3D Mammography Helps Detect Breast Cancer Earlier
|
By MedImaging International staff writers Posted on 06 Mar 2016 |
A new study concludes that screening with digital breast tomosynthesis (DBT) combined with digital mammography (DM) increases breast cancer detection rates.
Researchers at the University of Pennsylvania (Philadelphia, USA) conducted a retrospective, four-year study of screening mammography metrics to determine if the improved outcomes observed after initial implementation of DBT screening are sustainable over time, and to evaluate the effect of more than one DBT screening at the individual level. In all, 44,468 screening events were performed on 23,958 unique women. The researchers then assessed the differences in outcomes between each DBT year and the DM year.
The researchers evaluated the results between groups of women with only 1, 2, or 3 DBT screenings, and also calculated the odds of recall adjusted for age, race and ethnicity, breast density, and prior mammograms. The results showed that the yearly rate of women called back for additional imaging decreased with the number of years they received three dimensional (3D) DBT mammography exams. Per 1,000 women, 130 were recalled in the first year of 3D mammography exams, 78 after two years, and only 59 after three years.
The analysis also showed that the yearly rate of women called back for additional imaging with 3D DBT mammography was consistently lower than the rate with standard 2D mammography. Concomitantly, the cancer detection rate per 1,000 women increased from 4.6 with 2D mammography to 5.5 in year one of 3D DBT mammography screenings, 5.8 in year two, and 6.1 in year three. Interval cancer rates decreased from 0.7% with the use of DM to 0.5% with the use of DBT. The study was published on February 18, 2016, in JAMA Oncology.
“We found that reduction in recall was sustainable at a population level, with additional reduction in recall as women returned for a second and third DBT examination,” concluded senior author Emily Conant, MD, and colleagues of the department of radiology and the computational breast imaging group. “These findings reaffirm that 3D mammography is a better mammogram for breast cancer screening […] and are an important step toward informing policies so that all women can receive 3D mammography for screening.”
DBT mammograms use low dose X-rays to create a 3D image of the breast, which can then be viewed in narrow slices, similarly to CT scan images. While in conventional 2D mammography overlapping tissues can mask suspicious areas, 3D images eliminate the overlap, making abnormalities easier to recognize. Experts estimate that 3D mammography will replace conventional mammography within ten years.
Related Links:
University of Pennsylvania
Researchers at the University of Pennsylvania (Philadelphia, USA) conducted a retrospective, four-year study of screening mammography metrics to determine if the improved outcomes observed after initial implementation of DBT screening are sustainable over time, and to evaluate the effect of more than one DBT screening at the individual level. In all, 44,468 screening events were performed on 23,958 unique women. The researchers then assessed the differences in outcomes between each DBT year and the DM year.
The researchers evaluated the results between groups of women with only 1, 2, or 3 DBT screenings, and also calculated the odds of recall adjusted for age, race and ethnicity, breast density, and prior mammograms. The results showed that the yearly rate of women called back for additional imaging decreased with the number of years they received three dimensional (3D) DBT mammography exams. Per 1,000 women, 130 were recalled in the first year of 3D mammography exams, 78 after two years, and only 59 after three years.
The analysis also showed that the yearly rate of women called back for additional imaging with 3D DBT mammography was consistently lower than the rate with standard 2D mammography. Concomitantly, the cancer detection rate per 1,000 women increased from 4.6 with 2D mammography to 5.5 in year one of 3D DBT mammography screenings, 5.8 in year two, and 6.1 in year three. Interval cancer rates decreased from 0.7% with the use of DM to 0.5% with the use of DBT. The study was published on February 18, 2016, in JAMA Oncology.
“We found that reduction in recall was sustainable at a population level, with additional reduction in recall as women returned for a second and third DBT examination,” concluded senior author Emily Conant, MD, and colleagues of the department of radiology and the computational breast imaging group. “These findings reaffirm that 3D mammography is a better mammogram for breast cancer screening […] and are an important step toward informing policies so that all women can receive 3D mammography for screening.”
DBT mammograms use low dose X-rays to create a 3D image of the breast, which can then be viewed in narrow slices, similarly to CT scan images. While in conventional 2D mammography overlapping tissues can mask suspicious areas, 3D images eliminate the overlap, making abnormalities easier to recognize. Experts estimate that 3D mammography will replace conventional mammography within ten years.
