Study Demonstrates Radiation Risk from Digital Screening Mammography Can Be Reduced Further
|
By MedImaging International staff writers Posted on 19 Jan 2016 |
The risk of radiation-induced breast cancer for women undergoing digital screening mammography can be reduced even more for most women by employing simple changes in screening guidelines.
The findings were published in the January 2016, issue of the Annals of Internal Medicine. The research was part of a comprehensive modeling study, undertaken by the UC Davis School of Medicine (Sacramento, CA, USA) that found minimal risk of radiation-induced breast cancer for most women from digital mammography breast cancer screening. Women with large breasts or those with breast implants, often receive extra screening, and have increased radiation exposure. Larger detectors and other new technologies can help mitigate the risk for these women.
The researchers modeled the risk of women developing radiation-induced breast cancer during their lifetime from digital screening mammography, and as a result dying from the disease. The researchers compared this to the number of breast cancer deaths that were prevented by early detection and found that screening 100,000 women aged between 50 and 74, every two years, prevented 627 deaths. The radiation from such exams, and subsequent additional diagnostics, could cause 27 cases of breast cancer, and four deaths. When women aged 40 to 74 were screened every year, an additional 100 radiation-induced breast cancers occurred, and 12 breast cancer deaths, compared to women aged 50 to 74, who were screened every two years.
The results of the study showed screening mammograms taken every two years, instead of yearly, and starting from age 50, not 40 or 45, would be safer for all women.
Diana Miglioretti, first author of the study, and Biostatistics professor at UC Davis School of Medicine, said, “For most women, the risks are very low. The one group I worry about is women with very large breasts who choose to be screened annually from ages 40 to 74. Most screening mammograms are two views per breast. Some women with large breasts need more than four views for a complete screening examination, increasing their exposure to ionizing radiation. In addition, the dose per view increases with compressed breast thickness, further increasing exposure. For the average woman, having an additional workup for an abnormal screening result offers very small additional radiation exposure. But for some women who have additional mammography views and an image-guided biopsy, the additional workup can account for a quarter of their annual radiation exposure from mammography. For the majority of women, screening mammography is very safe. And if you screen every other year between 50 and 74, that makes it safest.”
Related Links:
UC Davis School of Medicine
The findings were published in the January 2016, issue of the Annals of Internal Medicine. The research was part of a comprehensive modeling study, undertaken by the UC Davis School of Medicine (Sacramento, CA, USA) that found minimal risk of radiation-induced breast cancer for most women from digital mammography breast cancer screening. Women with large breasts or those with breast implants, often receive extra screening, and have increased radiation exposure. Larger detectors and other new technologies can help mitigate the risk for these women.
The researchers modeled the risk of women developing radiation-induced breast cancer during their lifetime from digital screening mammography, and as a result dying from the disease. The researchers compared this to the number of breast cancer deaths that were prevented by early detection and found that screening 100,000 women aged between 50 and 74, every two years, prevented 627 deaths. The radiation from such exams, and subsequent additional diagnostics, could cause 27 cases of breast cancer, and four deaths. When women aged 40 to 74 were screened every year, an additional 100 radiation-induced breast cancers occurred, and 12 breast cancer deaths, compared to women aged 50 to 74, who were screened every two years.
The results of the study showed screening mammograms taken every two years, instead of yearly, and starting from age 50, not 40 or 45, would be safer for all women.
Diana Miglioretti, first author of the study, and Biostatistics professor at UC Davis School of Medicine, said, “For most women, the risks are very low. The one group I worry about is women with very large breasts who choose to be screened annually from ages 40 to 74. Most screening mammograms are two views per breast. Some women with large breasts need more than four views for a complete screening examination, increasing their exposure to ionizing radiation. In addition, the dose per view increases with compressed breast thickness, further increasing exposure. For the average woman, having an additional workup for an abnormal screening result offers very small additional radiation exposure. But for some women who have additional mammography views and an image-guided biopsy, the additional workup can account for a quarter of their annual radiation exposure from mammography. For the majority of women, screening mammography is very safe. And if you screen every other year between 50 and 74, that makes it safest.”
