Researchers Develop AI Model to Make Cancer Treatment Less Toxic
|
By MedImaging International staff writers Posted on 20 Aug 2018 |
Image: Researchers aim to improve the quality of life for patients suffering from glioblastoma with a machine-learning model that makes chemotherapy and radiotherapy dosing regimens less toxic but still as effective as human-designed regimens (Photo courtesy of MIT).
Researchers from the Massachusetts Institute of Technology (Cambridge, MA, USA) have developed an artificial intelligence model that “learns” from patient data to make cancer-dosing regimens less toxic but still effective.
In a paper presented at the 2018 Machine Learning for Healthcare conference at Stanford University, MIT Media Lab researchers have detailed a novel machine-learning technique to improve the quality of life for patients by reducing toxic chemotherapy and radiotherapy dosing for glioblastoma, the most aggressive form of brain cancer. The “self-learning” machine-learning technique looks at the current treatment regimens in use and iteratively adjusts the doses, eventually finding an optimal treatment plan, with the lowest possible potency and frequency of doses that should still reduce tumor sizes to a degree comparable to that of traditional regimens.
In simulated trials of 50 patients, the machine-learning model designed treatment cycles that reduced the potency to a quarter or half of nearly all the doses while maintaining the same tumor-shrinking potential. It skipped doses altogether several times and scheduled administrations only twice a year instead of monthly.
The model is a major improvement over the conventional “eye-balling” method of administering doses, observing how patients respond, and adjusting accordingly, according to Nicholas J. Schork, a professor and director of human biology at the J. Craig Venter Institute, and an expert in clinical trial design. “[Humans don’t] have the in-depth perception that a machine looking at tons of data has, so the human process is slow, tedious, and inexact,” he said. “Here, you’re just letting a computer look for patterns in the data, which would take forever for a human to sift through, and use those patterns to find optimal doses.”
According to Schork, the work could be of particular interest to the US FDA, which is currently looking for ways to leverage data and artificial intelligence to develop health technologies. Regulations still need be established, he said, “but I don’t doubt, in a short amount of time, the FDA will figure out how to vet these [technologies] appropriately, so they can be used in everyday clinical programs.”
Related Links:
Massachusetts Institute of Technology
In a paper presented at the 2018 Machine Learning for Healthcare conference at Stanford University, MIT Media Lab researchers have detailed a novel machine-learning technique to improve the quality of life for patients by reducing toxic chemotherapy and radiotherapy dosing for glioblastoma, the most aggressive form of brain cancer. The “self-learning” machine-learning technique looks at the current treatment regimens in use and iteratively adjusts the doses, eventually finding an optimal treatment plan, with the lowest possible potency and frequency of doses that should still reduce tumor sizes to a degree comparable to that of traditional regimens.
In simulated trials of 50 patients, the machine-learning model designed treatment cycles that reduced the potency to a quarter or half of nearly all the doses while maintaining the same tumor-shrinking potential. It skipped doses altogether several times and scheduled administrations only twice a year instead of monthly.
The model is a major improvement over the conventional “eye-balling” method of administering doses, observing how patients respond, and adjusting accordingly, according to Nicholas J. Schork, a professor and director of human biology at the J. Craig Venter Institute, and an expert in clinical trial design. “[Humans don’t] have the in-depth perception that a machine looking at tons of data has, so the human process is slow, tedious, and inexact,” he said. “Here, you’re just letting a computer look for patterns in the data, which would take forever for a human to sift through, and use those patterns to find optimal doses.”
According to Schork, the work could be of particular interest to the US FDA, which is currently looking for ways to leverage data and artificial intelligence to develop health technologies. Regulations still need be established, he said, “but I don’t doubt, in a short amount of time, the FDA will figure out how to vet these [technologies] appropriately, so they can be used in everyday clinical programs.”
Related Links:
Massachusetts Institute of Technology
Latest Industry News News
- Hologic Acquires UK-Based Breast Surgical Guidance Company Endomagnetics Ltd.