Related Links:
University of Pennsylvania
Latest Radiography News
- Novel Breast Imaging System Proves As Effective As Mammography
- AI Assistance Improves Breast-Cancer Screening by Reducing False Positives
- AI Could Boost Clinical Adoption of Chest DDR
- 3D Mammography Almost Halves Breast Cancer Incidence between Two Screening Tests
- AI Model Predicts 5-Year Breast Cancer Risk from Mammograms
- Deep Learning Framework Detects Fractures in X-Ray Images With 99% Accuracy
- Direct AI-Based Medical X-Ray Imaging System a Paradigm-Shift from Conventional DR and CT
- Chest X-Ray AI Solution Automatically Identifies, Categorizes and Highlights Suspicious Areas
- AI Diagnoses Wrist Fractures As Well As Radiologists
- Annual Mammography Beginning At 40 Cuts Breast Cancer Mortality By 42%
- 3D Human GPS Powered By Light Paves Way for Radiation-Free Minimally-Invasive Surgery
- Novel AI Technology to Revolutionize Cancer Detection in Dense Breasts
- AI Solution Provides Radiologists with 'Second Pair' Of Eyes to Detect Breast Cancers
- AI Helps General Radiologists Achieve Specialist-Level Performance in Interpreting Mammograms
- Novel Imaging Technique Could Transform Breast Cancer Detection
- Computer Program Combines AI and Heat-Imaging Technology for Early Breast Cancer Detection
Channels
MRI
view channel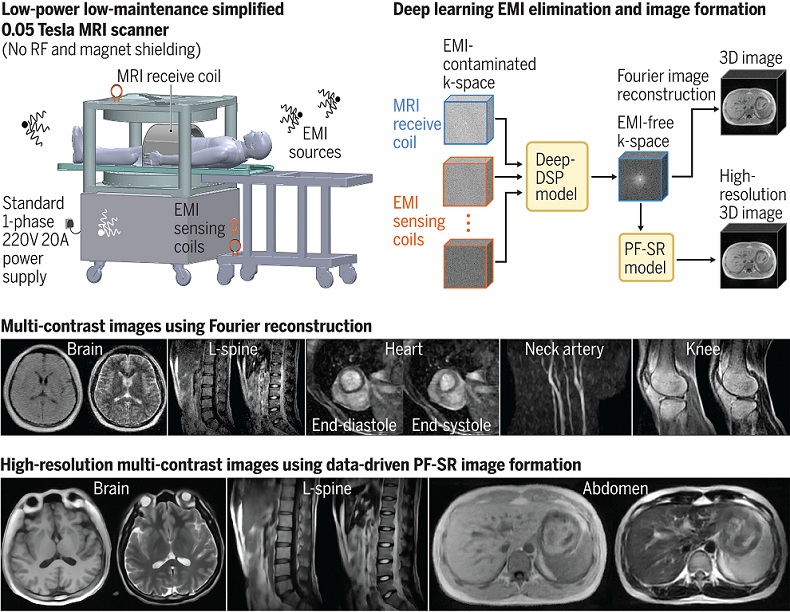
Low-Cost Whole-Body MRI Device Combined with AI Generates High-Quality Results
Magnetic Resonance Imaging (MRI) has significantly transformed healthcare, providing a noninvasive, radiation-free method for detailed imaging. It is especially promising for the future of medical diagnosis... Read more
World's First Whole-Body Ultra-High Field MRI Officially Comes To Market
The world's first whole-body ultra-high field (UHF) MRI has officially come to market, marking a remarkable advancement in diagnostic radiology. United Imaging (Shanghai, China) has secured clearance from the U.... Read moreUltrasound
view channel.jpg)
Diagnostic System Automatically Analyzes TTE Images to Identify Congenital Heart Disease
Congenital heart disease (CHD) is one of the most prevalent congenital anomalies worldwide, presenting substantial health and financial challenges for affected patients. Early detection and treatment of... Read more
Super-Resolution Imaging Technique Could Improve Evaluation of Cardiac Conditions
The heart depends on efficient blood circulation to pump blood throughout the body, delivering oxygen to tissues and removing carbon dioxide and waste. Yet, when heart vessels are damaged, it can disrupt... Read more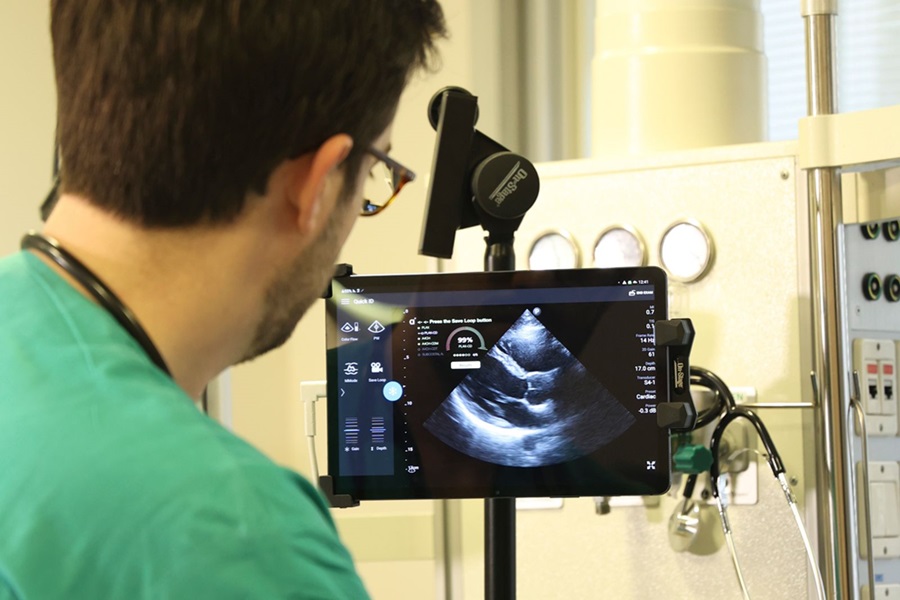
First AI-Powered POC Ultrasound Diagnostic Solution Helps Prioritize Cases Based On Severity
Ultrasound scans are essential for identifying and diagnosing various medical conditions, but often, patients must wait weeks or months for results due to a shortage of qualified medical professionals... Read moreNuclear Medicine
