Reprogramming Stem Cells May Suppress Cancer after Radiotherapy
|
By MedImaging International staff writers Posted on 27 Jan 2015 |
The body has developed strategies of purging defective stem cells. A new study has revealed that one of these ways is a “program” that makes stem cells damaged by radiation differentiate into other cells that can no longer survive forever.
Radiation makes a stem cell lose its “stemness,” which makes sense because damaged stem cells do not need to hang around to pump out damaged cells. Moreover, the research, conducted by University of Colorado (CU) Cancer Center (Aurora, USA) scientists, and published online December 27, 2014, in the journal Stem Cells, demonstrated that this same protection of “programmed mediocrity” that rids stem cells damaged by radiation allows blood cancers to grow in instances when the total body is irradiated. Furthermore, by reprogramming this defense, cancer may be prevented in the aftermath of full body radiation. “The body didn’t evolve to deal with leaking nuclear reactors and CT scans. It evolved to deal with only a few cells at a time receiving dangerous doses of radiation or other insults to their DNA,” said James DeGregori, PhD, investigator at the CU Cancer Center, professor of biochemistry and molecular genetics at the CU School of Medicine, and the article’s senior author.
Dr. DeGregori, doctoral student Courtney Fleenor, and colleagues examined the effects of full body radiation on the blood stem cells of mice. In this case, radiation increased the probability that cells in the hematopoietic stem cell system would differentiate. Only, while most obeyed this instruction, a few did not. Stem cells with a very specific mutation were able to disobey the instruction to differentiate and retain their “stemness.” Genetic inhibition of the gene C/EBPA allowed a few stem cells to keep the ability to act as stem cells. With competition from other, healthy stem cells removed, the stem cells with reduced C/EBPA were able to dominate the blood cell production system. In this way, the blood system transitioned from C/EBPA+ cells to primarily C/EBPA- cells.
Mutations and other genetic alterations resulting in inhibition of the C/EBPA gene are associated with acute myeloid leukemia in humans. Thus, it's not mutations caused by radiation but a blood system reengineered by faulty stem cells that creates cancer risk in people who have experienced radiation. “It’s about evolution driven by natural selection,” Dr. DeGregori noted. “In a healthy blood system, healthy stem cells out-compete stem cells that happen to have the C/EBPA mutation. But when radiation reduces the heath and robustness of the stem cell population, the mutated cells that have been there all along are suddenly given the opportunity to take over.”
These studies do not only clarify why radiation makes hematopoietic stem cells (HSCs) differentiate; they also show that by activating a stem cell maintenance pathway, we can keep it from happening. Even months after irradiation, artificially activating the NOTCH signaling pathway of irradiated HSCs lets them act “stemmy” again—restarting the blood cell assembly line in these HSCs that would have otherwise differentiated in response to radiation.
When Drs. DeGregori, Fleenor and colleagues triggered NOTCH in earlier irradiated HSCs, it kept the population of dangerous, C/EBPA cells at bay. Competition from non-C/EBPA-mutant stem cells, with their health restored by NOTCH activation, meant that there was no evolutionary space for C/EBPA-mutant stem cells.
“If I were working in a situation in which I was likely to experience full-body radiation, I would freeze a bunch of my HSCs,” Dr. DeGregori stated, explaining that an infusion of healthy HSCs after radiation exposure would likely allow the healthy blood system to out-compete the radiation-exposed HSC with their ‘programmed mediocrity’ [increased differentiation] and even HSC with cancer-causing mutations. “But there’s also hope that in the future, we could offer drugs that would restore the fitness of stem cells left over after radiation.”
Related Links:
University of Colorado Cancer Center
Radiation makes a stem cell lose its “stemness,” which makes sense because damaged stem cells do not need to hang around to pump out damaged cells. Moreover, the research, conducted by University of Colorado (CU) Cancer Center (Aurora, USA) scientists, and published online December 27, 2014, in the journal Stem Cells, demonstrated that this same protection of “programmed mediocrity” that rids stem cells damaged by radiation allows blood cancers to grow in instances when the total body is irradiated. Furthermore, by reprogramming this defense, cancer may be prevented in the aftermath of full body radiation. “The body didn’t evolve to deal with leaking nuclear reactors and CT scans. It evolved to deal with only a few cells at a time receiving dangerous doses of radiation or other insults to their DNA,” said James DeGregori, PhD, investigator at the CU Cancer Center, professor of biochemistry and molecular genetics at the CU School of Medicine, and the article’s senior author.
