Lymph Node Ultrasound Imaging Most Effective for Obese Breast Cancer Patients
|
By MedImaging International staff writers Posted on 14 May 2014 |
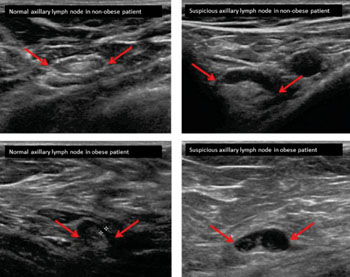
Image: Ultrasound imaging used to identify breast cancer in underarm lymph nodes in obese women has generated an unexpected finding: Fat did not obscure the images, and ultrasound imaging showing no suspicious lymph nodes actually was shown to be more accurate in overweight and obese patients than in women with a normal body mass index (Photo courtesy of the Mayo Clinic).
New research into whether ultrasound imaging used to identify breast cancer in underarm lymph nodes is less effective in obese women, has generated an unexpected finding. Fat did not obscure the images and ultrasound imaging showing no suspicious lymph nodes actually was shown to be more accurate in overweight and obese patients than in women with a normal body mass index.
The research was among several Mayo Clinic (Rochester, MN, USA) studies presented at the American Society of Breast Surgeons annual meeting, held April 30–May 4, 2014, in Las Vegas (NV, USA).
Researchers studied 1,331 breast cancer patients who received ultrasounds of their axillary lymph nodes, the lymph nodes in the armpits, to check for cancer before surgery. Of those patients, 36% were considered obese, with a body mass index of 30 or more. Body mass index is a formula that uses weight and height to estimate body fat. Of the other women evaluated, 33% were of normal weight and 31% were overweight but not obese.
Obesity can change lymph nodes, including the way they look in imaging studies, and make physical exam of underarm lymph nodes more challenging. The Mayo study discovered that higher body weight did not cloud ultrasound images of the axillary lymph nodes in overweight or obese cancer patients, and that their ultrasound scans had better specificity and accuracy than those of thinner women, meaning that when ultrasound showed no suspicious lymph nodes, it was likelier to be correct. “I think we were surprised at these results,” noted senior author Tina Hieken, MD, a breast cancer surgeon at Mayo Clinic. “It should be very reassuring that regardless of the weight of the patient, axillary ultrasound is helpful.”
Potential reasons for the findings, Dr. Hieken hypothesizes: Soft fatty tissue can be compressed during ultrasound scanning, and physicians now have more experience in knowing what lymph nodes may look like in overweight and obese patients. In some thin patients, ultrasounds may not yield as much information because underarm lymph nodes can be so close to the surface, it may be difficult to get good images, she reported.
Surgeons do not rely on ultrasound by itself to determine whether or not breast cancer has spread; it is one of several sources of information used to guide treatment. “For most patients with invasive breast cancer, if the axillary ultrasound is negative, we perform a sentinel lymph node biopsy at the time of the breast operation to make sure cancer has not spread. When the preoperative axillary ultrasound shows suspicious lymph nodes, we then do a fine-needle aspiration of the lymph nodes. If that shows cancer, we may discuss other strategies with the patient such as giving chemotherapy before surgery,” Dr. Hieken said.
More research is planned, including evaluating at different techniques of lymph node ultrasound to improve accuracy and perhaps to avoid axillary lymph node surgery altogether in some breast cancer patients with small tumors and negative axillary ultrasounds, Dr. Hieken reported.
Related Links:
Mayo Clinic
The research was among several Mayo Clinic (Rochester, MN, USA) studies presented at the American Society of Breast Surgeons annual meeting, held April 30–May 4, 2014, in Las Vegas (NV, USA).
Researchers studied 1,331 breast cancer patients who received ultrasounds of their axillary lymph nodes, the lymph nodes in the armpits, to check for cancer before surgery. Of those patients, 36% were considered obese, with a body mass index of 30 or more. Body mass index is a formula that uses weight and height to estimate body fat. Of the other women evaluated, 33% were of normal weight and 31% were overweight but not obese.
