Fetal MRI Superior for Detecting Zika Brain Damage
|
By MedImaging International staff writers Posted on 18 Oct 2017 |
Image: An illustration of Zika virus in the blood (Photo courtesy of SPL).
Fetal magnetic resonance imaging (MRI) should be used in addition to ultrasound (US) to reveal the extent of brain damage caused by the Zika virus in the developing brain, claims a new study.
Researchers at Children's National Health System (CNHS; Washington, DC, USA) conducted a longitudinal neuroimaging study that enrolled 48 pregnant women exposed to the Zika virus in the first or second trimester, and whose infection was confirmed by reverse transcription polymerase chain reaction (PCR) and/or Immunoglobulin M testing. Of the study participants, 46 live in Barranquilla (Colombia), where Zika infection is endemic, and two women live in the Washington DC (USA) region and were exposed to Zika during travel elsewhere.
All of the women underwent at least one diagnostic imaging session while pregnant, receiving an initial MRI or US at 25.1 weeks gestational age, with 36 women undergoing a second MRI/US imaging pair at roughly 31 weeks gestation. Three of the pregnancies (6%) were marked by abnormal fetal MRIs. One fetus had heterotopias and abnormal cortical indent; but the ultrasound taken at the same gestational age showed its brain was developing normally. Another fetus had parietal encephalocele and Chiari malformation Type II, with US also detecting these brain abnormalities.
A third fetus had a thin corpus callosum, abnormally developed brain stem, temporal cysts, general cerebral and cerebellar atrophy, and subependymal heterotopias. US revealed major ventriculomegaly and a fetal head circumference that decreased sharply from the 32nd to 36th gestational week, a hallmark of microcephaly. After the children were born, the infants underwent a follow-up MRI without sedation and another US. For nine infants, the US revealed cysts in the choroid plexus or germinal matrix, and one infant's US after birth showed lenticulostriate vasculopathy brain lesions. The study was presented at the annual IDWeek meeting, held during October 2017 in San Diego (CA, USA).
“MRI and US provide complementary data needed to assess ongoing changes to the brains of fetuses exposed to Zika in utero,” said lead author and study presenter CNHS fetal/neonatal neurologist Sarah Mulkey, MD, PhD. “In addition, our study found that relying on ultrasound alone would have given one mother the false assurance that her fetus' brain was developing normally, while the sharper MRI clearly pointed to brain abnormalities.”
Zika virus is a member of the Flaviviridae family, of the genus Flavivirus, and is transmitted by the daytime-active Aedes mosquitoes. In adults, the virus causes a mild illness known as Zika fever. Locally transmitted Zika virus was first reported in Brazil in May 2015, and since then health authorities have estimated that around a million suspected cases have occurred. Brazilian health authorities also observed a significant increase in the number of detected cases of microcephaly and Guillain-Barré Syndrome affecting fetuses and newborns.
Related Links:
Children's National Health System
Researchers at Children's National Health System (CNHS; Washington, DC, USA) conducted a longitudinal neuroimaging study that enrolled 48 pregnant women exposed to the Zika virus in the first or second trimester, and whose infection was confirmed by reverse transcription polymerase chain reaction (PCR) and/or Immunoglobulin M testing. Of the study participants, 46 live in Barranquilla (Colombia), where Zika infection is endemic, and two women live in the Washington DC (USA) region and were exposed to Zika during travel elsewhere.
All of the women underwent at least one diagnostic imaging session while pregnant, receiving an initial MRI or US at 25.1 weeks gestational age, with 36 women undergoing a second MRI/US imaging pair at roughly 31 weeks gestation. Three of the pregnancies (6%) were marked by abnormal fetal MRIs. One fetus had heterotopias and abnormal cortical indent; but the ultrasound taken at the same gestational age showed its brain was developing normally. Another fetus had parietal encephalocele and Chiari malformation Type II, with US also detecting these brain abnormalities.
A third fetus had a thin corpus callosum, abnormally developed brain stem, temporal cysts, general cerebral and cerebellar atrophy, and subependymal heterotopias. US revealed major ventriculomegaly and a fetal head circumference that decreased sharply from the 32nd to 36th gestational week, a hallmark of microcephaly. After the children were born, the infants underwent a follow-up MRI without sedation and another US. For nine infants, the US revealed cysts in the choroid plexus or germinal matrix, and one infant's US after birth showed lenticulostriate vasculopathy brain lesions. The study was presented at the annual IDWeek meeting, held during October 2017 in San Diego (CA, USA).
