Enhanced Treatment Assessment for Liver Cancer Using New Imaging Analysis Technique
|
By MedImaging International staff writers Posted on 10 Jan 2016 |
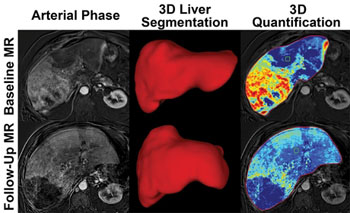
Image: Liver images from before, and after treatment. The bottom-right image shows that less cancer is visible after treatment (Photo courtesy of RSNA).
A study presented at the annual Radiological Society of North America (RSNA 2015) meeting in Chicago USA has shown that a novel MRI analysis technique can significantly speed up the assessment of the effectiveness of liver cancer treatment compared to existing methods.
Hepatocellular Carcinoma (HCC) is the second most deadly cancer worldwide and treatment consists of an image-guided procedure called Transarterial Chemoembolization (TACE). During the procedure chemotherapeutic drugs are delivered to the tumor while at the same time the blood supply to the tumor is blocked. If a patient does not respond to TACE treatment the clinician needs treat them again, or change their therapy, as rapidly as possible. Infiltrative HCC is very difficult to treat after TACE with traditional methods because of the large number of lesions and their ill-defined borders.
The researchers used a new approach developed together with Philips Research North America (Cambridge, MA, USA), called the quantitative European Association for the Study of the Liver (qEASL) technique. The new 3D technology provides whole liver volumetric enhancement quantification on Magnetic Resonance Imaging (MRI) and enables a radiologist to segment and delineate an entire tumor in 15–20 seconds in a semi-automated process. The researchers assessed 68 liver cancer patients with infiltrative HCC, using the qEASL technique, before their first TACE procedure, and again one month after the procedure. The researchers measured treatment response, and predicted survival, and segmented the entire liver of the patients while identifying tumors. The researchers found that responders had an overall survival rate of around 21 months and a mean 57.8% decrease in enhancing volume. Non-responders had a survival rate of 6.8 months and a 19.1% increase enhancing volume on average.
According to the researchers, the qEASL approach can also be used with modalities such as cone-beam Computed Tomography (CT), Multidetector CT (MDCT), and Single-Photon Emission Computed Tomography (SPECT), and has also been validated for benign brain, and uterine lesions, and might also be applicable for systemic therapy.
Coauthor of the study, Julius Chapiro, MD, Yale University School of Medicine, said, "In clinical oncology, it is very challenging to assess tumor response to treatment. Up until now, we could measure the extent of tumor diameter or uptake with manual tools like the caliper on the screen, which are highly unreliable due to reader bias. The radiologist can segment the entire tumor with the assistance of the computer. It's a work-flow efficient, semi-automated process that takes 15 to 20 seconds to segment and allows you to delineate the tumor in 3D. The findings show that quantitative tumor enhancement is possible with 3-D qEASL and can predict survival after TACE for infiltrative and multifocal HCC. qEASL is not a diagnostic tool but rather a means of comparing differences before and after treatment to identify non-responders. The earlier the non-responders are identified and treated, the better their outcomes."
Related Links:
Philips Research North America
Hepatocellular Carcinoma (HCC) is the second most deadly cancer worldwide and treatment consists of an image-guided procedure called Transarterial Chemoembolization (TACE). During the procedure chemotherapeutic drugs are delivered to the tumor while at the same time the blood supply to the tumor is blocked. If a patient does not respond to TACE treatment the clinician needs treat them again, or change their therapy, as rapidly as possible. Infiltrative HCC is very difficult to treat after TACE with traditional methods because of the large number of lesions and their ill-defined borders.
The researchers used a new approach developed together with Philips Research North America (Cambridge, MA, USA), called the quantitative European Association for the Study of the Liver (qEASL) technique. The new 3D technology provides whole liver volumetric enhancement quantification on Magnetic Resonance Imaging (MRI) and enables a radiologist to segment and delineate an entire tumor in 15–20 seconds in a semi-automated process. The researchers assessed 68 liver cancer patients with infiltrative HCC, using the qEASL technique, before their first TACE procedure, and again one month after the procedure. The researchers measured treatment response, and predicted survival, and segmented the entire liver of the patients while identifying tumors. The researchers found that responders had an overall survival rate of around 21 months and a mean 57.8% decrease in enhancing volume. Non-responders had a survival rate of 6.8 months and a 19.1% increase enhancing volume on average.