Dr. DeGregori, doctoral student Courtney Fleenor, and colleagues examined the effects of full body radiation on the blood stem cells of mice. In this case, radiation increased the probability that cells in the hematopoietic stem cell system would differentiate. Only, while most obeyed this instruction, a few did not. Stem cells with a very specific mutation were able to disobey the instruction to differentiate and retain their “stemness.” Genetic inhibition of the gene C/EBPA allowed a few stem cells to keep the ability to act as stem cells. With competition from other, healthy stem cells removed, the stem cells with reduced C/EBPA were able to dominate the blood cell production system. In this way, the blood system transitioned from C/EBPA+ cells to primarily C/EBPA- cells.
Mutations and other genetic alterations resulting in inhibition of the C/EBPA gene are associated with acute myeloid leukemia in humans. Thus, it's not mutations caused by radiation but a blood system reengineered by faulty stem cells that creates cancer risk in people who have experienced radiation. “It’s about evolution driven by natural selection,” Dr. DeGregori noted. “In a healthy blood system, healthy stem cells out-compete stem cells that happen to have the C/EBPA mutation. But when radiation reduces the heath and robustness of the stem cell population, the mutated cells that have been there all along are suddenly given the opportunity to take over.”
These studies do not only clarify why radiation makes hematopoietic stem cells (HSCs) differentiate; they also show that by activating a stem cell maintenance pathway, we can keep it from happening. Even months after irradiation, artificially activating the NOTCH signaling pathway of irradiated HSCs lets them act “stemmy” again—restarting the blood cell assembly line in these HSCs that would have otherwise differentiated in response to radiation.
When Drs. DeGregori, Fleenor and colleagues triggered NOTCH in earlier irradiated HSCs, it kept the population of dangerous, C/EBPA cells at bay. Competition from non-C/EBPA-mutant stem cells, with their health restored by NOTCH activation, meant that there was no evolutionary space for C/EBPA-mutant stem cells.
“If I were working in a situation in which I was likely to experience full-body radiation, I would freeze a bunch of my HSCs,” Dr. DeGregori stated, explaining that an infusion of healthy HSCs after radiation exposure would likely allow the healthy blood system to out-compete the radiation-exposed HSC with their ‘programmed mediocrity’ [increased differentiation] and even HSC with cancer-causing mutations. “But there’s also hope that in the future, we could offer drugs that would restore the fitness of stem cells left over after radiation.”
Related Links:
University of Colorado Cancer Center
Latest Radiography News
- Novel Breast Imaging System Proves As Effective As Mammography
- AI Assistance Improves Breast-Cancer Screening by Reducing False Positives
- AI Could Boost Clinical Adoption of Chest DDR
- 3D Mammography Almost Halves Breast Cancer Incidence between Two Screening Tests
- AI Model Predicts 5-Year Breast Cancer Risk from Mammograms
- Deep Learning Framework Detects Fractures in X-Ray Images With 99% Accuracy
- Direct AI-Based Medical X-Ray Imaging System a Paradigm-Shift from Conventional DR and CT
- Chest X-Ray AI Solution Automatically Identifies, Categorizes and Highlights Suspicious Areas
- AI Diagnoses Wrist Fractures As Well As Radiologists
- Annual Mammography Beginning At 40 Cuts Breast Cancer Mortality By 42%
- 3D Human GPS Powered By Light Paves Way for Radiation-Free Minimally-Invasive Surgery
- Novel AI Technology to Revolutionize Cancer Detection in Dense Breasts
- AI Solution Provides Radiologists with 'Second Pair' Of Eyes to Detect Breast Cancers
- AI Helps General Radiologists Achieve Specialist-Level Performance in Interpreting Mammograms
- Novel Imaging Technique Could Transform Breast Cancer Detection
- Computer Program Combines AI and Heat-Imaging Technology for Early Breast Cancer Detection
Channels
MRI
view channel
World's First Whole-Body Ultra-High Field MRI Officially Comes To Market
The world's first whole-body ultra-high field (UHF) MRI has officially come to market, marking a remarkable advancement in diagnostic radiology. United Imaging (Shanghai, China) has secured clearance from the U.... Read more
World's First Sensor Detects Errors in MRI Scans Using Laser Light and Gas