“MRI and US provide complementary data needed to assess ongoing changes to the brains of fetuses exposed to Zika in utero,” said lead author and study presenter CNHS fetal/neonatal neurologist Sarah Mulkey, MD, PhD. “In addition, our study found that relying on ultrasound alone would have given one mother the false assurance that her fetus' brain was developing normally, while the sharper MRI clearly pointed to brain abnormalities.”
Zika virus is a member of the Flaviviridae family, of the genus Flavivirus, and is transmitted by the daytime-active Aedes mosquitoes. In adults, the virus causes a mild illness known as Zika fever. Locally transmitted Zika virus was first reported in Brazil in May 2015, and since then health authorities have estimated that around a million suspected cases have occurred. Brazilian health authorities also observed a significant increase in the number of detected cases of microcephaly and Guillain-Barré Syndrome affecting fetuses and newborns.
Related Links:
Children's National Health System
Latest MRI News
- Diamond Dust Could Offer New Contrast Agent Option for Future MRI Scans
- Combining MRI with PSA Testing Improves Clinical Outcomes for Prostate Cancer Patients
- PET/MRI Improves Diagnostic Accuracy for Prostate Cancer Patients
- Next Generation MR-Guided Focused Ultrasound Ushers In Future of Incisionless Neurosurgery
- Two-Part MRI Scan Detects Prostate Cancer More Quickly without Compromising Diagnostic Quality
- World’s Most Powerful MRI Machine Images Living Brain with Unrivaled Clarity
- New Whole-Body Imaging Technology Makes It Possible to View Inflammation on MRI Scan
- Combining Prostate MRI with Blood Test Can Avoid Unnecessary Prostate Biopsies
- New Treatment Combines MRI and Ultrasound to Control Prostate Cancer without Serious Side Effects
- MRI Improves Diagnosis and Treatment of Prostate Cancer
- Combined PET-MRI Scan Improves Treatment for Early Breast Cancer Patients
- 4D MRI Could Improve Clinical Assessment of Heart Blood Flow Abnormalities
- MRI-Guided Focused Ultrasound Therapy Shows Promise in Treating Prostate Cancer
- AI-Based MRI Tool Outperforms Current Brain Tumor Diagnosis Methods
- DW-MRI Lights up Small Ovarian Lesions like Light Bulbs
- Abbreviated Breast MRI Effective for High-Risk Screening without Compromising Diagnostic Accuracy
Channels
Radiography
view channel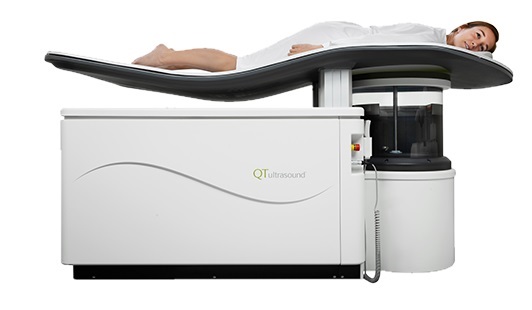
Novel Breast Imaging System Proves As Effective As Mammography