Obesity can change lymph nodes, including the way they look in imaging studies, and make physical exam of underarm lymph nodes more challenging. The Mayo study discovered that higher body weight did not cloud ultrasound images of the axillary lymph nodes in overweight or obese cancer patients, and that their ultrasound scans had better specificity and accuracy than those of thinner women, meaning that when ultrasound showed no suspicious lymph nodes, it was likelier to be correct. “I think we were surprised at these results,” noted senior author Tina Hieken, MD, a breast cancer surgeon at Mayo Clinic. “It should be very reassuring that regardless of the weight of the patient, axillary ultrasound is helpful.”
Potential reasons for the findings, Dr. Hieken hypothesizes: Soft fatty tissue can be compressed during ultrasound scanning, and physicians now have more experience in knowing what lymph nodes may look like in overweight and obese patients. In some thin patients, ultrasounds may not yield as much information because underarm lymph nodes can be so close to the surface, it may be difficult to get good images, she reported.
Surgeons do not rely on ultrasound by itself to determine whether or not breast cancer has spread; it is one of several sources of information used to guide treatment. “For most patients with invasive breast cancer, if the axillary ultrasound is negative, we perform a sentinel lymph node biopsy at the time of the breast operation to make sure cancer has not spread. When the preoperative axillary ultrasound shows suspicious lymph nodes, we then do a fine-needle aspiration of the lymph nodes. If that shows cancer, we may discuss other strategies with the patient such as giving chemotherapy before surgery,” Dr. Hieken said.
More research is planned, including evaluating at different techniques of lymph node ultrasound to improve accuracy and perhaps to avoid axillary lymph node surgery altogether in some breast cancer patients with small tumors and negative axillary ultrasounds, Dr. Hieken reported.
Related Links:
Mayo Clinic
Latest Ultrasound News
- Diagnostic System Automatically Analyzes TTE Images to Identify Congenital Heart Disease
- Super-Resolution Imaging Technique Could Improve Evaluation of Cardiac Conditions

- First AI-Powered POC Ultrasound Diagnostic Solution Helps Prioritize Cases Based On Severity

- Largest Model Trained On Echocardiography Images Assesses Heart Structure and Function
- Groundbreaking Technology Enables Precise, Automatic Measurement of Peripheral Blood Vessels
- Deep Learning Advances Super-Resolution Ultrasound Imaging
