely characterization of pulmonary nodules on chest computed tomography (CT) is essential for directing care. Interpreting nodule morphology demands... Read more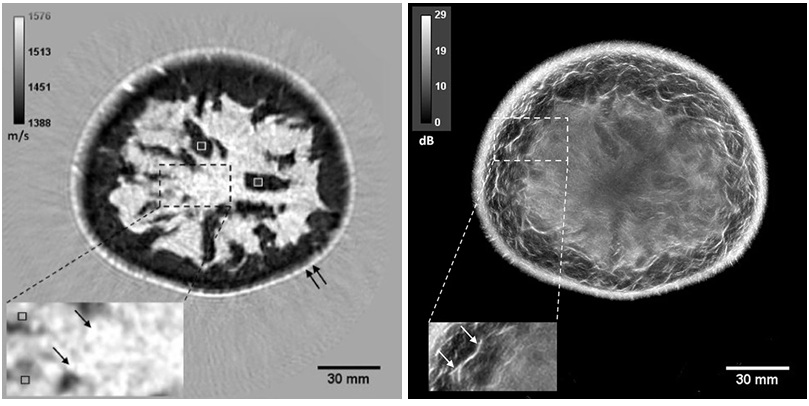
Breast Imaging Software Enhances Visualization and Tissue Characterization in Challenging Cases
Breast imaging can be particularly challenging in cases involving small breasts or implants, where image reconstruction and tissue characterization may be limited. Clinicians also need reproducible analysis... Read more
New Google Cloud Medical Imaging Suite Makes Imaging Healthcare Data More Accessible
Medical imaging is a critical tool used to diagnose patients, and there are billions of medical images scanned globally each year. Imaging data accounts for about 90% of all healthcare data1 and, until... Read more