fMRI Could Help Identify New Painkillers
|
By MedImaging International staff writers Posted on 10 Feb 2016 |
Measuring the brain's neural response to pain using functional magnetic resonance imaging (fMRI) may be a viable tool for evaluating the effectiveness of new pain medications, according to a new study.
Researchers at John Radcliffe Hospital (Oxford, United Kingdom) and Oxford University (United Kingdom) conducted a double-blind, randomized study in 24 healthy volunteers on three separate occasions to assess the use of fMRI in obtaining objective outcome measures of drug differentiation. To induce pain, the researchers used capsaicin cream, a topical irritant often used to produce similar characteristics of neuropathic pain on subjects' skin.
Prior to capsaicin cream application, the subjects either received a single dose of gabapentin, which is considered effective and a first line treatment for neuropathic pain; ibuprofen, which is generally not considered an effective treatment for the condition; or a placebo. The researchers then assessed the effect the drugs or placebo had on the brain's neural response to pain using fMRI, in addition to patient-reported pain relief.
The results showed that neural activity was significantly reduced in the subjects who received gabapentin, even with extremely low subject numbers, highlighting the potential for fMRI to make a drug's effect clear in small cohorts, such as during the early stages of human drug development. This ability could provide a much-needed objective method to collect data that could prevent premature discarding of potentially beneficial therapies. The study was published in the January 2106 issue of Anesthesiology.
“Chronic pain is a very common condition. Even the most effective pain medications currently available only provide adequate pain relief, defined as a 50% reduction in pain, in one out of four patients, while some drugs, such as opioids, have significant side effects, including dependence and overuse,” said lead author Vishvarani Wanigasekera, MD, of the University of Oxford. “We believe that neuroimaging techniques, such as fMRI, can provide objective evidence that can be used as outcome measures in early drug development to enhance the efficiency of the drug development process.”
Patient-reported pain relief is the primary outcome measure used in current drug development studies to assess whether medication is effective or not. However, due to their subjective and context-dependent nature, self-reported pain perception and relief are subject to many influences. Due to the low subject population, researchers can also easily miss effective compounds that might work well in the population at large.
Related Links:
John Radcliffe Hospital
Oxford University
Researchers at John Radcliffe Hospital (Oxford, United Kingdom) and Oxford University (United Kingdom) conducted a double-blind, randomized study in 24 healthy volunteers on three separate occasions to assess the use of fMRI in obtaining objective outcome measures of drug differentiation. To induce pain, the researchers used capsaicin cream, a topical irritant often used to produce similar characteristics of neuropathic pain on subjects' skin.
Prior to capsaicin cream application, the subjects either received a single dose of gabapentin, which is considered effective and a first line treatment for neuropathic pain; ibuprofen, which is generally not considered an effective treatment for the condition; or a placebo. The researchers then assessed the effect the drugs or placebo had on the brain's neural response to pain using fMRI, in addition to patient-reported pain relief.
The results showed that neural activity was significantly reduced in the subjects who received gabapentin, even with extremely low subject numbers, highlighting the potential for fMRI to make a drug's effect clear in small cohorts, such as during the early stages of human drug development. This ability could provide a much-needed objective method to collect data that could prevent premature discarding of potentially beneficial therapies. The study was published in the January 2106 issue of Anesthesiology.
“Chronic pain is a very common condition. Even the most effective pain medications currently available only provide adequate pain relief, defined as a 50% reduction in pain, in one out of four patients, while some drugs, such as opioids, have significant side effects, including dependence and overuse,” said lead author Vishvarani Wanigasekera, MD, of the University of Oxford. “We believe that neuroimaging techniques, such as fMRI, can provide objective evidence that can be used as outcome measures in early drug development to enhance the efficiency of the drug development process.”
Patient-reported pain relief is the primary outcome measure used in current drug development studies to assess whether medication is effective or not. However, due to their subjective and context-dependent nature, self-reported pain perception and relief are subject to many influences. Due to the low subject population, researchers can also easily miss effective compounds that might work well in the population at large.