Breast cancer remains the most frequently diagnosed cancer among women. It is projected that one in eight women will be diagnosed with breast cancer during her lifetime, and one in 42 women who turn 50... Read more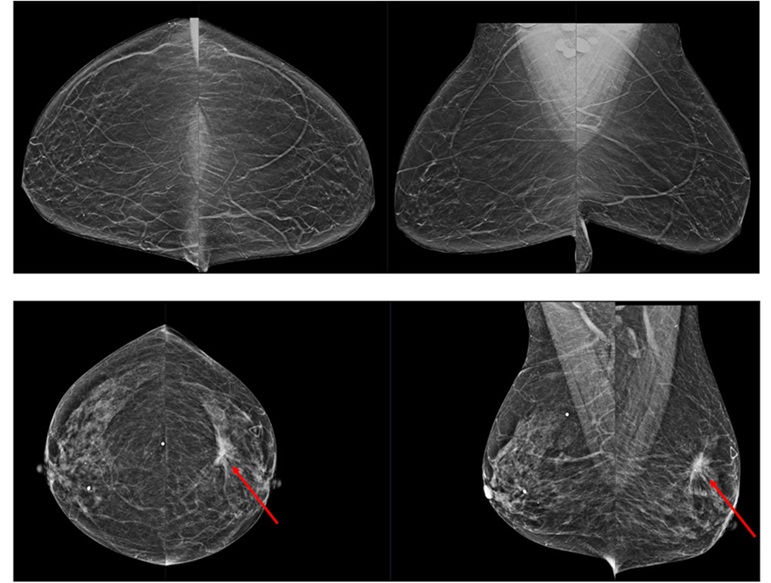
AI Assistance Improves Breast-Cancer Screening by Reducing False Positives
Radiologists typically detect one case of cancer for every 200 mammograms reviewed. However, these evaluations often result in false positives, leading to unnecessary patient recalls for additional testing,... Read moreUltrasound
view channel.jpg)
Groundbreaking Technology Enables Precise, Automatic Measurement of Peripheral Blood Vessels
The current standard of care of using angiographic information is often inadequate for accurately assessing vessel size in the estimated 20 million people in the U.S. who suffer from peripheral vascular disease.... Read more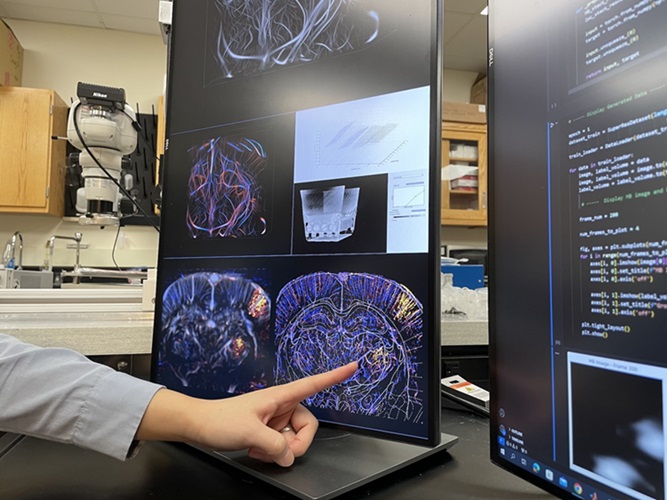
Deep Learning Advances Super-Resolution Ultrasound Imaging
Ultrasound localization microscopy (ULM) is an advanced imaging technique that offers high-resolution visualization of microvascular structures. It employs microbubbles, FDA-approved contrast agents, injected... Read more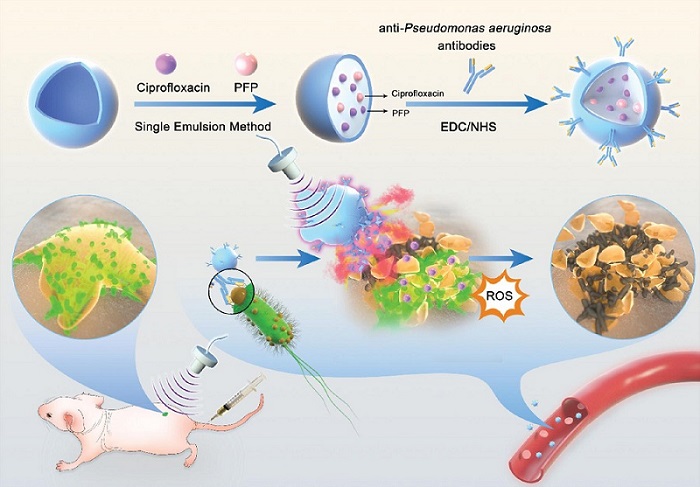
Novel Ultrasound-Launched Targeted Nanoparticle Eliminates Biofilm and Bacterial Infection
Biofilms, formed by bacteria aggregating into dense communities for protection against harsh environmental conditions, are a significant contributor to various infectious diseases. Biofilms frequently... Read moreNuclear Medicine
view channel
New Imaging Technique Monitors Inflammation Disorders without Radiation Exposure
Imaging inflammation using traditional radiological techniques presents significant challenges, including radiation exposure, poor image quality, high costs, and invasive procedures. Now, new contrast... Read more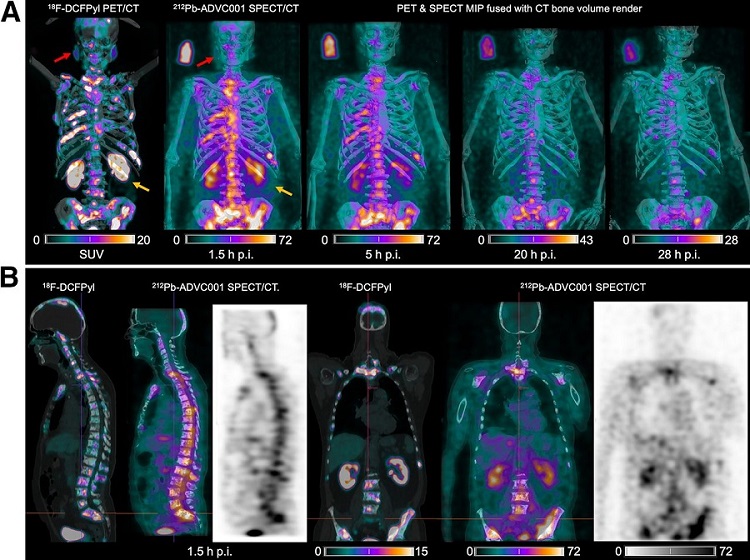
New SPECT/CT Technique Could Change Imaging Practices and Increase Patient Access
The development of lead-212 (212Pb)-PSMA–based targeted alpha therapy (TAT) is garnering significant interest in treating patients with metastatic castration-resistant prostate cancer. The imaging of 212Pb,... Read moreNew Radiotheranostic System Detects and Treats Ovarian Cancer Noninvasively
Ovarian cancer is the most lethal gynecological cancer, with less than a 30% five-year survival rate for those diagnosed in late stages. Despite surgery and platinum-based chemotherapy being the standard... Read more
