Play-Based Preparation Helps Children Undergoing Radiation Therapy
|
By MedImaging International staff writers Posted on 26 May 2016 |
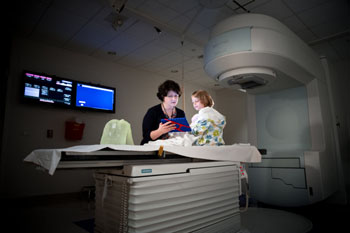
Image: Child Life Specialist Amy Kennedy helps a patient prepare for RT (Photo courtesy of St. Jude Children\'s Research Hospital).
Support interventions by child life specialists decrease sedation use and costs associated with radiation therapy (RT) for brain cancer, according to a new study.
Researchers at St. Jude Children's Research Hospital (St. Jude; Memphis, TN, USA) conducted a retrospective chart review of 116 children aged 5–12 years in order to examine the relationship between play-based procedural preparation and support intervention, and use of sedation in children with central nervous system (CNS) tumors during RT.
Outcome measures included the total number of RT sessions, the number of treatments received with and without sedation, and the type and duration of interventions, which consisted of developmentally appropriate play, education, preparation, and distraction provided by a certified child life specialist. A secondary objective was to analyze the cost-effectiveness of the intervention, compared to costs associated with daily sedation alone.
The results showed that age and tumor location affected sedation use. Each one-year increase in patient age was associated with significantly higher odds of receiving cranial RT without any sedation. After adjusting for age, tumor location, and craniospinal radiation, each additional intervention session with the child life specialist was associated with a 23% increase in the odds of receiving cranial radiation with partial sedation over full sedation. The study was published in the June 2016 issue of Supportive Care in Cancer.
“The child life specialist will set up practice sessions where the patient will have the opportunity to lie on the table to see what it will be like before the actual radiation therapy session,” said lead author Shawna Grissom, director of Child Life at St. Jude. “The specialist will work with the child to practice lying still and will work with the patient on coping skills. Child life specialists can also help during radiation sessions by reading books to the children, leading them through guided imagery or checking on them during breaks to make sure they are coping well.”
“Play-based programming implemented by a certified child life specialist can help provide a sense of accomplishment for the patients that they can get through these treatment sessions often with less or no sedation,” concluded Ms. Grissom, who added that “less sedation for the children means fewer clinical risks, less time in treatment sessions, and reduced health care costs that can approach USD 80,000 per patient.”
CNS tumors are the most commonly diagnosed solid tumors in childhood, accounting for nearly 20% of all pediatric cancers in the U.S. Although RT is effective, it is stressful for children who must lie still throughout the process to avoid unintended exposure to their developing brains. Sedation is often used to ensure precise positioning, but on the other hand, sedation in children may be associated with several health risks, including respiratory ailments and cognitive functioning deficits.
Related Links:
St. Jude Children's Research Hospital
Researchers at St. Jude Children's Research Hospital (St. Jude; Memphis, TN, USA) conducted a retrospective chart review of 116 children aged 5–12 years in order to examine the relationship between play-based procedural preparation and support intervention, and use of sedation in children with central nervous system (CNS) tumors during RT.
Outcome measures included the total number of RT sessions, the number of treatments received with and without sedation, and the type and duration of interventions, which consisted of developmentally appropriate play, education, preparation, and distraction provided by a certified child life specialist. A secondary objective was to analyze the cost-effectiveness of the intervention, compared to costs associated with daily sedation alone.
The results showed that age and tumor location affected sedation use. Each one-year increase in patient age was associated with significantly higher odds of receiving cranial RT without any sedation. After adjusting for age, tumor location, and craniospinal radiation, each additional intervention session with the child life specialist was associated with a 23% increase in the odds of receiving cranial radiation with partial sedation over full sedation. The study was published in the June 2016 issue of Supportive Care in Cancer.
“The child life specialist will set up practice sessions where the patient will have the opportunity to lie on the table to see what it will be like before the actual radiation therapy session,” said lead author Shawna Grissom, director of Child Life at St. Jude. “The specialist will work with the child to practice lying still and will work with the patient on coping skills. Child life specialists can also help during radiation sessions by reading books to the children, leading them through guided imagery or checking on them during breaks to make sure they are coping well.”
“Play-based programming implemented by a certified child life specialist can help provide a sense of accomplishment for the patients that they can get through these treatment sessions often with less or no sedation,” concluded Ms. Grissom, who added that “less sedation for the children means fewer clinical risks, less time in treatment sessions, and reduced health care costs that can approach USD 80,000 per patient.”
CNS tumors are the most commonly diagnosed solid tumors in childhood, accounting for nearly 20% of all pediatric cancers in the U.S. Although RT is effective, it is stressful for children who must lie still throughout the process to avoid unintended exposure to their developing brains. Sedation is often used to ensure precise positioning, but on the other hand, sedation in children may be associated with several health risks, including respiratory ailments and cognitive functioning deficits.