- Bayer and Google Partner on New AI Product for Radiologists
- Samsung and Bracco Enter Into New Diagnostic Ultrasound Technology Agreement
- IBA Acquires Radcal to Expand Medical Imaging Quality Assurance Offering
- International Societies Suggest Key Considerations for AI Radiology Tools
- Samsung's X-Ray Devices to Be Powered by Lunit AI Solutions for Advanced Chest Screening
- Canon Medical and Olympus Collaborate on Endoscopic Ultrasound Systems
- GE HealthCare Acquires AI Imaging Analysis Company MIM Software
- First Ever International Criteria Lays Foundation for Improved Diagnostic Imaging of Brain Tumors
- RSNA Unveils 10 Most Cited Radiology Studies of 2023
- RSNA 2023 Technical Exhibits to Offer Innovations in AI, 3D Printing and More
- AI Medical Imaging Products to Increase Five-Fold by 2035, Finds Study
- RSNA 2023 Technical Exhibits to Highlight Latest Medical Imaging Innovations
- AI-Powered Technologies to Aid Interpretation of X-Ray and MRI Images for Improved Disease Diagnosis
- Hologic and Bayer Partner to Improve Mammography Imaging
- Global Fixed and Mobile C-Arms Market Driven by Increasing Surgical Procedures
Channels
Radiography
view channel
Novel Breast Imaging System Proves As Effective As Mammography
Breast cancer remains the most frequently diagnosed cancer among women. It is projected that one in eight women will be diagnosed with breast cancer during her lifetime, and one in 42 women who turn 50... Read more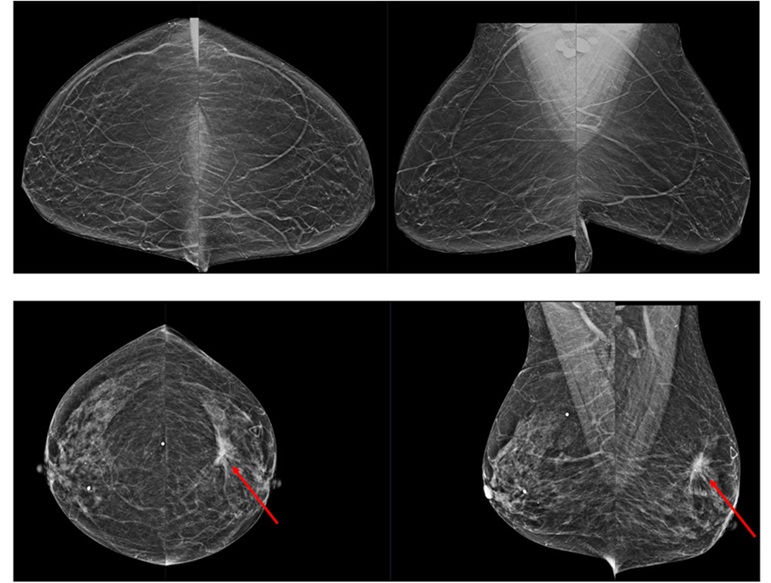
AI Assistance Improves Breast-Cancer Screening by Reducing False Positives
Radiologists typically detect one case of cancer for every 200 mammograms reviewed. However, these evaluations often result in false positives, leading to unnecessary patient recalls for additional testing,... Read moreMRI
view channel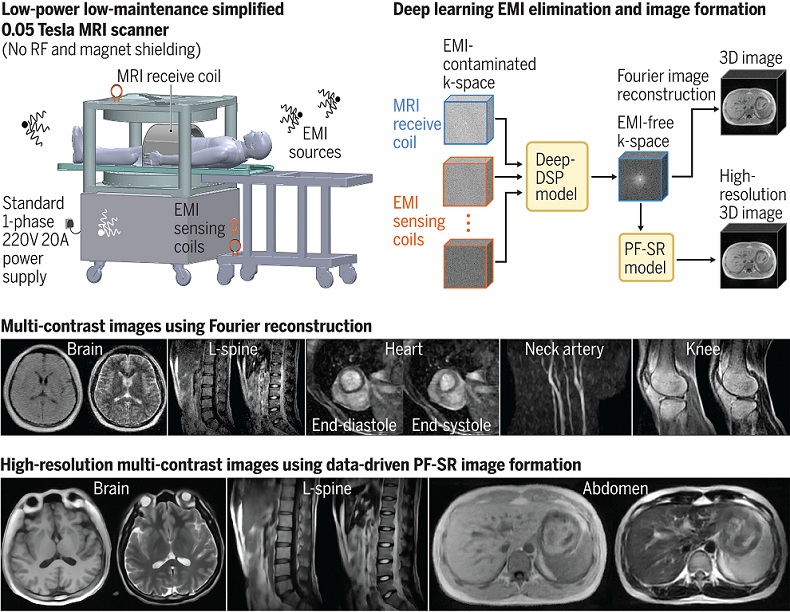