- Novel Ultrasound-Launched Targeted Nanoparticle Eliminates Biofilm and Bacterial Infection
- AI-Guided Ultrasound System Enables Rapid Assessments of DVT
- Focused Ultrasound Technique Gets Quality Assurance Protocol
- AI-Guided Handheld Ultrasound System Helps Capture Diagnostic-Quality Cardiac Images
- Non-Invasive Ultrasound Imaging Device Diagnoses Risk of Chronic Kidney Disease
- Wearable Ultrasound Platform Paves Way for 24/7 Blood Pressure Monitoring On the Wrist
- Diagnostic Ultrasound Enhancing Agent to Improve Image Quality in Pediatric Heart Patients
- AI Detects COVID-19 in Lung Ultrasound Images
- New Ultrasound Technology to Revolutionize Respiratory Disease Diagnoses
- Dynamic Contrast-Enhanced Ultrasound Highly Useful For Interventions
Channels
Radiography
view channel
Novel Breast Imaging System Proves As Effective As Mammography
Breast cancer remains the most frequently diagnosed cancer among women. It is projected that one in eight women will be diagnosed with breast cancer during her lifetime, and one in 42 women who turn 50... Read more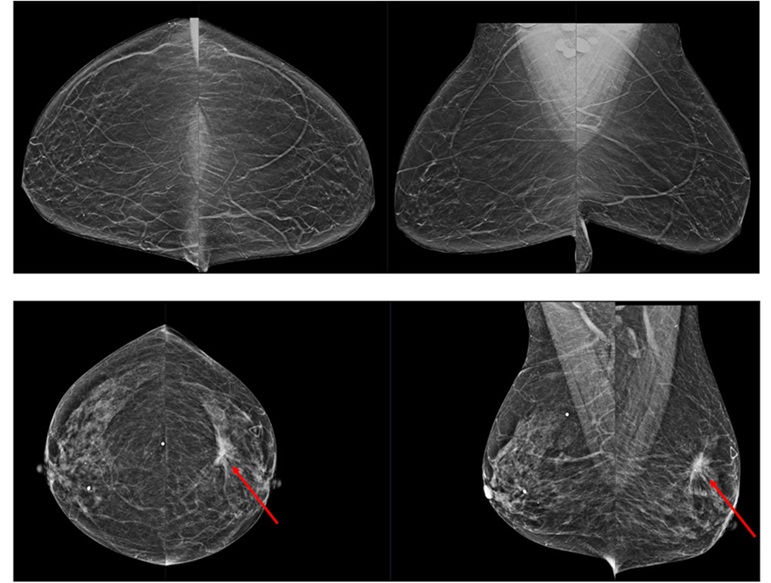
AI Assistance Improves Breast-Cancer Screening by Reducing False Positives
Radiologists typically detect one case of cancer for every 200 mammograms reviewed. However, these evaluations often result in false positives, leading to unnecessary patient recalls for additional testing,... Read moreMRI
view channel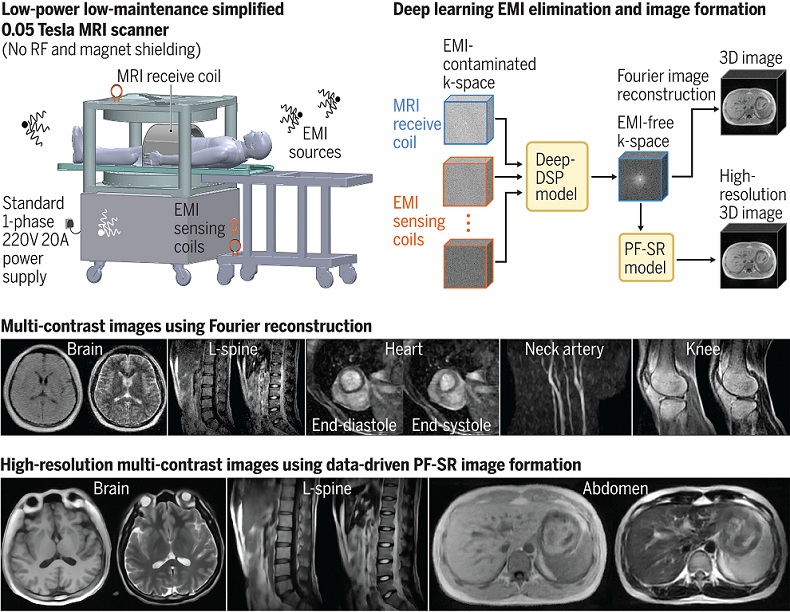
Low-Cost Whole-Body MRI Device Combined with AI Generates High-Quality Results
Magnetic Resonance Imaging (MRI) has significantly transformed healthcare, providing a noninvasive, radiation-free method for detailed imaging. It is especially promising for the future of medical diagnosis... Read more
World's First Whole-Body Ultra-High Field MRI Officially Comes To Market
The world's first whole-body ultra-high field (UHF) MRI has officially come to market, marking a remarkable advancement in diagnostic radiology. United Imaging (Shanghai, China) has secured clearance from the U.... Read moreNuclear Medicine
view channel
New PET Biomarker Predicts Success of Immune Checkpoint Blockade Therapy
Immunotherapies, such as immune checkpoint blockade (ICB), have shown promising clinical results in treating melanoma, non-small cell lung cancer, and other tumor types. However, the effectiveness of these... Read moreNew PET Agent Rapidly and Accurately Visualizes Lesions in Clear Cell Renal Cell Carcinoma Patients
Clear cell renal cell cancer (ccRCC) represents 70-80% of renal cell carcinoma cases. While localized disease can be effectively treated with surgery and ablative therapies, one-third of patients either... Read more