Related Links:
UC Davis School of Medicine
Latest Radiography News
- Novel Breast Imaging System Proves As Effective As Mammography
- AI Assistance Improves Breast-Cancer Screening by Reducing False Positives
- AI Could Boost Clinical Adoption of Chest DDR
- 3D Mammography Almost Halves Breast Cancer Incidence between Two Screening Tests
- AI Model Predicts 5-Year Breast Cancer Risk from Mammograms
- Deep Learning Framework Detects Fractures in X-Ray Images With 99% Accuracy
- Direct AI-Based Medical X-Ray Imaging System a Paradigm-Shift from Conventional DR and CT
- Chest X-Ray AI Solution Automatically Identifies, Categorizes and Highlights Suspicious Areas
- AI Diagnoses Wrist Fractures As Well As Radiologists
- Annual Mammography Beginning At 40 Cuts Breast Cancer Mortality By 42%
- 3D Human GPS Powered By Light Paves Way for Radiation-Free Minimally-Invasive Surgery
- Novel AI Technology to Revolutionize Cancer Detection in Dense Breasts
- AI Solution Provides Radiologists with 'Second Pair' Of Eyes to Detect Breast Cancers
- AI Helps General Radiologists Achieve Specialist-Level Performance in Interpreting Mammograms
- Novel Imaging Technique Could Transform Breast Cancer Detection
- Computer Program Combines AI and Heat-Imaging Technology for Early Breast Cancer Detection
Channels
MRI
view channel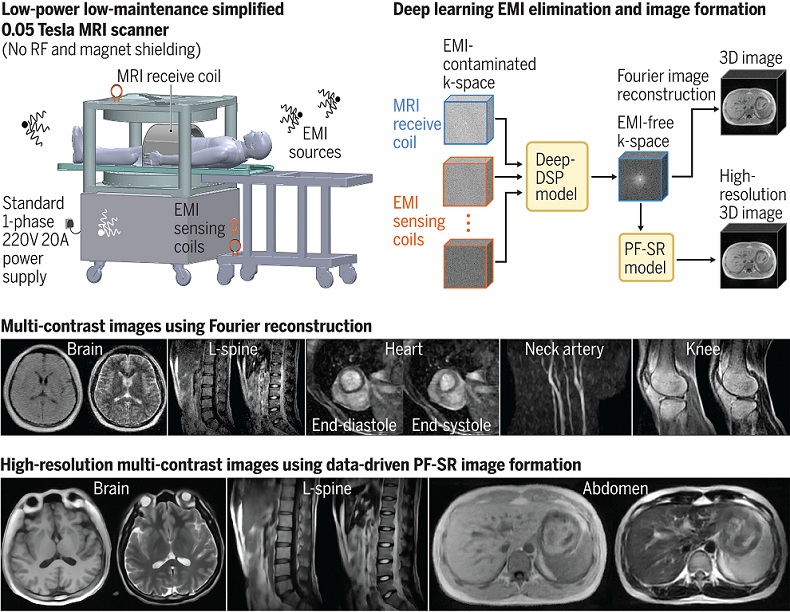
Low-Cost Whole-Body MRI Device Combined with AI Generates High-Quality Results
Magnetic Resonance Imaging (MRI) has significantly transformed healthcare, providing a noninvasive, radiation-free method for detailed imaging. It is especially promising for the future of medical diagnosis... Read more
World's First Whole-Body Ultra-High Field MRI Officially Comes To Market
The world's first whole-body ultra-high field (UHF) MRI has officially come to market, marking a remarkable advancement in diagnostic radiology. United Imaging (Shanghai, China) has secured clearance from the U.... Read moreUltrasound
view channel.jpg)
Diagnostic System Automatically Analyzes TTE Images to Identify Congenital Heart Disease
Congenital heart disease (CHD) is one of the most prevalent congenital anomalies worldwide, presenting substantial health and financial challenges for affected patients. Early detection and treatment of... Read more
Super-Resolution Imaging Technique Could Improve Evaluation of Cardiac Conditions
The heart depends on efficient blood circulation to pump blood throughout the body, delivering oxygen to tissues and removing carbon dioxide and waste. Yet, when heart vessels are damaged, it can disrupt... Read more
First AI-Powered POC Ultrasound Diagnostic Solution Helps Prioritize Cases Based On Severity
Ultrasound scans are essential for identifying and diagnosing various medical conditions, but often, patients must wait weeks or months for results due to a shortage of qualified medical professionals... Read moreNuclear Medicine