Low-Cost Whole-Body MRI Device Combined with AI Generates High-Quality Results
Magnetic Resonance Imaging (MRI) has significantly transformed healthcare, providing a noninvasive, radiation-free method for detailed imaging. It is especially promising for the future of medical diagnosis... Read more
World's First Whole-Body Ultra-High Field MRI Officially Comes To Market
The world's first whole-body ultra-high field (UHF) MRI has officially come to market, marking a remarkable advancement in diagnostic radiology. United Imaging (Shanghai, China) has secured clearance from the U.... Read moreUltrasound
view channel.jpg)
Diagnostic System Automatically Analyzes TTE Images to Identify Congenital Heart Disease
Congenital heart disease (CHD) is one of the most prevalent congenital anomalies worldwide, presenting substantial health and financial challenges for affected patients. Early detection and treatment of... Read more
Super-Resolution Imaging Technique Could Improve Evaluation of Cardiac Conditions
The heart depends on efficient blood circulation to pump blood throughout the body, delivering oxygen to tissues and removing carbon dioxide and waste. Yet, when heart vessels are damaged, it can disrupt... Read more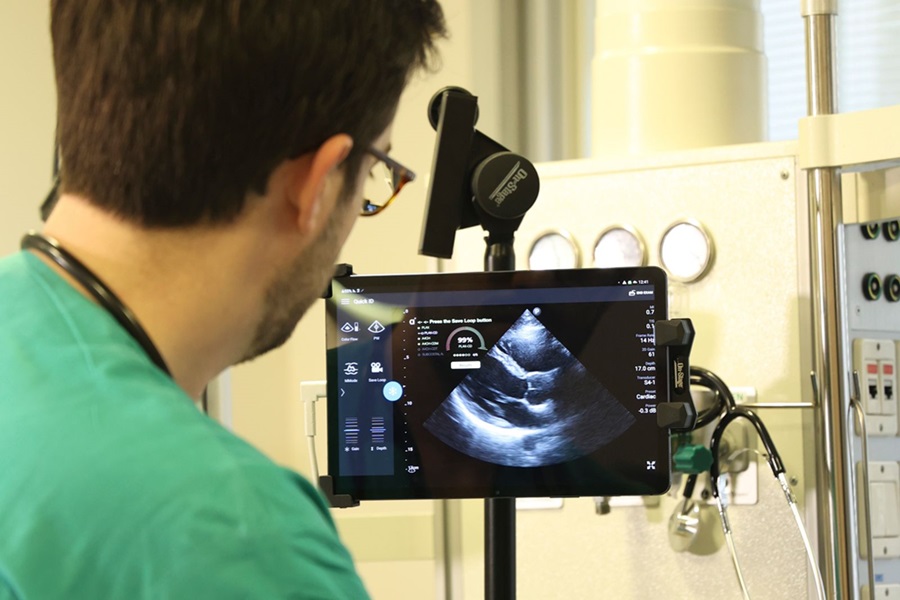
First AI-Powered POC Ultrasound Diagnostic Solution Helps Prioritize Cases Based On Severity
Ultrasound scans are essential for identifying and diagnosing various medical conditions, but often, patients must wait weeks or months for results due to a shortage of qualified medical professionals... Read moreNuclear Medicine
view channel
New PET Biomarker Predicts Success of Immune Checkpoint Blockade Therapy
Immunotherapies, such as immune checkpoint blockade (ICB), have shown promising clinical results in treating melanoma, non-small cell lung cancer, and other tumor types. However, the effectiveness of these... Read moreNew PET Agent Rapidly and Accurately Visualizes Lesions in Clear Cell Renal Cell Carcinoma Patients