view channelNew PET Agent Rapidly and Accurately Visualizes Lesions in Clear Cell Renal Cell Carcinoma Patients
Clear cell renal cell cancer (ccRCC) represents 70-80% of renal cell carcinoma cases. While localized disease can be effectively treated with surgery and ablative therapies, one-third of patients either... Read more
New Imaging Technique Monitors Inflammation Disorders without Radiation Exposure
Imaging inflammation using traditional radiological techniques presents significant challenges, including radiation exposure, poor image quality, high costs, and invasive procedures. Now, new contrast... Read more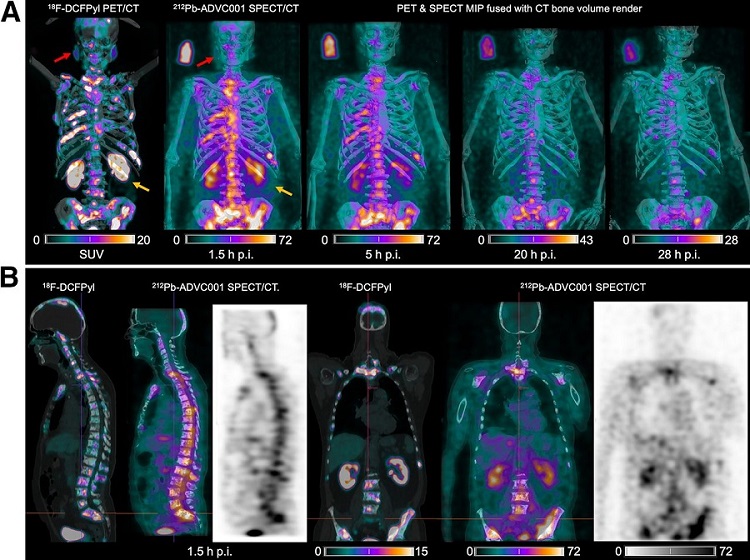
New SPECT/CT Technique Could Change Imaging Practices and Increase Patient Access
The development of lead-212 (212Pb)-PSMA–based targeted alpha therapy (TAT) is garnering significant interest in treating patients with metastatic castration-resistant prostate cancer. The imaging of 212Pb,... Read moreGeneral/Advanced Imaging
view channelBone Density Test Uses Existing CT Images to Predict Fractures
Osteoporotic fractures are not only devastating and deadly, especially hip fractures, but also impose significant costs. They rank among the top chronic diseases in terms of disability-adjusted life years... Read more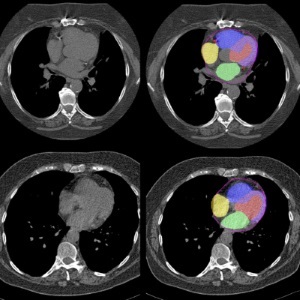
AI Predicts Cardiac Risk and Mortality from Routine Chest CT Scans
Heart disease remains the leading cause of death and is largely preventable, yet many individuals are unaware of their risk until it becomes severe. Early detection through screening can reveal heart issues,... Read moreImaging IT
view channel
New Google Cloud Medical Imaging Suite Makes Imaging Healthcare Data More Accessible
Medical imaging is a critical tool used to diagnose patients, and there are billions of medical images scanned globally each year. Imaging data accounts for about 90% of all healthcare data1 and, until... Read more
Global AI in Medical Diagnostics Market to Be Driven by Demand for Image Recognition in Radiology
The global artificial intelligence (AI) in medical diagnostics market is expanding with early disease detection being one of its key applications and image recognition becoming a compelling consumer proposition... Read moreIndustry News
view channel
Hologic Acquires UK-Based Breast Surgical Guidance Company Endomagnetics Ltd.
Hologic, Inc. (Marlborough, MA, USA) has entered into a definitive agreement to acquire Endomagnetics Ltd. (Cambridge, UK), a privately held developer of breast cancer surgery technologies, for approximately... Read more
Bayer and Google Partner on New AI Product for Radiologists
Medical imaging data comprises around 90% of all healthcare data, and it is a highly complex and rich clinical data modality and serves as a vital tool for diagnosing patients. Each year, billions of medical... Read more