AI System Automatically and Reliably Detects Cardiac Amyloidosis Using Scintigraphy Imaging
Cardiac amyloidosis, a condition characterized by the buildup of abnormal protein deposits (amyloids) in the heart muscle, severely affects heart function and can lead to heart failure or death without... Read moreGeneral/Advanced Imaging
view channel
PET Scans Reveal Hidden Inflammation in Multiple Sclerosis Patients
A key challenge for clinicians treating patients with multiple sclerosis (MS) is that after a certain amount of time, they continue to worsen even though their MRIs show no change. A new study has now... Read more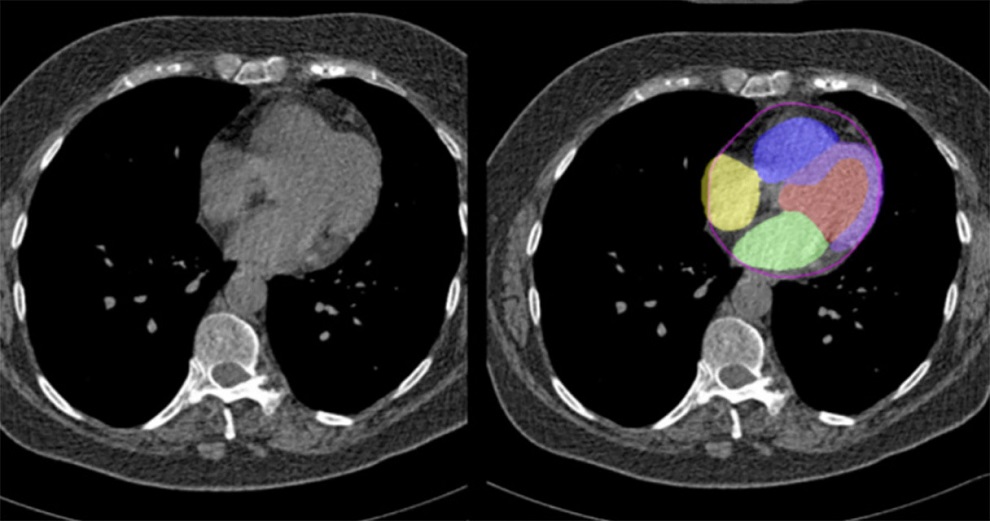
Artificial Intelligence Evaluates Cardiovascular Risk from CT Scans
Chest computed tomography (CT) is a common diagnostic tool, with approximately 15 million scans conducted each year in the United States, though many are underutilized or not fully explored.... Read more
New AI Method Captures Uncertainty in Medical Images
In the field of biomedicine, segmentation is the process of annotating pixels from an important structure in medical images, such as organs or cells. Artificial Intelligence (AI) models are utilized to... Read more.jpg)
CT Coronary Angiography Reduces Need for Invasive Tests to Diagnose Coronary Artery Disease
Coronary artery disease (CAD), one of the leading causes of death worldwide, involves the narrowing of coronary arteries due to atherosclerosis, resulting in insufficient blood flow to the heart muscle.... Read moreImaging IT
view channel
New Google Cloud Medical Imaging Suite Makes Imaging Healthcare Data More Accessible
Medical imaging is a critical tool used to diagnose patients, and there are billions of medical images scanned globally each year. Imaging data accounts for about 90% of all healthcare data1 and, until... Read more
Global AI in Medical Diagnostics Market to Be Driven by Demand for Image Recognition in Radiology
The global artificial intelligence (AI) in medical diagnostics market is expanding with early disease detection being one of its key applications and image recognition becoming a compelling consumer proposition... Read moreIndustry News
view channel
Bayer and Google Partner on New AI Product for Radiologists
Medical imaging data comprises around 90% of all healthcare data, and it is a highly complex and rich clinical data modality and serves as a vital tool for diagnosing patients. Each year, billions of medical... Read more