Related Links:
John Radcliffe Hospital
Oxford University
Latest MRI News
- Low-Cost Whole-Body MRI Device Combined with AI Generates High-Quality Results
- World's First Whole-Body Ultra-High Field MRI Officially Comes To Market
- World's First Sensor Detects Errors in MRI Scans Using Laser Light and Gas
- Diamond Dust Could Offer New Contrast Agent Option for Future MRI Scans
- Combining MRI with PSA Testing Improves Clinical Outcomes for Prostate Cancer Patients
- PET/MRI Improves Diagnostic Accuracy for Prostate Cancer Patients
- Next Generation MR-Guided Focused Ultrasound Ushers In Future of Incisionless Neurosurgery
- Two-Part MRI Scan Detects Prostate Cancer More Quickly without Compromising Diagnostic Quality
- World’s Most Powerful MRI Machine Images Living Brain with Unrivaled Clarity
- New Whole-Body Imaging Technology Makes It Possible to View Inflammation on MRI Scan
- Combining Prostate MRI with Blood Test Can Avoid Unnecessary Prostate Biopsies
- New Treatment Combines MRI and Ultrasound to Control Prostate Cancer without Serious Side Effects
- MRI Improves Diagnosis and Treatment of Prostate Cancer
- Combined PET-MRI Scan Improves Treatment for Early Breast Cancer Patients
- 4D MRI Could Improve Clinical Assessment of Heart Blood Flow Abnormalities
- MRI-Guided Focused Ultrasound Therapy Shows Promise in Treating Prostate Cancer
Channels
Radiography
view channel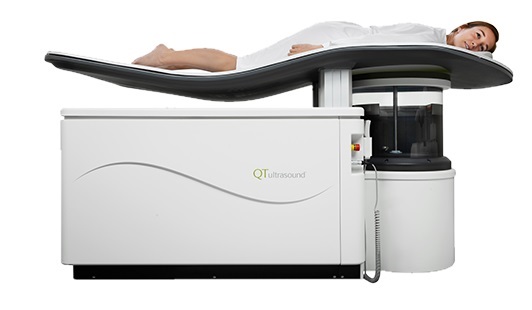
Novel Breast Imaging System Proves As Effective As Mammography
Breast cancer remains the most frequently diagnosed cancer among women. It is projected that one in eight women will be diagnosed with breast cancer during her lifetime, and one in 42 women who turn 50... Read more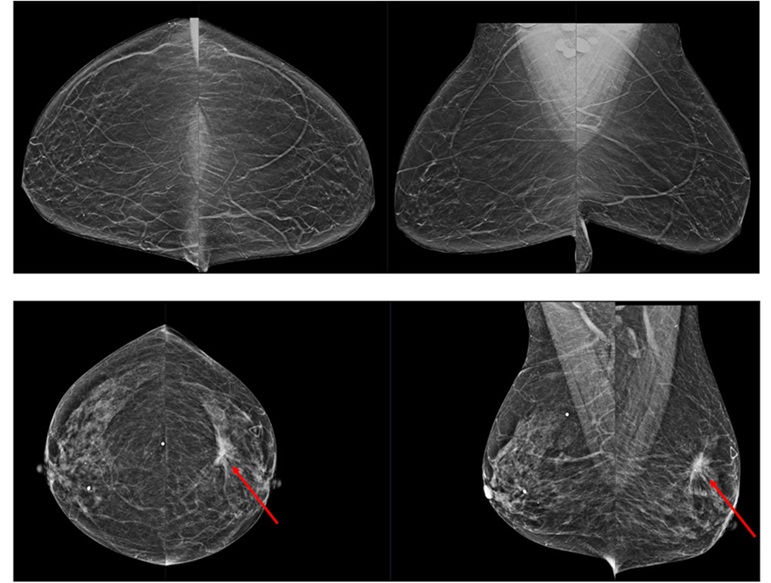
AI Assistance Improves Breast-Cancer Screening by Reducing False Positives
Radiologists typically detect one case of cancer for every 200 mammograms reviewed. However, these evaluations often result in false positives, leading to unnecessary patient recalls for additional testing,... Read moreUltrasound
view channel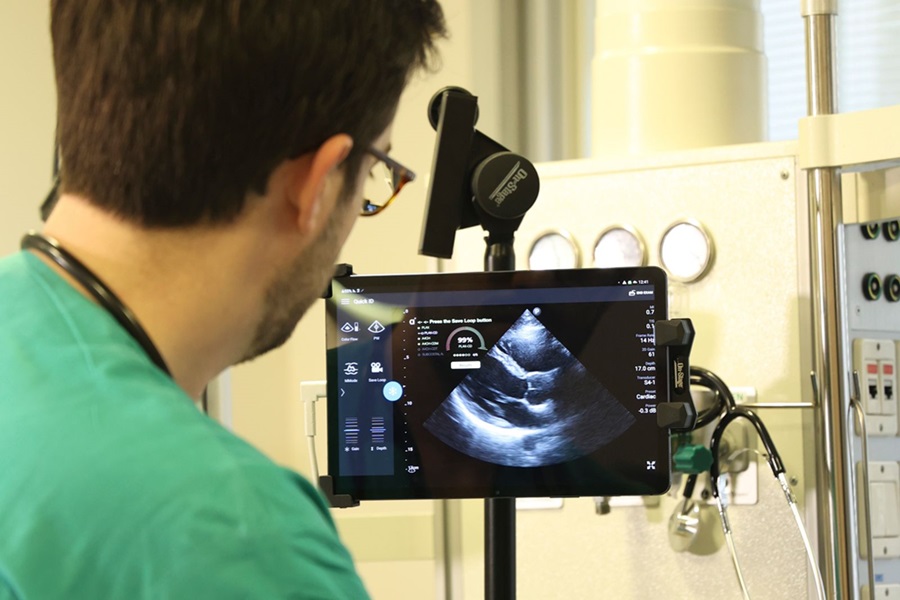
First AI-Powered POC Ultrasound Diagnostic Solution Helps Prioritize Cases Based On Severity
Ultrasound scans are essential for identifying and diagnosing various medical conditions, but often, patients must wait weeks or months for results due to a shortage of qualified medical professionals... Read more
Largest Model Trained On Echocardiography Images Assesses Heart Structure and Function
Foundation models represent an exciting frontier in generative artificial intelligence (AI), yet many lack the specialized medical data needed to make them applicable in healthcare settings.... Read more.jpg)
Groundbreaking Technology Enables Precise, Automatic Measurement of Peripheral Blood Vessels
The current standard of care of using angiographic information is often inadequate for accurately assessing vessel size in the estimated 20 million people in the U.S. who suffer from peripheral vascular disease.... Read moreNuclear Medicine