Clear cell renal cell cancer (ccRCC) represents 70-80% of renal cell carcinoma cases. While localized disease can be effectively treated with surgery and ablative therapies, one-third of patients either... Read more
New Imaging Technique Monitors Inflammation Disorders without Radiation Exposure
Imaging inflammation using traditional radiological techniques presents significant challenges, including radiation exposure, poor image quality, high costs, and invasive procedures. Now, new contrast... Read more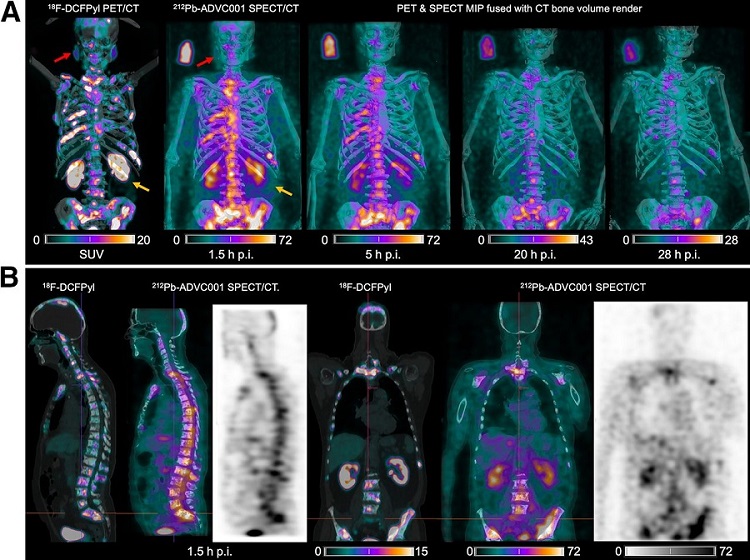
New SPECT/CT Technique Could Change Imaging Practices and Increase Patient Access
The development of lead-212 (212Pb)-PSMA–based targeted alpha therapy (TAT) is garnering significant interest in treating patients with metastatic castration-resistant prostate cancer. The imaging of 212Pb,... Read moreGeneral/Advanced Imaging
view channelBone Density Test Uses Existing CT Images to Predict Fractures
Osteoporotic fractures are not only devastating and deadly, especially hip fractures, but also impose significant costs. They rank among the top chronic diseases in terms of disability-adjusted life years... Read more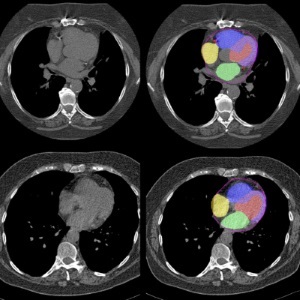
AI Predicts Cardiac Risk and Mortality from Routine Chest CT Scans
Heart disease remains the leading cause of death and is largely preventable, yet many individuals are unaware of their risk until it becomes severe. Early detection through screening can reveal heart issues,... Read moreImaging IT
view channel
New Google Cloud Medical Imaging Suite Makes Imaging Healthcare Data More Accessible
Medical imaging is a critical tool used to diagnose patients, and there are billions of medical images scanned globally each year. Imaging data accounts for about 90% of all healthcare data1 and, until... Read more