According to the researchers, the qEASL approach can also be used with modalities such as cone-beam Computed Tomography (CT), Multidetector CT (MDCT), and Single-Photon Emission Computed Tomography (SPECT), and has also been validated for benign brain, and uterine lesions, and might also be applicable for systemic therapy.
Coauthor of the study, Julius Chapiro, MD, Yale University School of Medicine, said, "In clinical oncology, it is very challenging to assess tumor response to treatment. Up until now, we could measure the extent of tumor diameter or uptake with manual tools like the caliper on the screen, which are highly unreliable due to reader bias. The radiologist can segment the entire tumor with the assistance of the computer. It's a work-flow efficient, semi-automated process that takes 15 to 20 seconds to segment and allows you to delineate the tumor in 3D. The findings show that quantitative tumor enhancement is possible with 3-D qEASL and can predict survival after TACE for infiltrative and multifocal HCC. qEASL is not a diagnostic tool but rather a means of comparing differences before and after treatment to identify non-responders. The earlier the non-responders are identified and treated, the better their outcomes."
Related Links:
Philips Research North America
Latest Nuclear Medicine News
- New PET Biomarker Predicts Success of Immune Checkpoint Blockade Therapy
- New PET Agent Rapidly and Accurately Visualizes Lesions in Clear Cell Renal Cell Carcinoma Patients
- New Imaging Technique Monitors Inflammation Disorders without Radiation Exposure
- New SPECT/CT Technique Could Change Imaging Practices and Increase Patient Access
- New Radiotheranostic System Detects and Treats Ovarian Cancer Noninvasively
- AI System Automatically and Reliably Detects Cardiac Amyloidosis Using Scintigraphy Imaging
- Early 30-Minute Dynamic FDG-PET Acquisition Could Halve Lung Scan Times
- New Method for Triggering and Imaging Seizures to Help Guide Epilepsy Surgery
- Radioguided Surgery Accurately Detects and Removes Metastatic Lymph Nodes in Prostate Cancer Patients
- New PET Tracer Detects Inflammatory Arthritis Before Symptoms Appear
- Novel PET Tracer Enhances Lesion Detection in Medullary Thyroid Cancer
- Targeted Therapy Delivers Radiation Directly To Cells in Hard-To-Treat Cancers
- New PET Tracer Noninvasively Identifies Cancer Gene Mutation for More Precise Diagnosis
- Algorithm Predicts Prostate Cancer Recurrence in Patients Treated by Radiation Therapy