view channelNew PET Agent Rapidly and Accurately Visualizes Lesions in Clear Cell Renal Cell Carcinoma Patients
Clear cell renal cell cancer (ccRCC) represents 70-80% of renal cell carcinoma cases. While localized disease can be effectively treated with surgery and ablative therapies, one-third of patients either... Read more
New Imaging Technique Monitors Inflammation Disorders without Radiation Exposure
Imaging inflammation using traditional radiological techniques presents significant challenges, including radiation exposure, poor image quality, high costs, and invasive procedures. Now, new contrast... Read more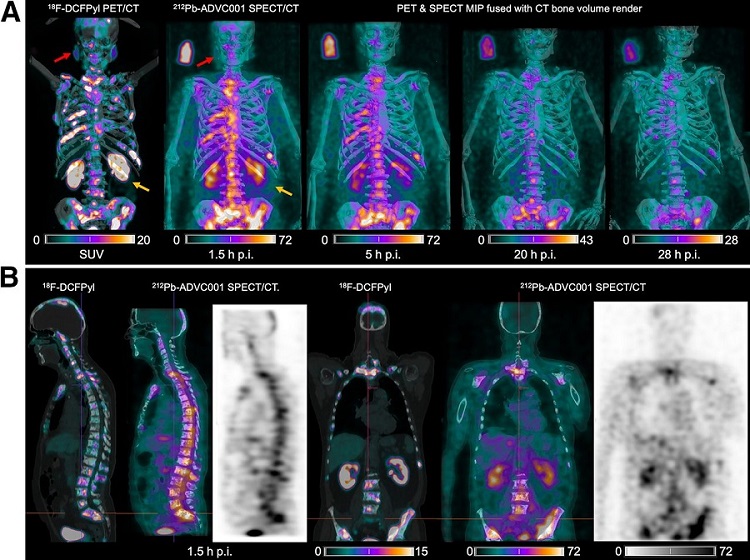
New SPECT/CT Technique Could Change Imaging Practices and Increase Patient Access
The development of lead-212 (212Pb)-PSMA–based targeted alpha therapy (TAT) is garnering significant interest in treating patients with metastatic castration-resistant prostate cancer. The imaging of 212Pb,... Read moreGeneral/Advanced Imaging
view channel
Radiation Therapy Computed Tomography Solution Boosts Imaging Accuracy
One of the most significant challenges in oncology care is disease complexity in terms of the variety of cancer types and the individualized presentation of each patient. This complexity necessitates a... Read more
PET Scans Reveal Hidden Inflammation in Multiple Sclerosis Patients
A key challenge for clinicians treating patients with multiple sclerosis (MS) is that after a certain amount of time, they continue to worsen even though their MRIs show no change. A new study has now... Read moreImaging IT
view channel
New Google Cloud Medical Imaging Suite Makes Imaging Healthcare Data More Accessible
Medical imaging is a critical tool used to diagnose patients, and there are billions of medical images scanned globally each year. Imaging data accounts for about 90% of all healthcare data1 and, until... Read more
Global AI in Medical Diagnostics Market to Be Driven by Demand for Image Recognition in Radiology
The global artificial intelligence (AI) in medical diagnostics market is expanding with early disease detection being one of its key applications and image recognition becoming a compelling consumer proposition... Read moreIndustry News
view channel
Hologic Acquires UK-Based Breast Surgical Guidance Company Endomagnetics Ltd.
Hologic, Inc. (Marlborough, MA, USA) has entered into a definitive agreement to acquire Endomagnetics Ltd. (Cambridge, UK), a privately held developer of breast cancer surgery technologies, for approximately... Read more
Bayer and Google Partner on New AI Product for Radiologists
Medical imaging data comprises around 90% of all healthcare data, and it is a highly complex and rich clinical data modality and serves as a vital tool for diagnosing patients. Each year, billions of medical... Read more