New Imaging Technique Monitors Inflammation Disorders without Radiation Exposure
Imaging inflammation using traditional radiological techniques presents significant challenges, including radiation exposure, poor image quality, high costs, and invasive procedures. Now, new contrast... Read more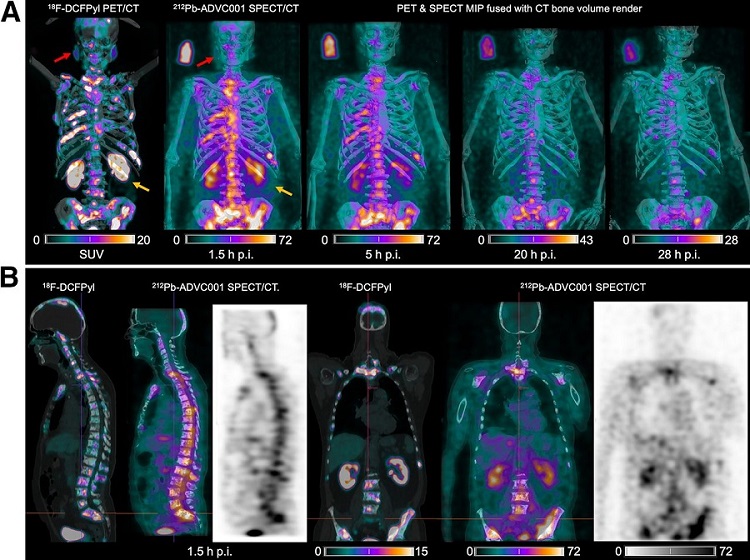
New SPECT/CT Technique Could Change Imaging Practices and Increase Patient Access
The development of lead-212 (212Pb)-PSMA–based targeted alpha therapy (TAT) is garnering significant interest in treating patients with metastatic castration-resistant prostate cancer. The imaging of 212Pb,... Read moreGeneral/Advanced Imaging
view channelBone Density Test Uses Existing CT Images to Predict Fractures
Osteoporotic fractures are not only devastating and deadly, especially hip fractures, but also impose significant costs. They rank among the top chronic diseases in terms of disability-adjusted life years... Read more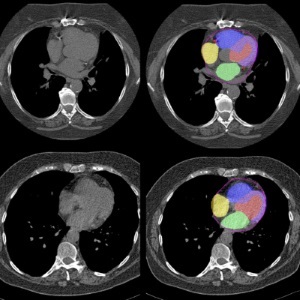
AI Predicts Cardiac Risk and Mortality from Routine Chest CT Scans
Heart disease remains the leading cause of death and is largely preventable, yet many individuals are unaware of their risk until it becomes severe. Early detection through screening can reveal heart issues,... Read moreImaging IT
view channel
New Google Cloud Medical Imaging Suite Makes Imaging Healthcare Data More Accessible
Medical imaging is a critical tool used to diagnose patients, and there are billions of medical images scanned globally each year. Imaging data accounts for about 90% of all healthcare data1 and, until... Read more
Global AI in Medical Diagnostics Market to Be Driven by Demand for Image Recognition in Radiology
The global artificial intelligence (AI) in medical diagnostics market is expanding with early disease detection being one of its key applications and image recognition becoming a compelling consumer proposition... Read moreIndustry News
view channel
Hologic Acquires UK-Based Breast Surgical Guidance Company Endomagnetics Ltd.
Hologic, Inc. (Marlborough, MA, USA) has entered into a definitive agreement to acquire Endomagnetics Ltd. (Cambridge, UK), a privately held developer of breast cancer surgery technologies, for approximately... Read more
Bayer and Google Partner on New AI Product for Radiologists
Medical imaging data comprises around 90% of all healthcare data, and it is a highly complex and rich clinical data modality and serves as a vital tool for diagnosing patients. Each year, billions of medical... Read more