Related Links:
St. Jude Children's Research Hospital
Latest Radiography News
- Novel Breast Imaging System Proves As Effective As Mammography
- AI Assistance Improves Breast-Cancer Screening by Reducing False Positives
- AI Could Boost Clinical Adoption of Chest DDR
- 3D Mammography Almost Halves Breast Cancer Incidence between Two Screening Tests
- AI Model Predicts 5-Year Breast Cancer Risk from Mammograms
- Deep Learning Framework Detects Fractures in X-Ray Images With 99% Accuracy
- Direct AI-Based Medical X-Ray Imaging System a Paradigm-Shift from Conventional DR and CT
- Chest X-Ray AI Solution Automatically Identifies, Categorizes and Highlights Suspicious Areas
- AI Diagnoses Wrist Fractures As Well As Radiologists
- Annual Mammography Beginning At 40 Cuts Breast Cancer Mortality By 42%
- 3D Human GPS Powered By Light Paves Way for Radiation-Free Minimally-Invasive Surgery
- Novel AI Technology to Revolutionize Cancer Detection in Dense Breasts
- AI Solution Provides Radiologists with 'Second Pair' Of Eyes to Detect Breast Cancers
- AI Helps General Radiologists Achieve Specialist-Level Performance in Interpreting Mammograms
- Novel Imaging Technique Could Transform Breast Cancer Detection
- Computer Program Combines AI and Heat-Imaging Technology for Early Breast Cancer Detection
Channels
MRI
view channel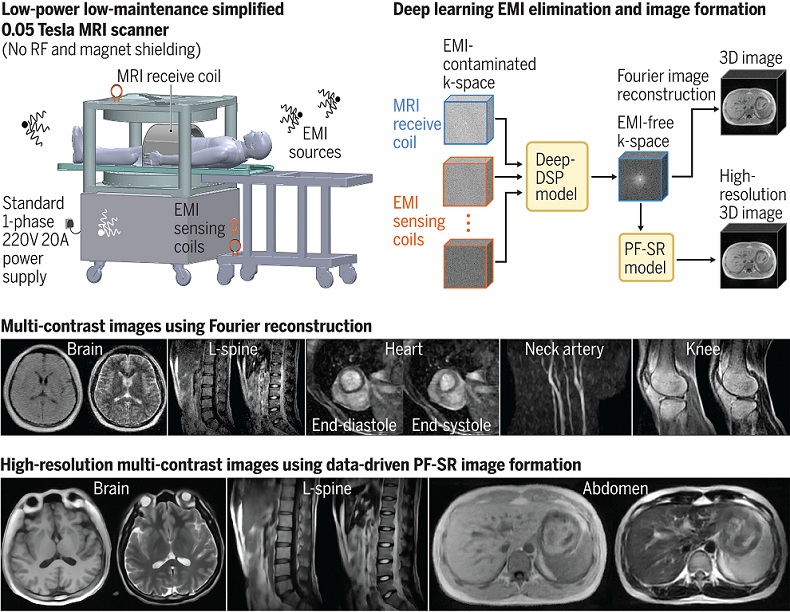
Low-Cost Whole-Body MRI Device Combined with AI Generates High-Quality Results
Magnetic Resonance Imaging (MRI) has significantly transformed healthcare, providing a noninvasive, radiation-free method for detailed imaging. It is especially promising for the future of medical diagnosis... Read more
World's First Whole-Body Ultra-High Field MRI Officially Comes To Market
The world's first whole-body ultra-high field (UHF) MRI has officially come to market, marking a remarkable advancement in diagnostic radiology. United Imaging (Shanghai, China) has secured clearance from the U.... Read moreUltrasound
view channel.jpg)
Diagnostic System Automatically Analyzes TTE Images to Identify Congenital Heart Disease
Congenital heart disease (CHD) is one of the most prevalent congenital anomalies worldwide, presenting substantial health and financial challenges for affected patients. Early detection and treatment of... Read more
Super-Resolution Imaging Technique Could Improve Evaluation of Cardiac Conditions
The heart depends on efficient blood circulation to pump blood throughout the body, delivering oxygen to tissues and removing carbon dioxide and waste. Yet, when heart vessels are damaged, it can disrupt... Read more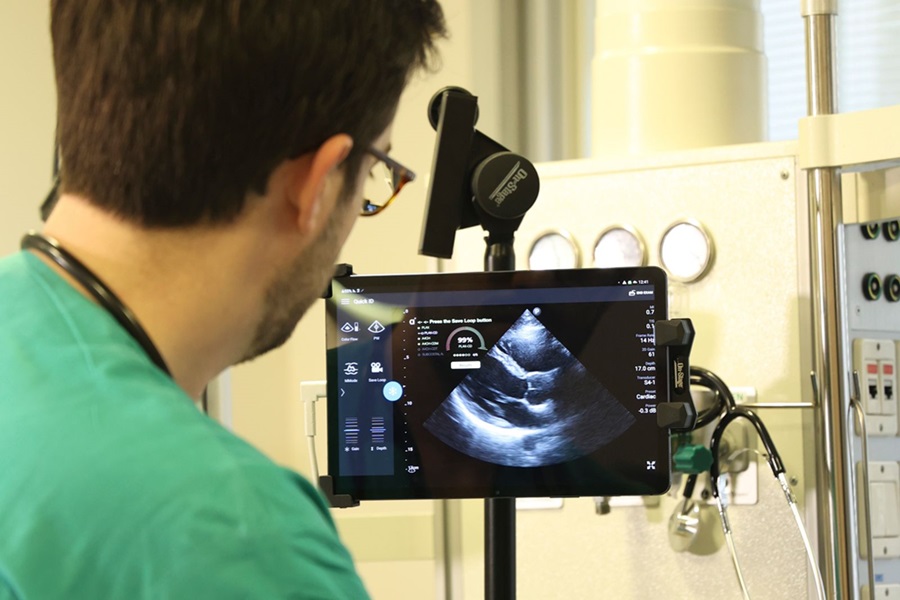
First AI-Powered POC Ultrasound Diagnostic Solution Helps Prioritize Cases Based On Severity
Ultrasound scans are essential for identifying and diagnosing various medical conditions, but often, patients must wait weeks or months for results due to a shortage of qualified medical professionals... Read moreNuclear Medicine