MRI scanners are daily tools for doctors and healthcare professionals, providing unparalleled 3D imaging of the brain, vital organs, and soft tissues, far surpassing other imaging technologies in quality.... Read more
Diamond Dust Could Offer New Contrast Agent Option for Future MRI Scans
Gadolinium, a heavy metal used for over three decades as a contrast agent in medical imaging, enhances the clarity of MRI scans by highlighting affected areas. Despite its utility, gadolinium not only... Read more.jpg)
Combining MRI with PSA Testing Improves Clinical Outcomes for Prostate Cancer Patients
Prostate cancer is a leading health concern globally, consistently being one of the most common types of cancer among men and a major cause of cancer-related deaths. In the United States, it is the most... Read moreUltrasound
view channel
First AI-Powered POC Ultrasound Diagnostic Solution Helps Prioritize Cases Based On Severity
Ultrasound scans are essential for identifying and diagnosing various medical conditions, but often, patients must wait weeks or months for results due to a shortage of qualified medical professionals... Read more
Largest Model Trained On Echocardiography Images Assesses Heart Structure and Function
Foundation models represent an exciting frontier in generative artificial intelligence (AI), yet many lack the specialized medical data needed to make them applicable in healthcare settings.... Read more.jpg)
Groundbreaking Technology Enables Precise, Automatic Measurement of Peripheral Blood Vessels
The current standard of care of using angiographic information is often inadequate for accurately assessing vessel size in the estimated 20 million people in the U.S. who suffer from peripheral vascular disease.... Read moreNuclear Medicine
view channelNew PET Agent Rapidly and Accurately Visualizes Lesions in Clear Cell Renal Cell Carcinoma Patients
Clear cell renal cell cancer (ccRCC) represents 70-80% of renal cell carcinoma cases. While localized disease can be effectively treated with surgery and ablative therapies, one-third of patients either... Read more
New Imaging Technique Monitors Inflammation Disorders without Radiation Exposure
Imaging inflammation using traditional radiological techniques presents significant challenges, including radiation exposure, poor image quality, high costs, and invasive procedures. Now, new contrast... Read more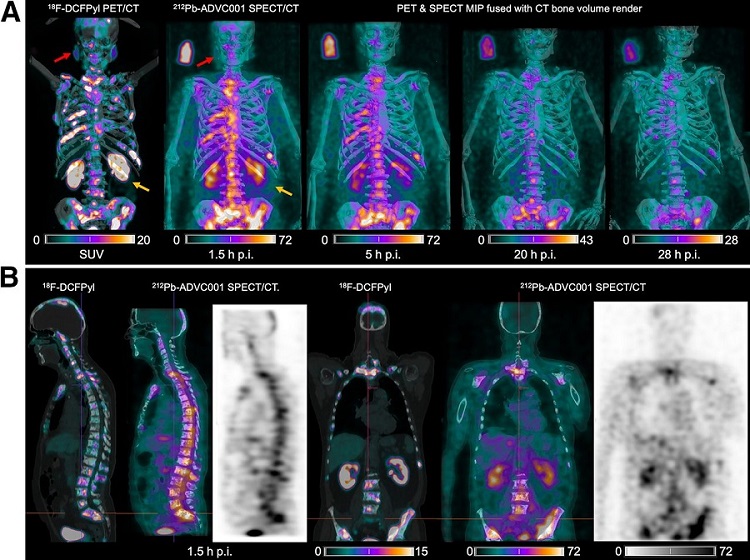
New SPECT/CT Technique Could Change Imaging Practices and Increase Patient Access
The development of lead-212 (212Pb)-PSMA–based targeted alpha therapy (TAT) is garnering significant interest in treating patients with metastatic castration-resistant prostate cancer. The imaging of 212Pb,... Read moreGeneral/Advanced Imaging
view channel
Radiation Therapy Computed Tomography Solution Boosts Imaging Accuracy
One of the most significant challenges in oncology care is disease complexity in terms of the variety of cancer types and the individualized presentation of each patient. This complexity necessitates a... Read more
PET Scans Reveal Hidden Inflammation in Multiple Sclerosis Patients
A key challenge for clinicians treating patients with multiple sclerosis (MS) is that after a certain amount of time, they continue to worsen even though their MRIs show no change. A new study has now... Read moreImaging IT
view channel
New Google Cloud Medical Imaging Suite Makes Imaging Healthcare Data More Accessible
Medical imaging is a critical tool used to diagnose patients, and there are billions of medical images scanned globally each year. Imaging data accounts for about 90% of all healthcare data1 and, until... Read more
Global AI in Medical Diagnostics Market to Be Driven by Demand for Image Recognition in Radiology
The global artificial intelligence (AI) in medical diagnostics market is expanding with early disease detection being one of its key applications and image recognition becoming a compelling consumer proposition... Read moreIndustry News
view channel
Hologic Acquires UK-Based Breast Surgical Guidance Company Endomagnetics Ltd.
Hologic, Inc. (Marlborough, MA, USA) has entered into a definitive agreement to acquire Endomagnetics Ltd. (Cambridge, UK), a privately held developer of breast cancer surgery technologies, for approximately... Read more
Bayer and Google Partner on New AI Product for Radiologists
Medical imaging data comprises around 90% of all healthcare data, and it is a highly complex and rich clinical data modality and serves as a vital tool for diagnosing patients. Each year, billions of medical... Read more