- Novel PET Imaging Tracer Noninvasively Identifies Cancer Gene Mutation for More Precise Diagnosis
- Ultrafast Laser Technology to Improve Cancer Treatment
Channels
Radiography
view channel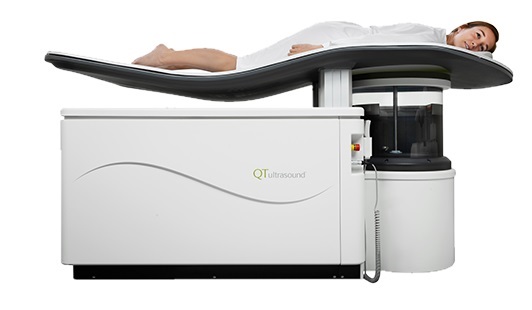
Novel Breast Imaging System Proves As Effective As Mammography
Breast cancer remains the most frequently diagnosed cancer among women. It is projected that one in eight women will be diagnosed with breast cancer during her lifetime, and one in 42 women who turn 50... Read more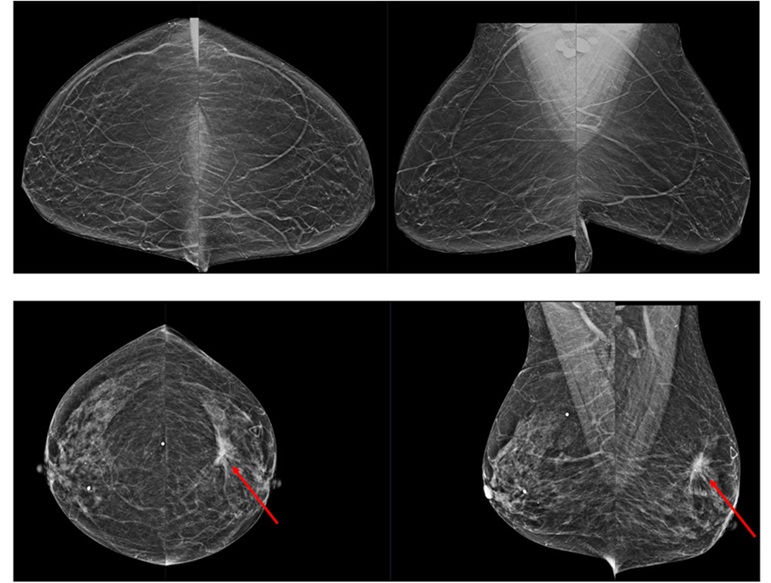
AI Assistance Improves Breast-Cancer Screening by Reducing False Positives
Radiologists typically detect one case of cancer for every 200 mammograms reviewed. However, these evaluations often result in false positives, leading to unnecessary patient recalls for additional testing,... Read moreMRI
view channel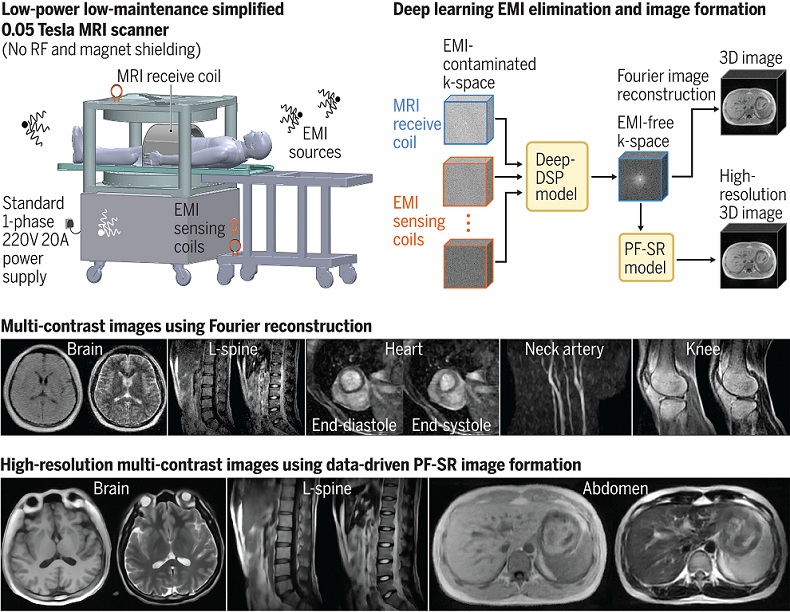
Low-Cost Whole-Body MRI Device Combined with AI Generates High-Quality Results
Magnetic Resonance Imaging (MRI) has significantly transformed healthcare, providing a noninvasive, radiation-free method for detailed imaging. It is especially promising for the future of medical diagnosis... Read more
World's First Whole-Body Ultra-High Field MRI Officially Comes To Market
The world's first whole-body ultra-high field (UHF) MRI has officially come to market, marking a remarkable advancement in diagnostic radiology. United Imaging (Shanghai, China) has secured clearance from the U.... Read moreUltrasound
view channel.jpg)
Diagnostic System Automatically Analyzes TTE Images to Identify Congenital Heart Disease
Congenital heart disease (CHD) is one of the most prevalent congenital anomalies worldwide, presenting substantial health and financial challenges for affected patients. Early detection and treatment of... Read more
Super-Resolution Imaging Technique Could Improve Evaluation of Cardiac Conditions
The heart depends on efficient blood circulation to pump blood throughout the body, delivering oxygen to tissues and removing carbon dioxide and waste. Yet, when heart vessels are damaged, it can disrupt... Read more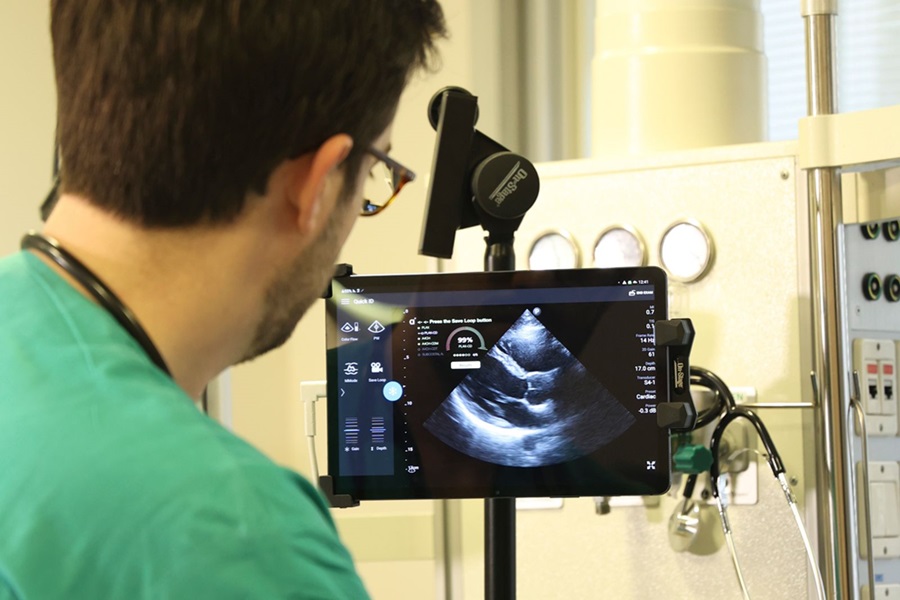
First AI-Powered POC Ultrasound Diagnostic Solution Helps Prioritize Cases Based On Severity
Ultrasound scans are essential for identifying and diagnosing various medical conditions, but often, patients must wait weeks or months for results due to a shortage of qualified medical professionals... Read moreNuclear Medicine