view channelNew PET Agent Rapidly and Accurately Visualizes Lesions in Clear Cell Renal Cell Carcinoma Patients
Clear cell renal cell cancer (ccRCC) represents 70-80% of renal cell carcinoma cases. While localized disease can be effectively treated with surgery and ablative therapies, one-third of patients either... Read more
New Imaging Technique Monitors Inflammation Disorders without Radiation Exposure
Imaging inflammation using traditional radiological techniques presents significant challenges, including radiation exposure, poor image quality, high costs, and invasive procedures. Now, new contrast... Read more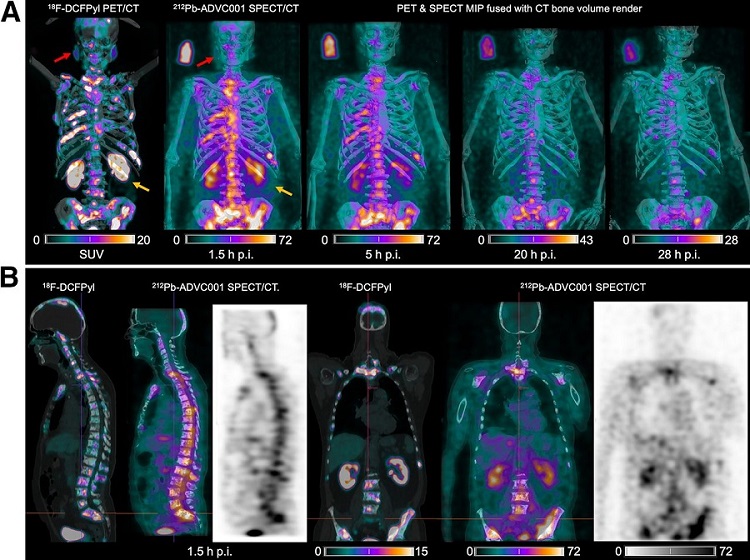
New SPECT/CT Technique Could Change Imaging Practices and Increase Patient Access
The development of lead-212 (212Pb)-PSMA–based targeted alpha therapy (TAT) is garnering significant interest in treating patients with metastatic castration-resistant prostate cancer. The imaging of 212Pb,... Read moreGeneral/Advanced Imaging
view channelBone Density Test Uses Existing CT Images to Predict Fractures
Osteoporotic fractures are not only devastating and deadly, especially hip fractures, but also impose significant costs. They rank among the top chronic diseases in terms of disability-adjusted life years... Read more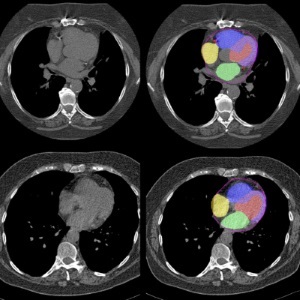
AI Predicts Cardiac Risk and Mortality from Routine Chest CT Scans
Heart disease remains the leading cause of death and is largely preventable, yet many individuals are unaware of their risk until it becomes severe. Early detection through screening can reveal heart issues,... Read moreImaging IT
view channel
New Google Cloud Medical Imaging Suite Makes Imaging Healthcare Data More Accessible
Medical imaging is a critical tool used to diagnose patients, and there are billions of medical images scanned globally each year. Imaging data accounts for about 90% of all healthcare data1 and, until... Read more
Global AI in Medical Diagnostics Market to Be Driven by Demand for Image Recognition in Radiology
The global artificial intelligence (AI) in medical diagnostics market is expanding with early disease detection being one of its key applications and image recognition becoming a compelling consumer proposition... Read moreIndustry News
view channel
Hologic Acquires UK-Based Breast Surgical Guidance Company Endomagnetics Ltd.
Hologic, Inc. (Marlborough, MA, USA) has entered into a definitive agreement to acquire Endomagnetics Ltd. (Cambridge, UK), a privately held developer of breast cancer surgery technologies, for approximately... Read more
Bayer and Google Partner on New AI Product for Radiologists
Medical imaging data comprises around 90% of all healthcare data, and it is a highly complex and rich clinical data modality and serves as a vital tool for diagnosing patients. Each year, billions of medical... Read more