view channelNew PET Agent Rapidly and Accurately Visualizes Lesions in Clear Cell Renal Cell Carcinoma Patients
Clear cell renal cell cancer (ccRCC) represents 70-80% of renal cell carcinoma cases. While localized disease can be effectively treated with surgery and ablative therapies, one-third of patients either... Read more
New Imaging Technique Monitors Inflammation Disorders without Radiation Exposure
Imaging inflammation using traditional radiological techniques presents significant challenges, including radiation exposure, poor image quality, high costs, and invasive procedures. Now, new contrast... Read more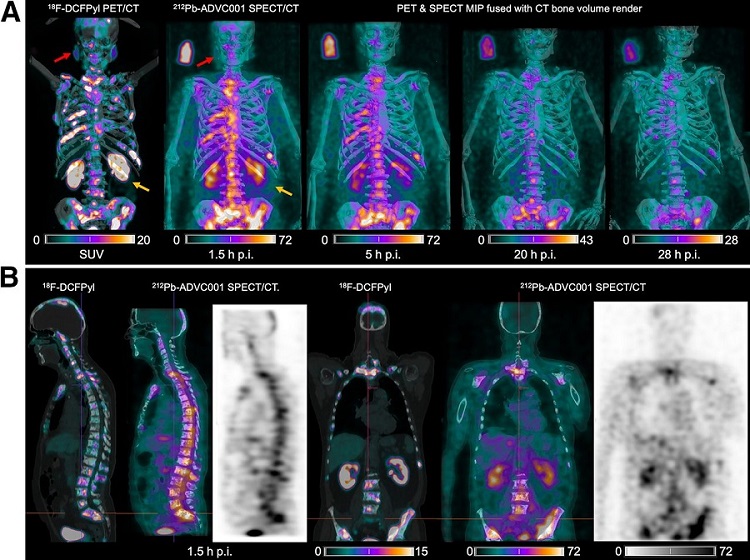
New SPECT/CT Technique Could Change Imaging Practices and Increase Patient Access
The development of lead-212 (212Pb)-PSMA–based targeted alpha therapy (TAT) is garnering significant interest in treating patients with metastatic castration-resistant prostate cancer. The imaging of 212Pb,... Read moreGeneral/Advanced Imaging
view channel
Radiation Therapy Computed Tomography Solution Boosts Imaging Accuracy
One of the most significant challenges in oncology care is disease complexity in terms of the variety of cancer types and the individualized presentation of each patient. This complexity necessitates a... Read more
PET Scans Reveal Hidden Inflammation in Multiple Sclerosis Patients
A key challenge for clinicians treating patients with multiple sclerosis (MS) is that after a certain amount of time, they continue to worsen even though their MRIs show no change. A new study has now... Read moreImaging IT
view channel
New Google Cloud Medical Imaging Suite Makes Imaging Healthcare Data More Accessible
Medical imaging is a critical tool used to diagnose patients, and there are billions of medical images scanned globally each year. Imaging data accounts for about 90% of all healthcare data1 and, until... Read more
Global AI in Medical Diagnostics Market to Be Driven by Demand for Image Recognition in Radiology
The global artificial intelligence (AI) in medical diagnostics market is expanding with early disease detection being one of its key applications and image recognition becoming a compelling consumer proposition... Read moreIndustry News
view channel
Hologic Acquires UK-Based Breast Surgical Guidance Company Endomagnetics Ltd.
Hologic, Inc. (Marlborough, MA, USA) has entered into a definitive agreement to acquire Endomagnetics Ltd. (Cambridge, UK), a privately held developer of breast cancer surgery technologies, for approximately... Read more
Bayer and Google Partner on New AI Product for Radiologists
Medical imaging data comprises around 90% of all healthcare data, and it is a highly complex and rich clinical data modality and serves as a vital tool for diagnosing patients. Each year, billions of medical... Read more