view channel
New PET Biomarker Predicts Success of Immune Checkpoint Blockade Therapy
Immunotherapies, such as immune checkpoint blockade (ICB), have shown promising clinical results in treating melanoma, non-small cell lung cancer, and other tumor types. However, the effectiveness of these... Read moreNew PET Agent Rapidly and Accurately Visualizes Lesions in Clear Cell Renal Cell Carcinoma Patients
Clear cell renal cell cancer (ccRCC) represents 70-80% of renal cell carcinoma cases. While localized disease can be effectively treated with surgery and ablative therapies, one-third of patients either... Read more
New Imaging Technique Monitors Inflammation Disorders without Radiation Exposure
Imaging inflammation using traditional radiological techniques presents significant challenges, including radiation exposure, poor image quality, high costs, and invasive procedures. Now, new contrast... Read more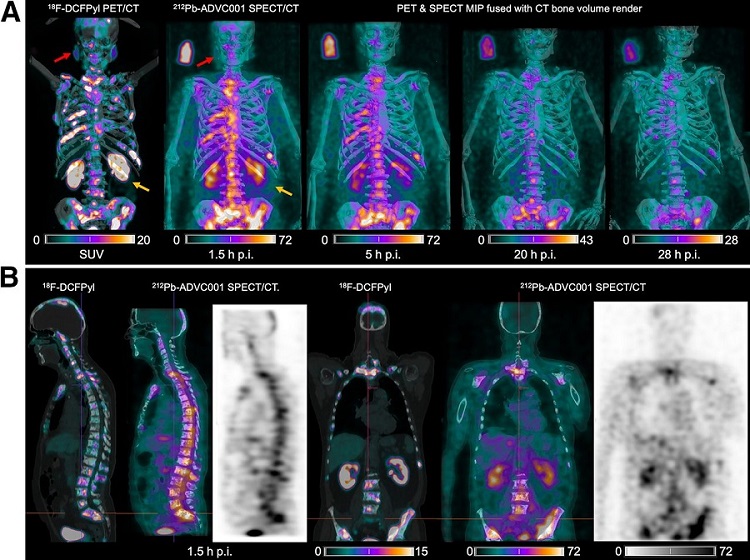
New SPECT/CT Technique Could Change Imaging Practices and Increase Patient Access
The development of lead-212 (212Pb)-PSMA–based targeted alpha therapy (TAT) is garnering significant interest in treating patients with metastatic castration-resistant prostate cancer. The imaging of 212Pb,... Read moreImaging IT
view channel
New Google Cloud Medical Imaging Suite Makes Imaging Healthcare Data More Accessible
Medical imaging is a critical tool used to diagnose patients, and there are billions of medical images scanned globally each year. Imaging data accounts for about 90% of all healthcare data1 and, until... Read more
Global AI in Medical Diagnostics Market to Be Driven by Demand for Image Recognition in Radiology
The global artificial intelligence (AI) in medical diagnostics market is expanding with early disease detection being one of its key applications and image recognition becoming a compelling consumer proposition... Read moreIndustry News
view channel
Hologic Acquires UK-Based Breast Surgical Guidance Company Endomagnetics Ltd.
Hologic, Inc. (Marlborough, MA, USA) has entered into a definitive agreement to acquire Endomagnetics Ltd. (Cambridge, UK), a privately held developer of breast cancer surgery technologies, for approximately... Read more
Bayer and Google Partner on New AI Product for Radiologists
Medical imaging data comprises around 90% of all healthcare data, and it is a highly complex and rich clinical data modality and serves as a vital tool for diagnosing patients. Each year, billions of medical... Read more